Background: Inpatient physicians often spend 30-60 minutes daily creating a “rounding list,” a process that requires reviewing the electronic health record (EHR) and transcribing data to paper. Previous studies have described automated rounding-lists leveraging EHR data showing improved clinician satisfaction, decreased daily chart review time, and improved accuracy of information. However, previous rounding lists were often developed in the context of a “home-grown” EHR limiting their potential for dissemination. Notably, clinicians prefer daily printed lists for rounding for portability despite electronically available resources.
Purpose: We aimed to implement a secure, clinician-friendly, user-customizable rounding list application embedded within a large, well-known commercial EHR (EpicTM) to automatically generate rounding lists that include patient-specific information directly pulled from the EHR with the goal of improving clinician satisfaction, decreasing daily chart review time and improving accuracy of information.
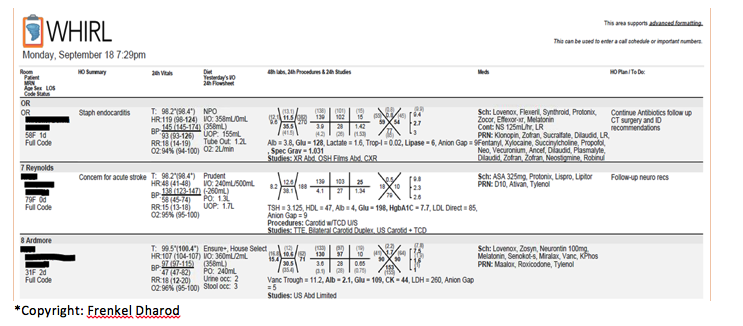
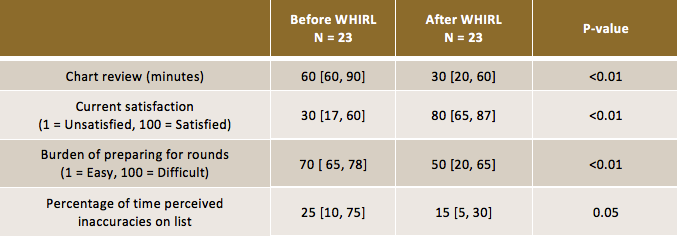
Description: We developed an inpatient rounding list generator termed the WHIRL embedded in the EHR. An example generated list is shown in Figure 1. In the WHIRL, columns with the “HO” prefix indicate free text handoff fields entered by clinicians in the EHR. WHIRL performs data manipulation and formats abnormal labs and vitals using information directly extracted from the EHR. The WHIRL allows clinicians to customize the look and feel of the rounding list. Individual labs and meds can be shown (or hidden) and dosage, form, and frequency can be displayed per medication. WHIRL was tested in beta-phase for several weeks prior to implementation on August 21, 2017. The WHIRL application usage increased from 50 to over 800 users within 1 month. WHIRL usage data from 10/02/2017-11/09/2017 reveals mean values of 108 active users per day, 228 lists generated per day and 631 patients accessed across the Health System per day. Survey data from 23 beta users is shown in Table 1. In brief, WHIRL saved clinicians’ time, improved satisfaction, and resulted in fewer rounding list data errors.
Conclusions: The WHIRL went “viral” at one academic medical center. Preliminary data suggests that using WHIRL decreases chart review time, improves provider satisfaction and improves accuracy of information. Time saved by WHIRL can be repurposed to education, communication between health care providers and direct patient care. We plan to further evaluate the WHIRL by surveying a broader clinical audience 6 months after the implementation of initial intervention, continuing to evaluate usage statistics and evaluate detailed EHR system usage time via click-action logs.