Background:
Transitioning care from hospitalization to ambulatory care can be a stressful and confusing experience for patients. The Society of Hospital Medicine has been charged to develop quality measures around the processes of appropriate and timely transition to postdischarge care. As hospitalists, we are poised to guide patients and to determine the most appropriate and timely follow‐up care. To address this potential gap in patient care, our hospitalist group evaluated the process by which patients are provided with their follow‐up appointment postdischarge.
Purpose:
To actively engage patients in scheduling a follow‐up appointment prior to their discharge from the hospital and to optimize their transition to the ambulatory care setting.
Description:
We created an online discharge appointment (ODA) Web page that takes 1 minute to complete. The information is received and reviewed by referral center coordinators along with insurance information. The patients are contacted by the referral center in their hospital room and connected to the follow‐up clinic to schedule an agreeable appointment for the patient within the time requested by the hospitalist. The appointment is entered into our scheduling system and is noted to be complete on the ODA Web page.
Conclusions:
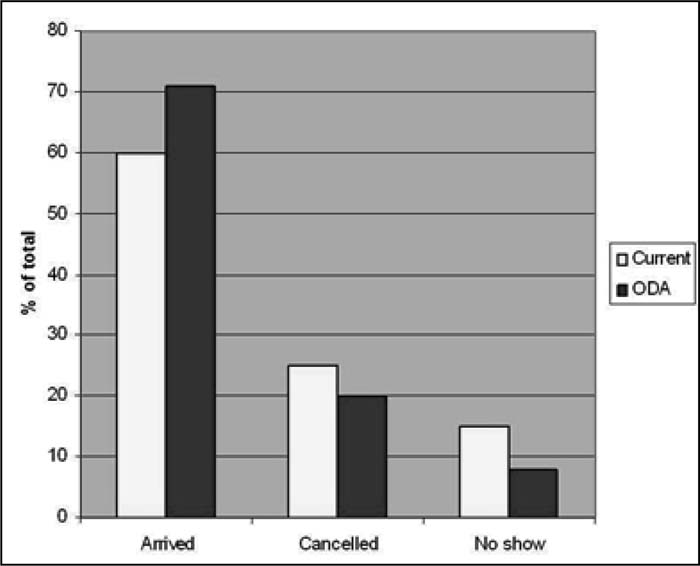
To assess the impact of this project, we looked at roughly 500 appointments scheduled through the ODA Web site by our hospitalist group. We analyzed the arrival, no‐show, and cancellation rates of the discharged patients. There was a 10% increase in arrivals to the clinics, with a 5% reduction in the cancellation rate and a 10% reduction in the no‐show rate (Fig. 1). In addition to the transition of care benefit for the patient, there has been an organizational benefit to better utilize the ambulatory care visit slot. We have developed an improved process for the transition of care from the inpatient to outpatient setting for patients, which has also reduced lost appointments and improved clinic arrival rates postdischarge. Informal surveys have shown an extremely high level of satisfaction from both patients and our hospitalists. Future metrics will include “return to ED within 3 days,” “return to ED within 14 days,” and “readmission within 14 days” for patients who received this transition of care service prior to their discharge.
Author Disclosure:
R. Chang, none; K. Bombach, none; C. Kim, none.