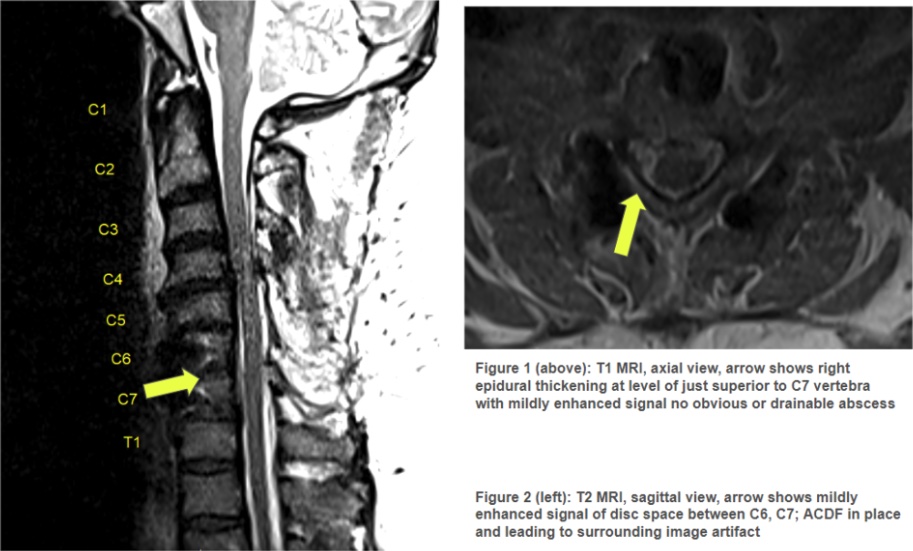
Case Presentation: A 55-year-old man with a history of obesity, gout, and multiple cervical spine surgeries, including a remote C4 laminectomy, C6-C7 fusion, and anterior cervical discectomy and fusion (ACDF) at C5-C7, presented for a higher level of care due to septic arthritis in his right knee. His medical history also included prolonged courses of methylprednisolone for chronic neck pain. At the referring hospital, knee aspiration revealed septic arthritis, prompting transfer. On arrival, orthopedic surgery performed an incision and drainage (I&D), and the patient was empirically started on vancomycin and cefepime. On postoperative day 1, blood cultures from the outside hospital showed gram-positive cocci in 2/2 bottles, and synovial fluid cultures grew Streptococcus equi subspecies equi. Antibiotic susceptibility testing confirmed sensitivity to ceftriaxone, leading to the de-escalation of therapy to ceftriaxone 2 g every 24 hours. Further history revealed indirect exposure to horses: the patient lived near a horse farm, and his dog frequently interacted with the horses before spending significant time indoors with the patient. This indirect contact was deemed the likely route of infection. Further evaluation for bacteremia revealed no vegetations on transesophageal echocardiography. However, an MRI identified discitis at C5-C7. The interdisciplinary team determined he was not a neurosurgical candidate, and he was recommended continuation of IV antibiotics. The patient was discharged on six weeks of ceftriaxone, followed by a planned transition to oral amoxicillin 500 mg every 8 hours for three months.
Discussion: Although Streptococcus equi is a rare human pathogen, it is a well-known cause of illness in domestic animals, predominately horses. It commonly causes “strangles,” a respiratory illness in horses characterized by cervical lymphadenopathy and increased nasal secretions. Although uncommon, zoonotic transmission of S. equi to humans has been reported in cases involving disseminated arthritis, meningitis, osteomyelitis, pneumonia, and endocarditis. Transmission is often through inhalation, cutaneous inoculation, or ingestion of contaminated materials such as unpasteurized dairy products. This case highlights the importance of considering zoonotic pathogens in patients with unusual infections and potential animal exposure. Multiple case reports in the literature demonstrate favorable resolution following successful multidisciplinary management, including source control and tailored antimicrobial therapy guided by susceptibility data.
Conclusions: Streptococcus equi should be recognized as a zoonotic pathogen when isolated from sterile sites such as blood or synovial fluid. Prompt initiation of antibiotics, de-escalation based on susceptibility testing, and consideration of infection severity and location are essential to management.