Background: Although systemic antibiotics are essential for treating infections, they can also have adverse side effects such as toxicity, allergic reactions, or resistance, which can significantly increase morbidity and mortality. This study examined mortality patterns and inequalities linked to adverse effects of systemic antibiotics between 1999 and 2020.
Methods: Analysis of Systemic Antibiotics Adverse Effects-related deaths in adults (≥25 years) in the U.S. from 1999-2020 was conducted using death certificate data from the CDC WONDER database, utilizing the ICD-10 code Y-40. Age-adjusted mortality rates (AAMR) per 1,000,000 population were extracted, and trends were analyzed using Joinpoint regression to calculate the Average Annual Percent Change (AAPC) with a p-value for statistical significance. Data were stratified using year, gender, race/ethnicity, and geographical regions.
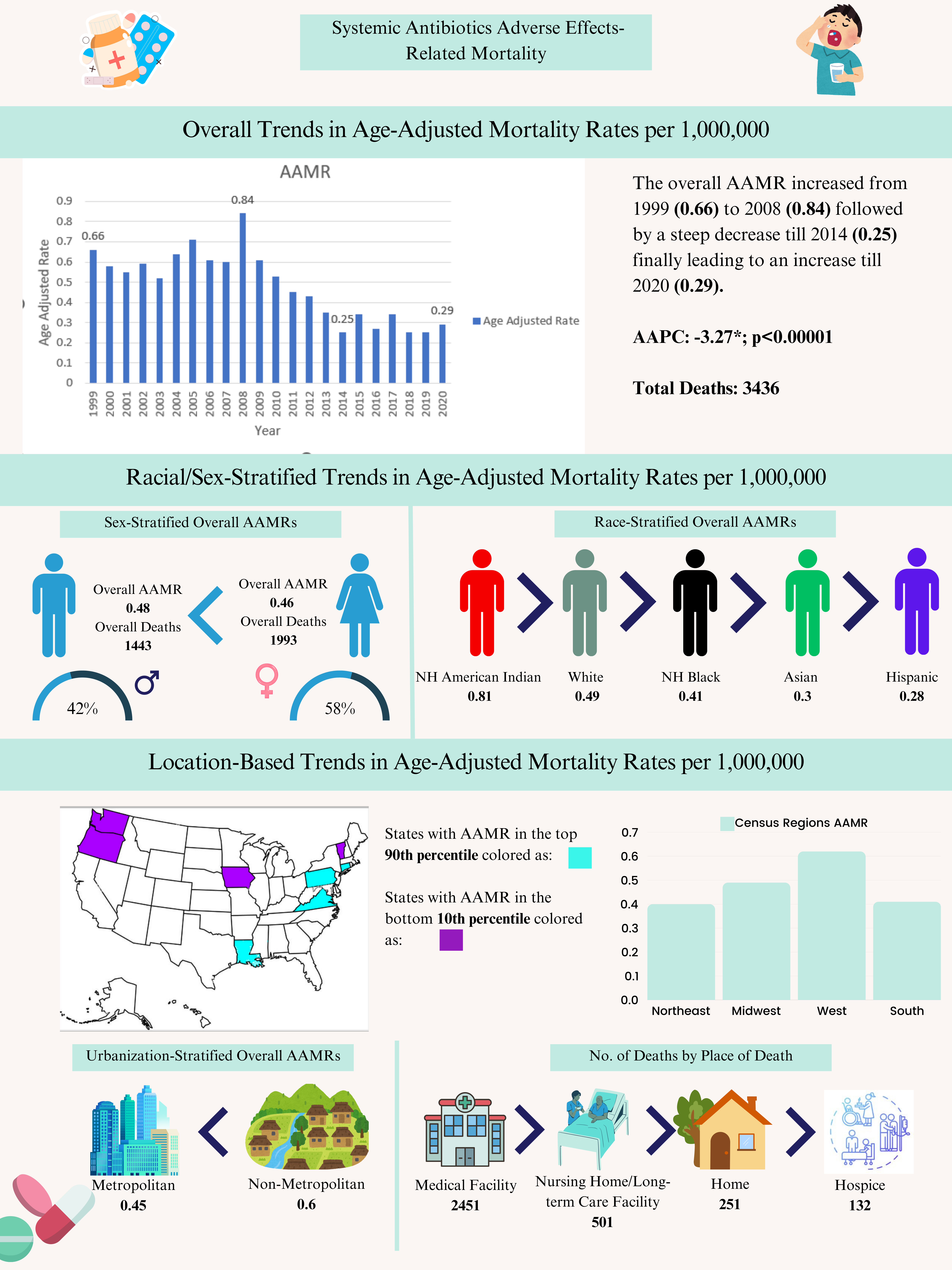
Results: Between 1999 and 2020, Antibiotic Therapy Adverse Effects caused 3436 deaths among U.S. older adults aged ≥25 years. Most deaths occurred in medical facilities (71%) and at decedent’s homes (14.6%). The overall AAMR for Systemic Antibiotics Adverse Effects-related deaths decreased from 0.66 in 1999 to 0.29 in 2020, with an AAPC of -3.27* (p < 0.000001). Men showed higher AAMRs than women (0.48 vs. 0.46), with a more pronounced decrease in women (AAPC: -5.09*, p < 0.000001), compared to men (AAPC: -3.08*, p < 0.000001). Racial disparities were significant, with American Indians or Alaska Natives having the highest AAMR (0.81), followed by Whites (0.49), Black individuals (0.41), Asians or Pacific Islanders (0.3), and Hispanics (0.28). The decline in AAMR throughout the study was most pronounced in Whites (AAPC: -3.15*, p < 0.000001). Geographically, Vermont had the highest AAMRs (2.22) and the lowest in Louisiana (0.19). The Western U.S. had the highest regional AAMR (0.62), followed by the Midwest (0.49), South (0.41), and Northeast (0.40). Nonmetropolitan areas had higher AAMRs than metropolitan areas, though metropolitan areas showed significant declines from 1999 to 2020 (Metropolitan: AAPC: -3.39*, p < 0.000001).
Conclusions: Over the past two decades, mortality related to adverse reactions from systemic antibiotics has lessened. Still, it shows disparities in men, American Indians, and nonmetropolitan areas, with the Western U.S. showing the most tremendous regional increase. These findings underline the necessity for precise prescribing practices, patient education, and enhanced monitoring to reduce adverse outcomes in high-risk groups.