Case Presentation:
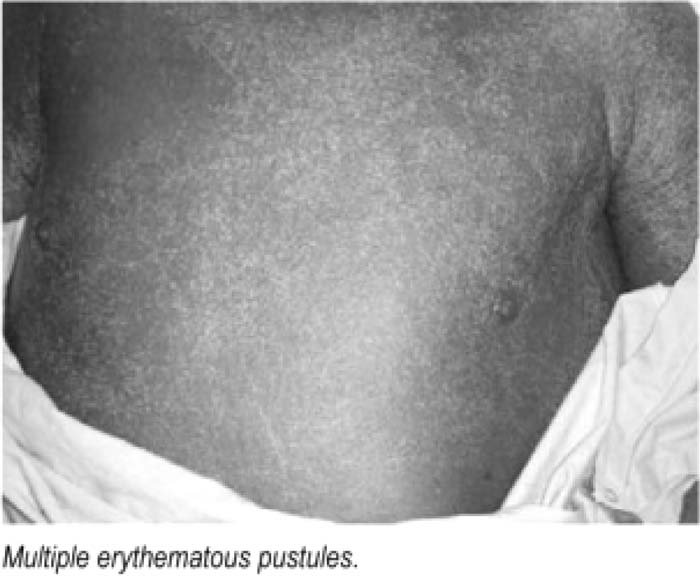
A 51‐year‐old male with history of diastolic heart failure, hypertension, MRSA bacteremia, and schizophrenia presented with desquamation of the skin that was initially a diffuse, pustular dermatitis of the body sparing the genitalia and back. He had been recently treated with ampicillin and sulbactam for a leg cellulitis. On admission, patient's labs were significant for leukocytosis with neutrophilia and elevated BUN and creatinine. Water loss from the skin desquamation later caused severe hypernatremia. The initial differential included TENS and Steven‐Johnson syndrome. He was initially treated with cefazolin because of the concern about TENS and Steven‐Johnson syndrome. A punch biopsy of the thigh was consistent with acute generalized exanthematous pustulosis (AGEP). The etiology was likely secondary to a beta‐lactam antibiotics exposure He was started on topical triamcinolone with improvement of the lesion.
Discussion:
In a recent review of AGEP. none of patients had a history of psoriasis or prior adverse drug reactions. AGEP developed after exposure to The causative agent in 2‐9 days, with a mean of 5.1 days. Etiologic agenls include anticonvulsants (mainly carbamazepine), antimicrobials mainly beta‐lactams, calcium channel blockers, and viral infection. Lesions usually start on the face and neck with infrequent mucous membrane involvement. Associated features include itching, fever, facial edema, and peripheral neutrophilia. Dermatologic manifestations include edematous erythema or scarlatinoid exanthema, which is quickly covered with numerous small pustules (< 5 mm), mainly nonfollicular and superficial. Hislopathology includes subcomai pustules, inflammatory perivascular polymorphonuclear infiltrate with eosinophilic predominance, and focal necrosis of keratinocytes. AGEP seems to be an immune reaction, with specific T cells producing large amounts of neutrophil‐attracting cytokines. Differential diagnoses include pustular psoriasis. Sweets syndrome, erythema multiforme, TEN, and anticonvulsive hypersensitivity syndrome. The symptoms usually resolve spontaneously within 2 weeks and respond well to steroids (topical or systemic); residual shedding is invariably observed. Supportive care, including aggressive skin hygiene, water maintenance, and infection surveillance may be needed depending on the areas involved.
Conclusions:
AGEP is a rare skin eruption, associated principally with drugs mainly anticonvulsants and antimicrobials and acute viral infections. Early recognition can help to differentiate from pustular psoriasis and infectious causes to avoid unnecessary diagnostic studies and treatments (including antibiotics).
Author Disclosure:
P. Sharma, none; S. Kandpal, none; R. Bahuva, none.