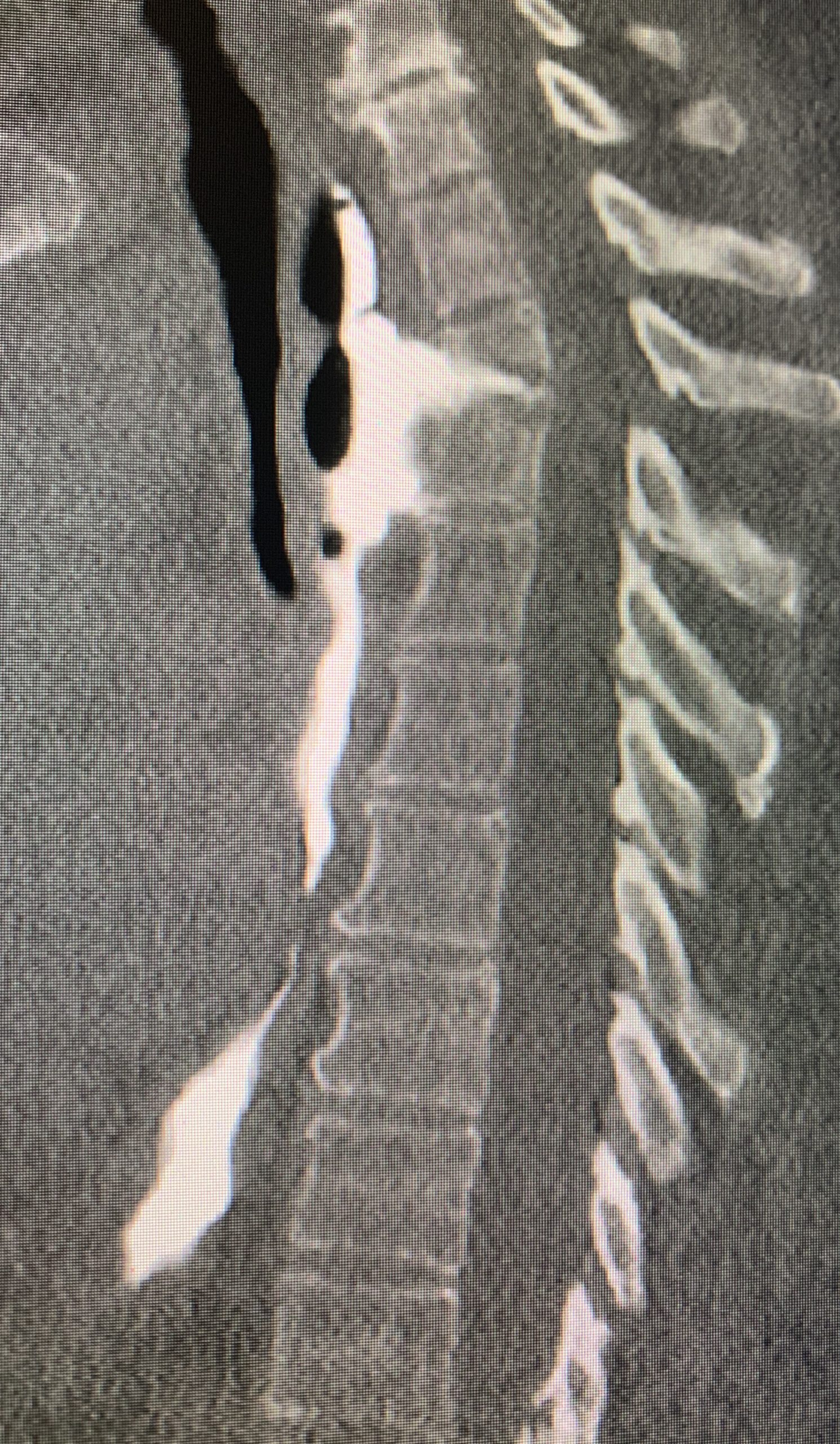
Case Presentation: Epidural-Esophageal fistula is an uncommon adverse event after esophageal perforation. The presenting symptoms may mimic other more common conditions, which may lead to incorrect diagnosis. We present a patient with esophageal perforation of unknown etiology, complicated by spinal epidural abscess.52-year-old female with a history of liver cirrhosis secondary to hepatitis C, endometrial carcinoma with metastasis to lung for which she received radiation therapy, hypertension and diabetes mellitus presented to the hospital with cough, fever and shortness of breath. Computer tomography scan (CT) showed a loculated effusion and a thoracostomy tube was placed. Microbiology cultures from the chest tube showed infection with GDS, Klebsiella, Eubacterium, VSE. She received vancomycin and unasyn, and the thoracostomy was removed. Subsequently, the patient developed acute back pain that prompted to get a magnetic resonance imaging (MRI) showing destruction of the endplates at T2-T3, a paravertebral and epidural abscess as well as an esophageal leak at the same level. Barium esophagogram revealed a 3.5 cm contained leak of the mid-upper esophagus. Antibiotic therapy with cefepime was started. Since the esophageal leak was contained and patient did not have any neurologic complaints at the time, the decision was made for no surgical intervention. An esophageal/endoluminal wound vac (WV) and PEG tube was placed as well, in an attempt to seal the leak and bypass the defect.
Discussion: Esophageal fistula presenting as epidural abscess has been reported to be a rare complication ofesophageal dilation, stent placement/removal, endoscopy and radiation. Management of epidural abscess depends on the severity and presence of neurologic symptoms. Certain patients can be conservatively treated with medical management alone, where antibiotics are the mainstem treatment . Clinical suspicion and early medical therapy or surgical management with indicated are the most important factors to have in mind when managing these patients.
Conclusions: Our case highlights the existence of esophageal fistulas, complicated by epidural abscess which is an uncommon complication, but in the presence of back pain and neurological symptoms, a CT scan or MRI should be pursued in order to have a prompt diagnosis and start early treatment strategies with the aim to reduce complications and improve clinical outcomes.