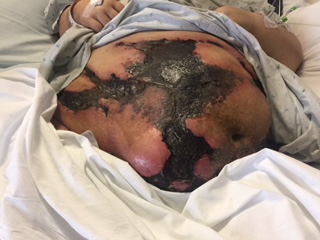
Case Presentation: A 52-year-old Caucasian female with medical history of recurrent deep vein thrombosis on warfarin for over 10 years and type II diabetes mellitus, presented as a transfer from outside hospital for further evaluation of necrotic abdominal wall wounds thought to be secondary to warfarin.She initially presented for evaluation of worsening abdominal wall necrotic rash that started one month prior as purpura over the umbilical region. She was treated with doxycycline for presumed panniculitis without improvement. Her lesions worsened over next few days to become necrotic and extended to her upper thighs. She was switched to dabigatran for fear of warfarin skin necrosis, but the lesions continued to spread despite medication change, and was transferred to our facility.
A skin exam was notable for multiple tender abdominal 20-30 cm interconnected retiform purpuric plaques with firm necrotic centers. The borders appeared less inflamed, with evidence of minimal re-epithelialization at base. On the left lower posterior leg were two 5-6 cm retiform purpuric patches, the superior lesion had central necrotic eschar.
Extensive hypercoagulability workup was notable for positive lupus anticoagulant and heterozygous prothrombin gene mutation. A full thickness abdominal skin biopsy revealed full thickness skin necrosis with intravascular thrombosis (dermal and pannicular) and panniculitis that was negative for calcium deposits.
Due to the clinical picture and biopsy results the underlying cause of ischemic skin necrosis was determined to be caused by thrombotic vasculopathy syndrome secondary to her prothrombin gene mutation and lupus anticoagulant positivity. She was treated with enoxaparin with improvement in wound appearance. Despite this, she developed new retiform purpuric lesions. The most recent biopsy showed thrombosis and necrosis which were more advanced in comparison to prior tissue samples.
Discussion: Here we present an interesting case of thrombotic occlusive vasculopathy, a syndrome characterized by arterial or venous thrombosis caused by a variety of systemic conditions. It is rare to present with such extensive subcutaneous thrombosis and necrosis. This patient’s clinical presentation is very similar to calciphylaxis, making this a challenging case to diagnose. In this case, it was crucial to obtain a biopsy and hypercoagulability workup to establish a diagnosis of thrombotic occlusive vasculopathy.
Conclusions: Both thrombotic occlusive vasculopathy and calciphylaxis are associated with significant morbidity and mortality. It is important to rule out calciphylaxis as the medical management is distinct in the use of sodium thiosulfate, compared to anticoagulation for the treatment of thrombotic occlusive vasculopathy. Clinicians should consider thrombotic occlusive vasculopathy associated with underlying prothrombotic state as part of the differential diagnosis in patients presenting with a similar rash.