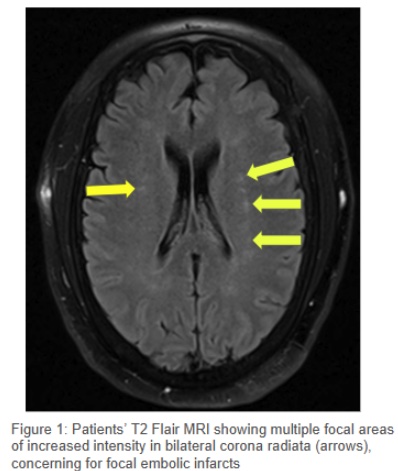
Case Presentation: A 56-year-old man was found unresponsive at home during a wellness check. Paraphernalia and the condition of other patients at the scene suggested a drug overdose. In the emergency department, his vital signs were HR 136 bpm, BP 164/90 mmHg, RR 22, and SpO2 94% on room air. Due to severe agitation, physical restraints and one-time doses of haloperidol and lorazepam were administered. A urine drug screen was positive for cocaine. Initial labs revealed AKI (creatinine 2.32 mg/dL), rhabdomyolysis (CK >30,000 U/L), acute liver injury (AST 557 U/L, ALT 150 U/L), elevated troponin I (5.3 ng/mL), and hyperkalemia (K 6.3 mmol/L) with peaked T waves on ECG. Treatment included 3L IV fluids, calcium gluconate, and arrangements for continuous renal replacement therapy (CRRT). A CT head without contrast showed no acute findings. Chest X-ray revealed pulmonary edema, and BNP was elevated (1,720 pg/mL), suggesting acute decompensated heart failure. He developed hypoxemia (SpO2 70%) with apneic episodes and fluctuating somnolence and agitation. After failed attempts at supplemental oxygen, he was intubated and sedated. With treatment, renal function slowly improved, troponin resolved in a pattern consistent with type 2 NSTEMI, liver injury normalized, and hyperkalemia corrected with CRRT. After extubation, he was unable to move his left arm. MRI of the left brachial plexus revealed acute plexopathy, and brain MRI showed bilateral embolic infarcts. Transesophageal echocardiography (TEE) identified a 0.96 x 0.74 cm lesion on the aortic valve, consistent with a sessile fibroelastoma. Cardiology and cardiothoracic surgery recommended open-heart surgery, but the patient elected to pursue treatment in his home state. He was discharged to a suitable facility.
Discussion: Cardiac fibroelastomas are benign tumors most commonly affecting the aortic and mitral valves. While often asymptomatic, they are significant due to their strong association with embolic events such as cerebrovascular accidents (CVA) and transient ischemic attacks. The risk of embolic fragmentation is high, with some studies reporting new CVA incidence as high as 8.9%. Diagnosis can be challenging as transthoracic echocardiography may miss smaller lesions. TEE is more sensitive and should be pursued if suspicion remains. Definitive treatment involves surgical excision with valve preservation when possible. Patients who cannot undergo surgery are at increased risk of embolic complications, with one study noting a 13% CVA incidence over five years in untreated individuals. For non-surgical patients, long-term antiplatelet therapy is recommended.
Conclusions: Fibroelastomas are rare but clinically significant cardiac tumors associated with a high risk of embolic events. Surgical excision is the preferred management strategy, but for non-surgical candidates, long-term antiplatelet therapy and close monitoring are critical to reducing the risk of complications.