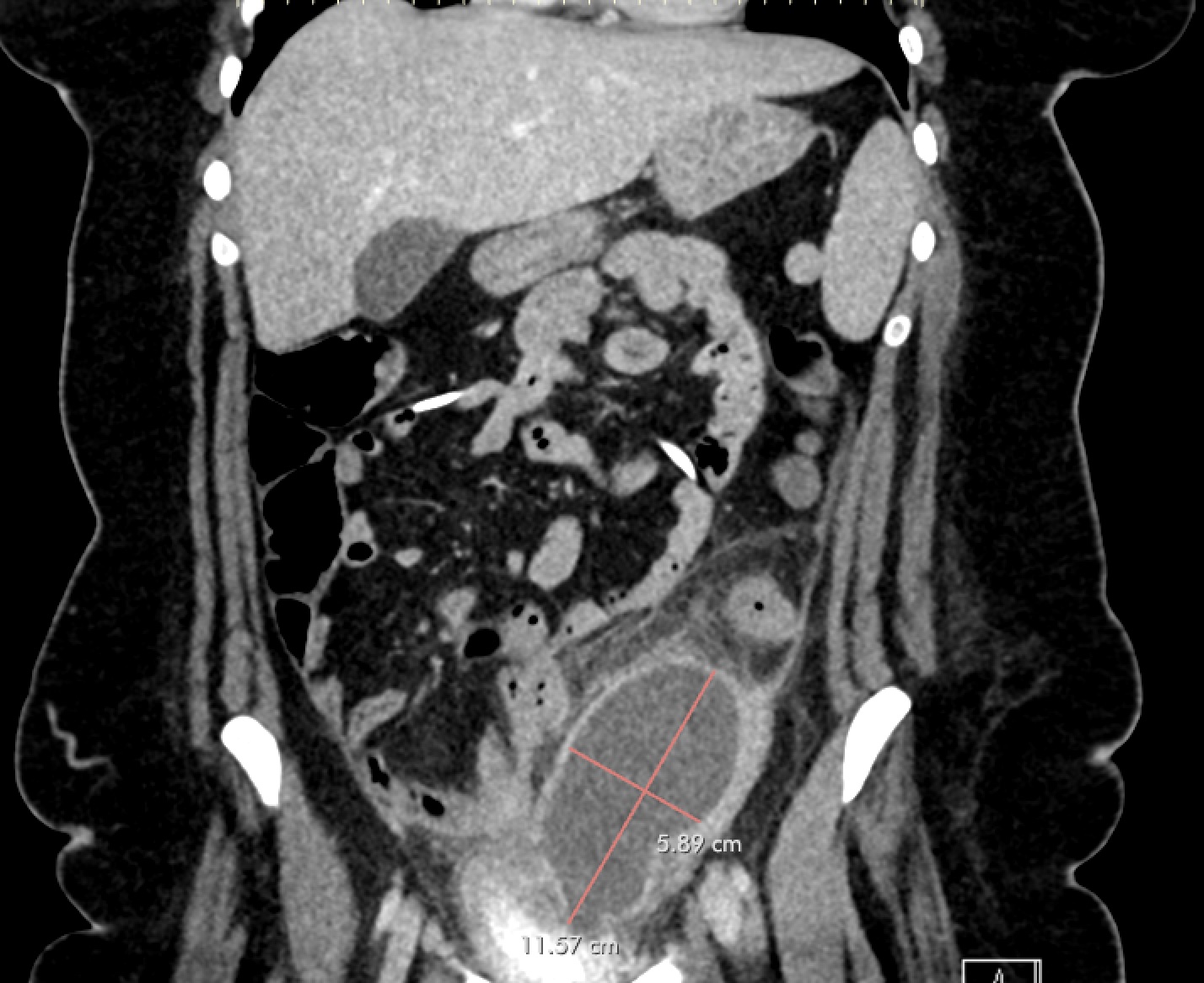
Case Presentation: A 22-year-old female with PMH of TBI with resultant hydrocephalus s/p VP shunt placement and borderline personality disorder presented with three weeks of progressively worsening abdominal pain. She also reported a new onset of vaginal bleeding for 3 days, which was different from her usual amenorrhea secondary to IUD placement. The exam was significant for tenderness to palpation in the left lower quadrant without rebound or guarding. Laboratory evaluation was significant for normal WBCs with neutrophilic predominance. CT abdomen/pelvis demonstrated a large, rim-enhancing intraabdominal fluid collection adjacent to the sigmoid colonic wall, concerning for abscess, as well as coiling of the intraabdominal portion of the VP shunt. General surgery was consulted and recommended Interval Radiology consult for drain placement. Due to location of the abscess and new vaginal bleeding, gynecology was consulted for concern for pelvic inflammatory disease and tubo-ovarian abscess. In discussion with the gynecology team, the patient reported high risk sexual activity with multiple partners in the last year with intermittent use of protection. A pelvic exam was completed and was without cervical motion tenderness or mucopurulent discharge. A transvaginal ultrasound was obtained with redemonstration of the intraabdominal fluid collection. She was started on antibiotics with cefoxitin and doxycycline for concern for pelvic inflammatory disease (PID) leading to tubo-ovarian abscess (TOA) and was admitted for further work-up and monitoring of this intraabdominal abscess. IR was consulted and a drain was placed into the fluid collection. Cultures of the fluid resulted with Hemophilus influenza, beta lactamase negative. She continued on cefoxitin and doxycycline and was stable for discharge to home to complete a 14-day course of doxycycline and metronidazole and follow-up with general surgery for drain management/removal.
Discussion: PID and its complications, such as TOA, are often attributed to sexually transmitted infections and known colonizers of the genitourinary tract, but other organisms have been associated with TOA and should be considered as a potential cause. Haemophilus influenza has been described in the literature to be a rare cause of TOA, yet the reports reviewed indicate a significant inflammatory response with fever and leukocytosis to the TOA, which was not present in our patient presenting with isolated left lower quadrant pain. Haemophilus is commonly thought of as a respiratory tract organism but can be involved in extrapulmonary disease, including TOA, cholecystitis, meningitis and more.
Conclusions: Hemophilus influenza should be considered as a cause of invasive infection, including PID and TOA, and while not applicable in the case of our patient, may change the standard management due to increasing prevalence of beta-lactamase resistance. Lack of improvement on standard antimicrobial therapies should prompt consideration for alternative therapies.