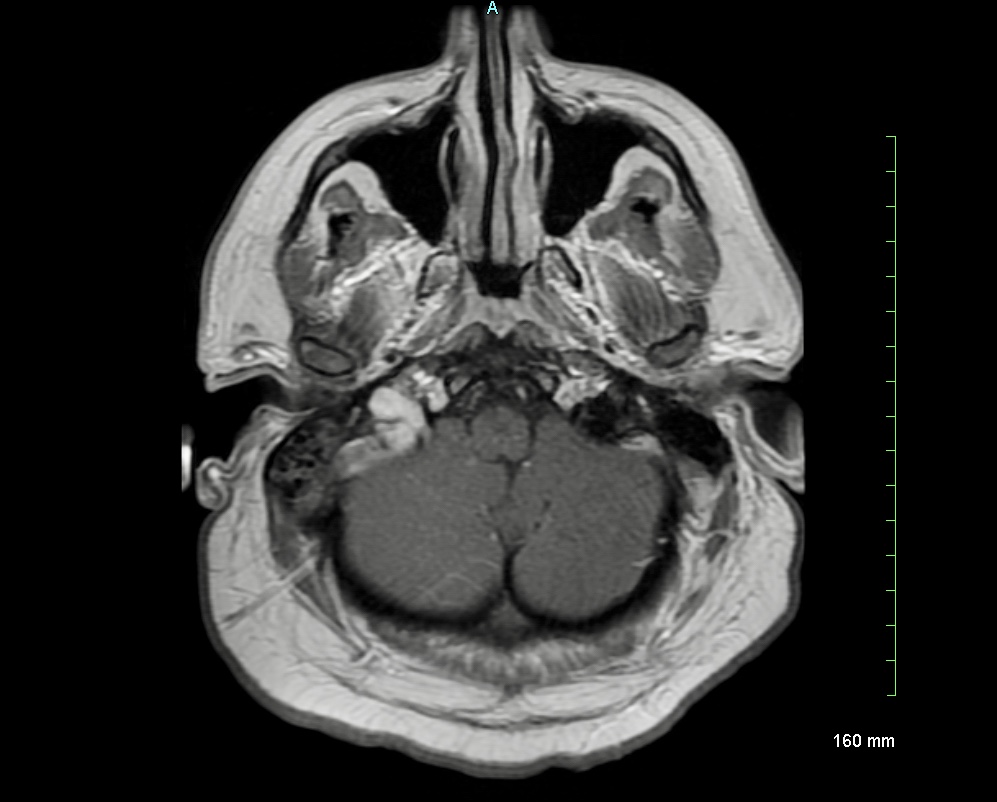
Case Presentation: A 29-year-old male presented with a new onset focal seizure and dull persistent right sided headaches for 2 weeks. Physical exam was negative for any focal neurological deficit except for a diffuse erythematous rash involving trunk and his extremities, bilateral conjunctival injection and mild confusion. An urgent CT head revealed a small acute parenchymal hemorrhage in the right inferior parietal lobe with a small amount of associated SAH. A subsequent CTA ruled out vascular malformations, but revealed dural venous sinus thrombosis involving right transverse sinus, sigmoid sinus, jugular bulb, and a portion of right IJV. MRI confirmed the findings. Lab results were pertinent for WBC count 3.5, CRP 1 and mild proteinuria with WBC casts. Extensive thrombophilia work-up was negative, yet autoimmune blood work revealed positive ANA (>1:640), dsDNA:72, low C3 and C4 levels, negative APLA and negative RF. EEG did not show any new epileptiform activity. Patient met the diagnostic criteria of SLE as per ACR. He was started on oral prednisone, hydroxychloroquine and therapeutic heparin, and gradually transitioned to warfarin with INR goal of 2-3.
Discussion: Cerebral venous sinus thrombosis (CVST) is an uncommon manifestation of neuropsychiatric lupus and is usually associated with secondary antiphospholipid antibody syndrome (APLA). CVST as a presenting feature in a male patient with systemic lupus erythematosus (SLE) with negative APLA is particularly rare (1,2). We report the case of a young male with CVST as the initial form of presentation of his SLE. He also has negative antiphospholipid antibodies.
Dural venous sinus thrombosis is a relatively rare complication of SLE, and even more rare to be a presenting diagnosis (3). In most cases, it is associated with anti phospholipid antibody syndrome but rarely presents without secondary APLA (4). CVST usually occurs in active lupus patients and has been associated with a higher SLEDAI score (SLE disease activity score). Etiology of CVST is multifactorial in SLE including vasculitis due to immune complexes along with prothrombotic state due to APLA (5). CVT can present as headaches, intra cranial hypertension, altered mental status, seizures or a local mass.
Conclusions: A high index of suspicion is essential, especially in young patients who present with cerebrovascular accidents without typical risk factors for arterial thrombosis. Prompt diagnosis and treatment can prevent potential residual neurological deficits and unfavorable outcomes.