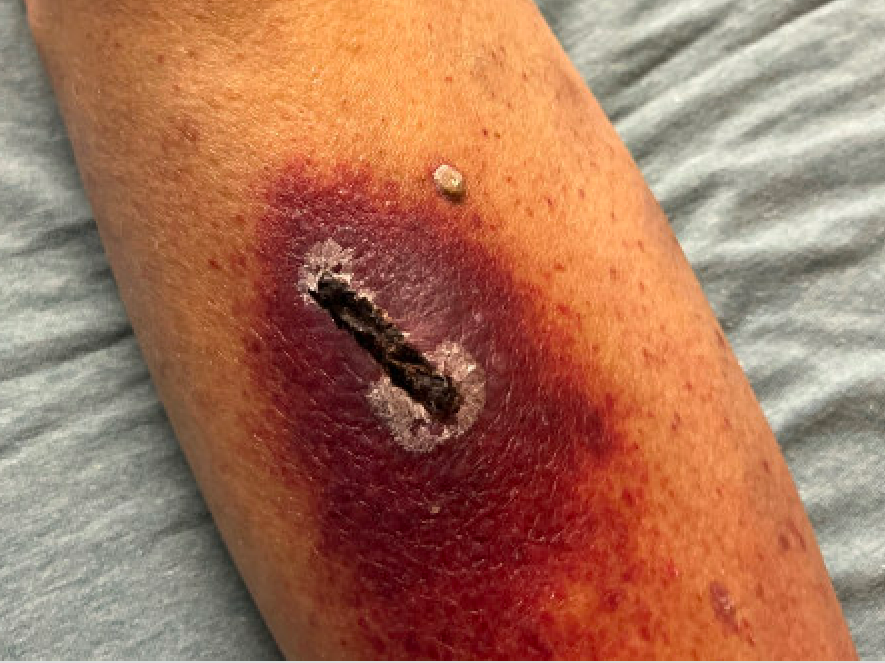
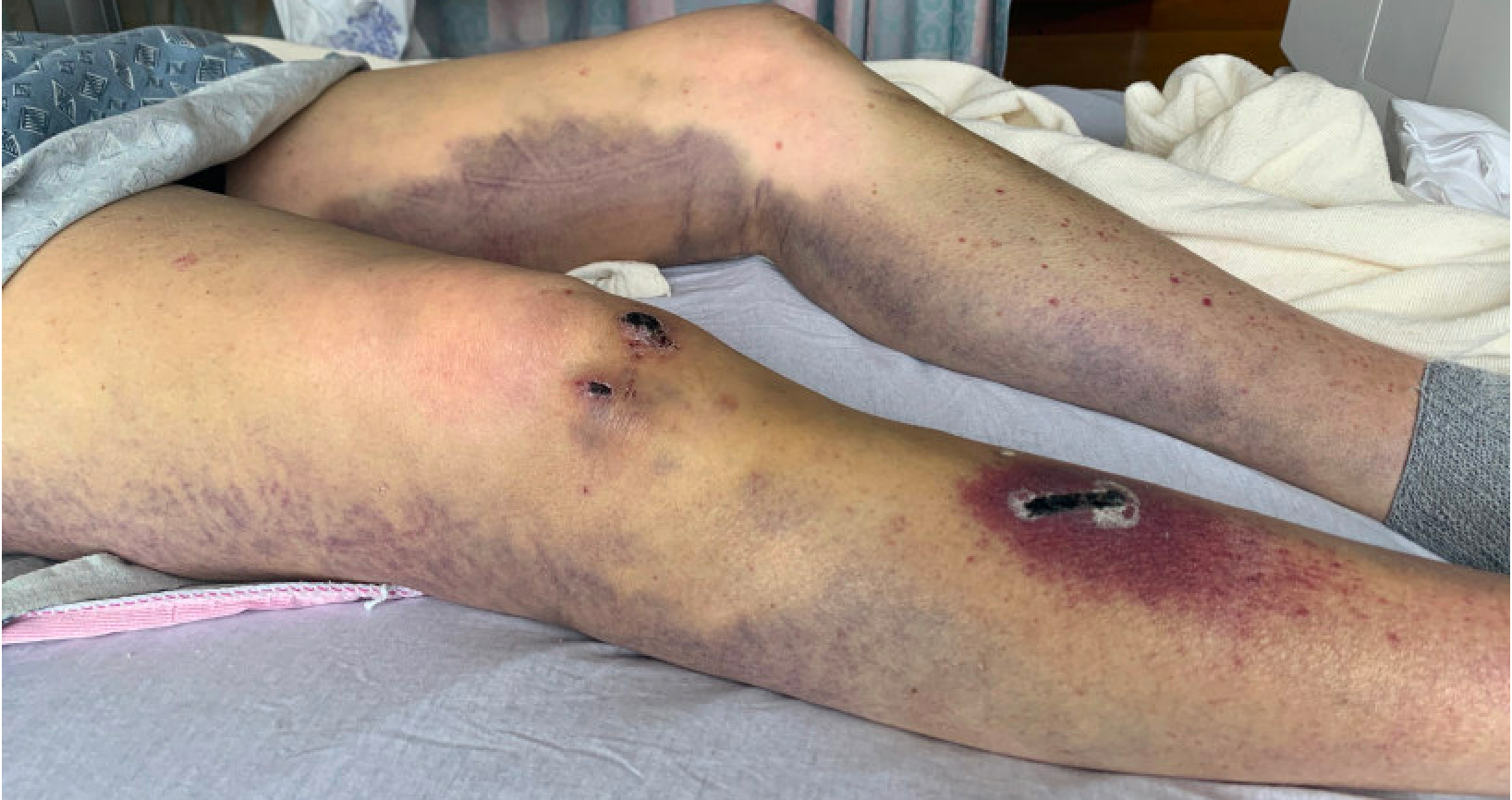
Case Presentation: A Caucasian man in his 60s presented to the ED with a 6-week history of extensive bruising, worse in both legs and buttocks, along with shortness of breath on minimal exertion. He stated he had a chronic wound on his right leg (Figure 1). He was not taking any regular medications. Days later he endorsed having 4 standard drinks daily, along with slight bleeding of gums when brushing his teeth, prolonged bleeding of 45 minutes following tooth extraction, and decreased appetite over the last few months. Examination revealed extensive confluent ecchymosis, hematomas, and petechiae in the dependent portions of bilateral lower extremities (Figure 2) and pale skin and conjunctivae. There was no lymphadenopathy, splenomegaly or stigmata of chronic liver disease. Examination revealed labored breathing, dyspnea, and tachycardia. Given shortness of breath and elevated D-dimer (478 ng/mL), CTPE was ordered showing a small subsegmental PE. Due to extensive ecchymosis and anemia (Hb 12.1 g/dL) an abdominal ultrasound was ordered for possible bleeding diathesis, but was normal. Since the patient presented with signs of both hypercoagulability and bleeding, various differential diagnoses were considered. DIC was ruled out due to peripheral smear without schistocytes and labs showing lack of thrombocytopenia, normal haptoglobin, and normal PTT/INR. Von Willebrand Disease was considered given normal platelet count (307 x 10exp9/L) in the setting of extensive bruising and petechiae, but further work-up demonstrated normal von willebrand antigen, factor VIII activity, ristocetin activity, and platelet function assay. Given heavy alcohol use, a clotting factor deficiency secondary to liver disorder was considered. Workup revealed normal liver function tests. Eventual lab work showing profoundly low Vitamin C levels (< 5umol/L) confirmed a diagnosis of scurvy. The patient was treated with anticoagulation for his PE with monitoring for additional bleeding. He received supplementation with vitamin C and was referred to hematology for follow up.
Discussion: Although uncommon in modern medicine, scurvy should be considered in patients with unexplained bruising and bleeding, especially if they endorse a restrictive diet and/or use alcohol excessively. Since humans cannot synthesize vitamin C, exogenous dietary sources of Vitamin C, like fruits and vegetables, are needed (1,2). Without these sources, scurvy symptoms can develop in as little as 4 weeks (1). Initial symptoms may be non-specific and include lethargy, malaise, weakness, anorexia, and depressed mood (1,2,3). Subsequent clinical features stemming from defective collagen synthesis leading to lack of vessel wall integrity include dermatologic and musculoskeletal bleeding, “corkscrew” hairs, and myalgias and arthralgias (1,3). Perifollicular hemorrhages and purpura affecting the dependent portion of the legs are common areas of bleeding, as seen in our patient (1,3). If left untreated, scurvy can progress to fatal bleeding within essential organs (1,3). Scurvy is treated with supplementation of vitamin C (300 to 1000 mg orally daily for one month) (1,2,3).
Conclusions: Hospitalists should consider scurvy in patients with poor diets and/or excessive alcohol use with dermatological and musculoskeletal findings, like hematomas, petechiae, and poor wound healing. This case mimicked a coagulation disorder with both physical exam, imaging, and lab findings which led to delayed diagnosis and high resource expenditure.