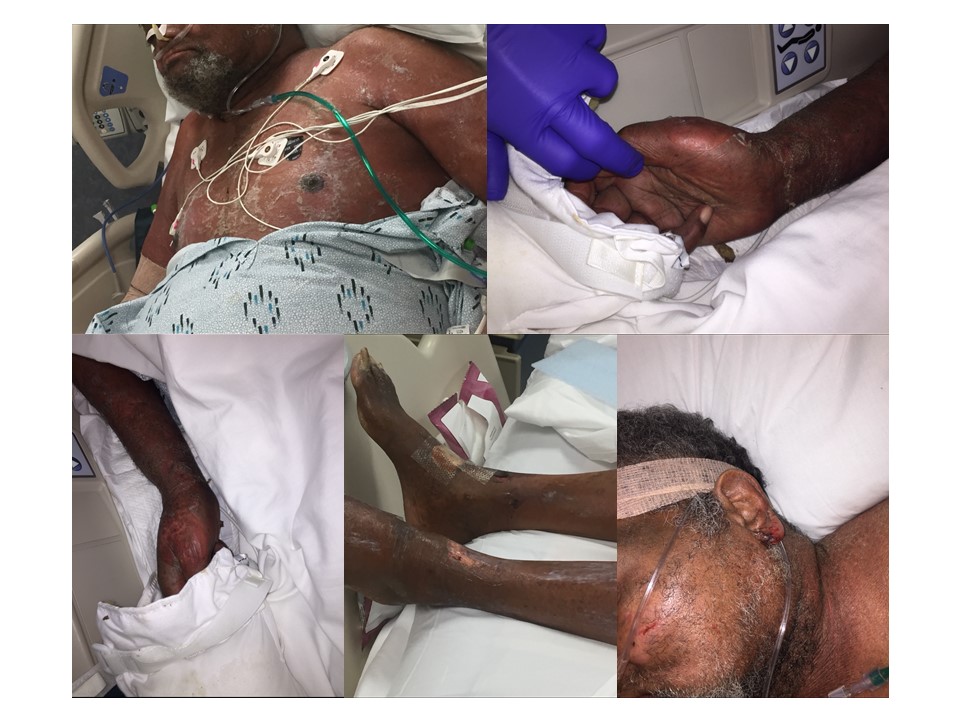
Case Presentation: A 74-year-old man with coronary artery disease, sick sinus syndrome with biventricular PPM/ICD, HFrEF (EF 45%), and diabetes. He presented to the hospital with five days of worsening substernal chest pain and troponin elevation concerning for a NSTEMI. Urgent left heart catheterization showed multivessel disease and he subsequently underwent three vessel CABG. His post-operative course was complicated by acute hypoxic respiratory failure secondary to multidrug resistant Enterobacter cloacae pneumonia requiring intubation and acute renal failure requiring initiation of hemodialysis.Amidst these complications, he developed a rapidly progressive, painful, full body desquamative skin rash. His skin exam was notable for diffuse erythema, shallow erosions and ulcers, and superficial desquamation that spared the palms, soles, and mucosal surfaces. Nikolsky sign was positive. Skin biopsy showed subcorneal splitting of the epidermis without evidence of bacterial or neutrophilic invasion. A diagnosis of Staph Scalded Skin Syndrome (SSSS) was made based on the biopsy and clinical history. The patient was treated with IV vancomycin and clindamycin with improvement of the rash and crusting over two weeks.
Discussion: SSSS is caused by infection with exfoliative exotoxin producing strains of Staphylococcus aureus. Hematogenous spread of the exotoxin from the initial focus of S. aureus infection cleave desmoglein-1, a protein responsible for keratinocyte adhesion in the upper layers of the epidermis. Staph scalded skin syndrome is a rare disease in adults, with an estimated incidence of less than 1:1,000,000. It typically occurs in immunocompromised patients, patients with renal impairment, and diabetics. Sites of infection are often not evident for patients with SSSS as seen in our patient who only had Staph aureus in the nares upon discharge. Cultures should be taken from sites with purulence or as in our case from common sites of S. aureus colonization such as the nares. It is important to distinguish SSSS from other etiologies of blistering and desquamative rashes, particularly Stevens Johnson Syndrome/Toxic Epidermal Necrolysis (SJS/TEN) and pemphigus foliaceus. SJS/TEN is often drug-induced and requires prompt discontinuation of the causative drug. SJS/TEN may respond to immunosuppressive therapy while antibiotics are the cornerstone of treatment for SSSS. SJS/TEN typically involves the mucosa, while SSSS is mucosa-sparing, as in our patient. Histopathology of SJS/TEN shows full thickness necrosis of the epidermis, while SSSS characteristically shows subcorneal splitting of the epidermis. Pemphigus foliaceus is an autoimmune skin disorder in which autoantibodies bind to desmoglein-1, leading to separation of the upper layers of the epidermis. Most cases of Pemphigus foliaceus are idiopathic but may also be precipitated by drugs such as angiotensin-converting enzyme inhibitors. Pemphigus foliaceus is indistinguishable from SSSS on skin biopsy, but typically presents on the face and scalp with rare extension to the whole body.
Conclusions: Staph scalded skin syndrome is a rare disease entity among adults that typically impacts patients with renal dysfunction or other immune compromise. It can be distinguished from other causes of a desquamative skin rash by physical exam and histopathology. Accurate diagnosis is imperative, given the dichotomy in treatment approach between Staph Scalded Skin Syndrome and other causes of desquamative rash, such as Toxic Epidermal Necrolysis.