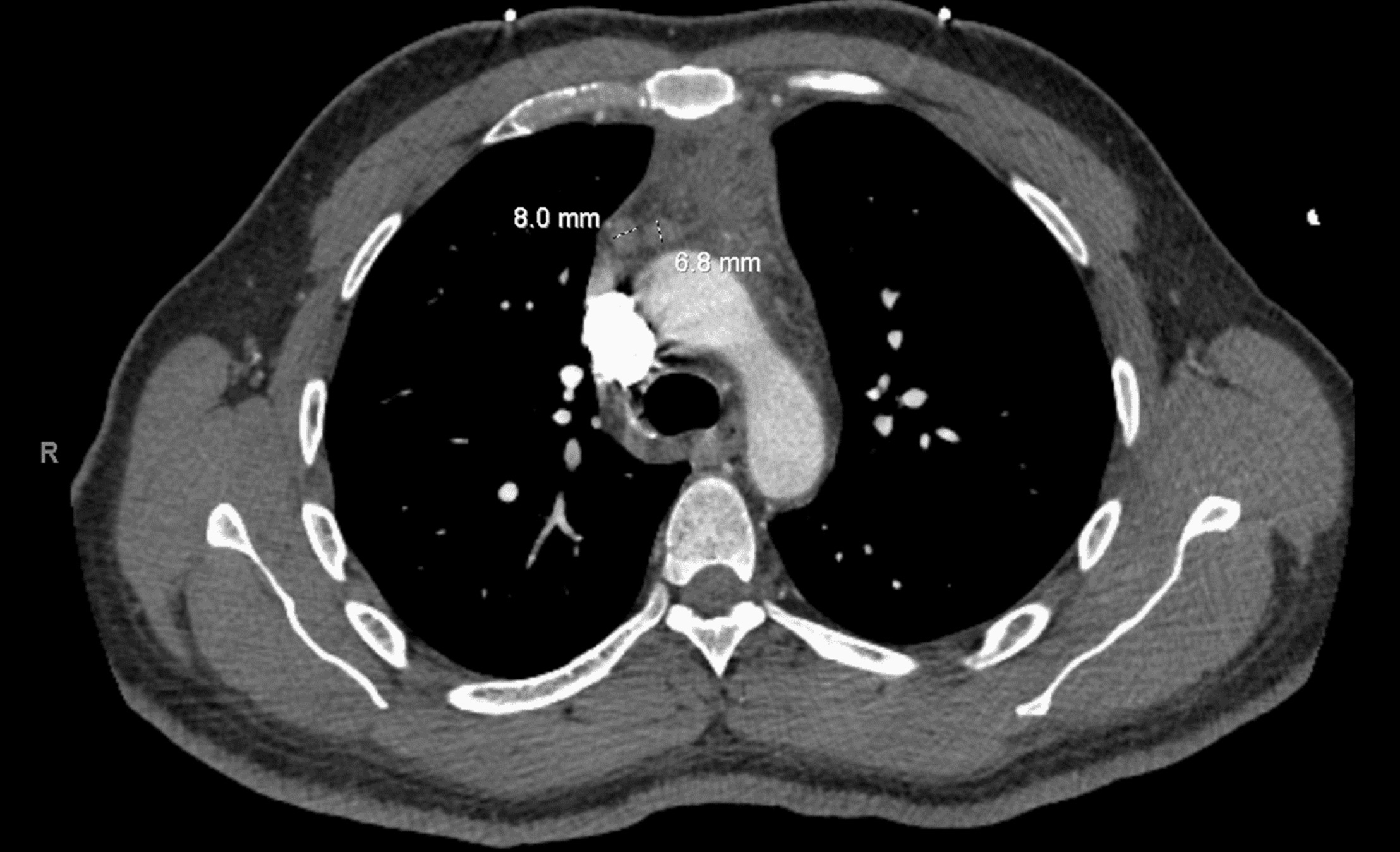
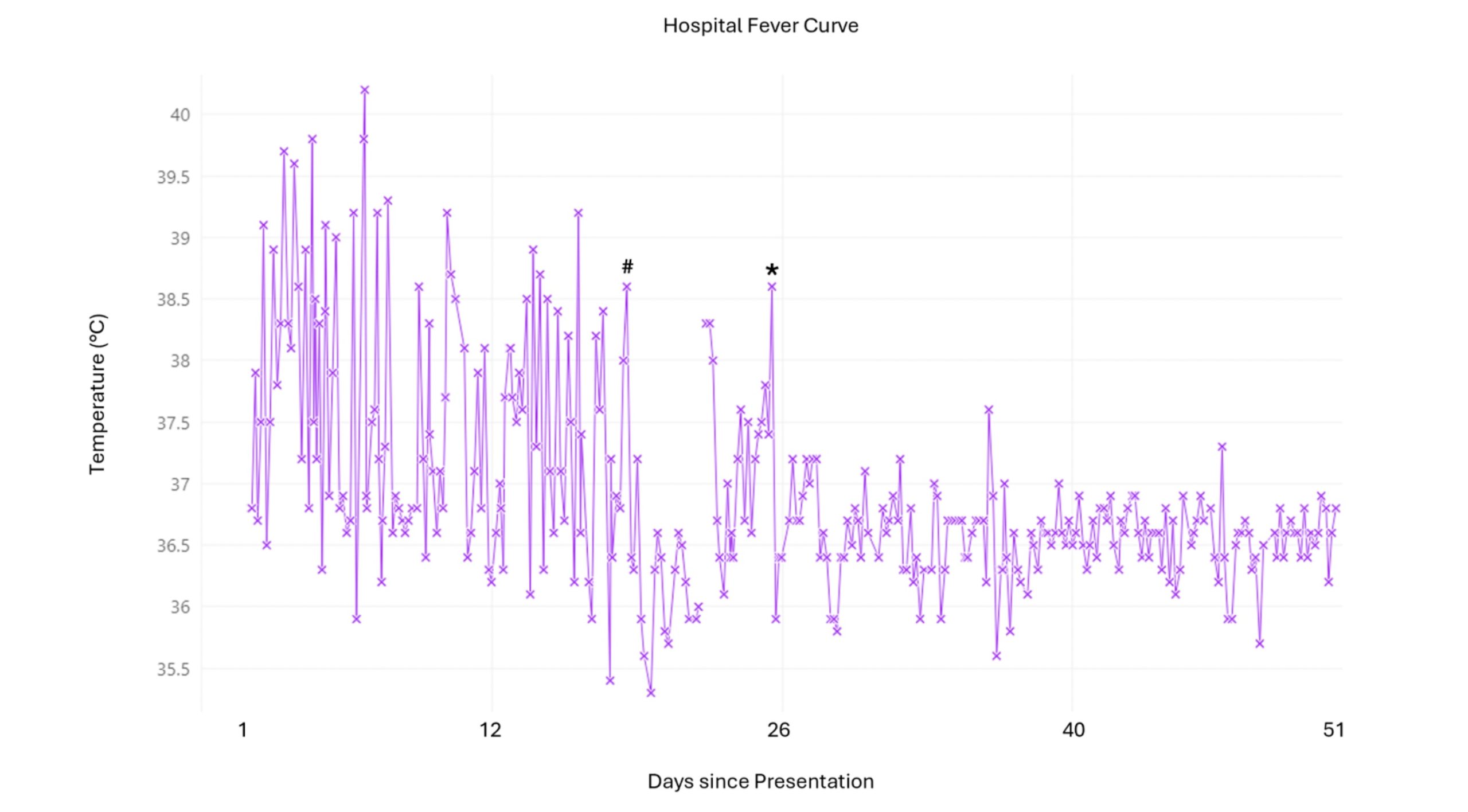
Case Presentation: We present a case of secondary Hemophagocytic Lymphohistiocytosis (HLH) triggered by Epstein-Barr Virus (EBV) in a 49 old male with no significant past medical history who worked as a cruise ship crewmember, presenting with high grade fevers and night sweats. Given his occupation, a broad differential diagnosis was initially considered, complicating timely diagnosis. From the initial testing, the patient was only positive for EBV IgG at a low titer. The patient continued with high fevers and developed acute liver failure which was treated with high dose steroids. Subsequent lymph node and bone marrow biopsies were negative. The patient then underwent a liver biopsy which demonstrated hemophagocytosis. HLH was eventually confirmed with other supporting laboratory tests. Fortunately, this patient survived after initiation of rituximab with dexamethasone.
Discussion: HLH is a rare but life-threatening autoimmune disease characterized by hyperinflammation and uncontrolled immune activation. The diagnosis of HLH in this patient was challenging due to his many non-specific symptoms, his occupation and the acute need for steroid use for his liver failure. This high dose steroid complicated diagnosis until a liver biopsy was performed demonstrating hemophagocytosis. It is important to note that hemophagocytosis can be seen in the spleen, liver or lymph nodes. Therefore a bone marrow biopsy, while helpful, is not crucial to the diagnosis and should not delay high dose steroid treatment for acutely ill patients. Additionally, a negative lymph node biopsy does not exclude diagnosis and clinical suspicion should prompt further investigation. Hemophagocytosis is neither pathognomonic, nor required for the diagnosis of HLH. In our case, other diagnostic criteria such as NK cell activity or CXCL9 were unavailable at our institution and so the presence of hemophagocytosis on liver biopsy was crucial in guiding diagnosis. Finally, HLH secondary to EBV specifically should be treated with rituximab. This is because EBV induces B lymphocyte proliferation while rituximab depletes B cells leading to improved outcomes for these patients.
Conclusions: This case highlights the importance of early recognition and clinical suspicion of HLH, particularly in patients with recent viral infections, to ensure prompt treatment and improve outcomes given the high mortality rates associated with the condition. Hemophagocytosis in HLH secondary to EBV, clinicians should use rituximab for treatment rather than etoposide.