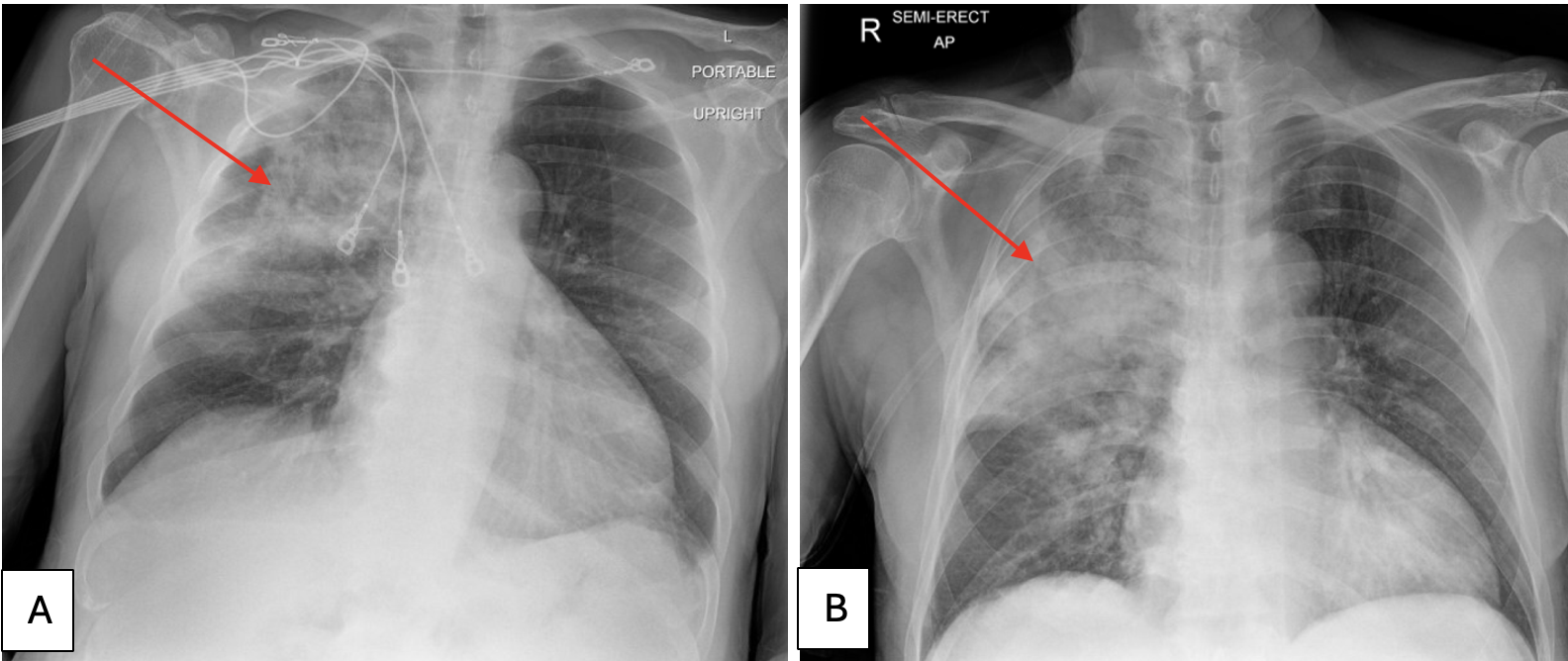
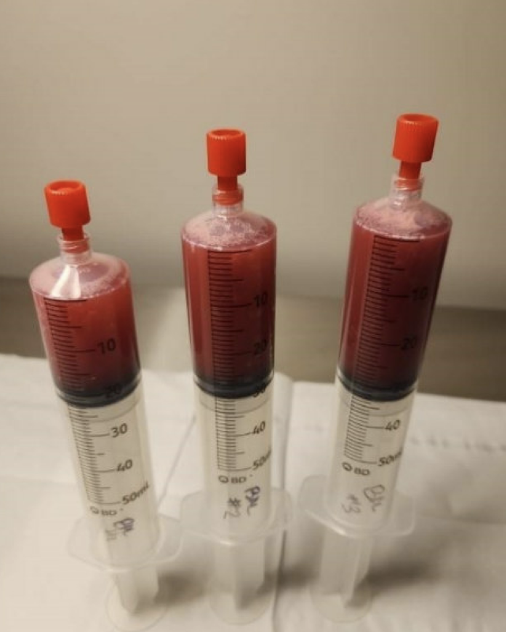
Case Presentation: We present a rare case of hydralazine-induced diffuse alveolar hemorrhage (DAH) in a 74-year-old male with a history of hypertension. The patient was admitted with symptoms including hemoptysis, dyspnea, and dark urine. Initial findings included a biopsy-confirmed leukocytoclastic vasculitis, elevated MPO antibodies, and evidence of DAH on bronchoscopy. Despite the absence of glomerulonephritis, the patient exhibited signs of pulmonary-renal syndrome, including worsening renal function and anemia. Notably, the patient developed melena (likely from aspiration of pulmonary hemorrhage per the gastroenterology team) and a down-trending hemoglobin to 6.8 g/dL (ref: 13.3-17.5 g/dL) which improved with a transfusion of 2 packed red blood cells. A bronchoscopy was also completed the same day which yielded heavy RBCs without organisms and a bronchoalveolar lavage suggestive of DAH. The patient’s condition improved significantly after cessation of hydralazine and initiation of intravenous methylprednisolone. On discharge, he continued 60 milligrams of methylprednisolone for 4 weeks with a taper for 5 additional weeks (decreasing 10 milligrams every week).
Discussion: Hydralazine is a known, well-tolerated, arterial vasodilator often used to treat essential hypertension, heart failure with reduced ejection fraction, and hypertensive emergency. Hydralazine is also known to induce hydralazine-induced ANCA vasculitis (HIAV) which can be challenging to delineate from hydralazine induced lupus given overlapping clinical features and markers such as positive ANA and hypocomplementemia.While the specific mechanism for HIAV is not fully understood, several theories include preferential autoreactivity of renal and pulmonary vasculature by anti-MPO or PR3, biotransformation, or activation of the innate immune system from neutrophil muscarinic receptors. Documented cases have noted that patients with HIAV often presented as older, female patients who have been on routinely prescribed hydralazine dosages for fewer than 5 years. Despite its rarity, HIAV is an important consideration to keep in mind because of its risks of rapidly increased mortality. In fact, studies have indicated the DAH in the setting of ANCA-associated vasculitis including HIAV is the most significant predictor of mortality. The combination of both glomerulonephritis and pulmonary hemorrhage is indicative of pulmonary-renal syndrome which is correlated with a high mortality risk even if addressed medically. Thorough review of medications with known risks of drug-induced vasculitis (DIV) such as hydralazine, allopurinol (which our patient was also taking but continued upon discharge given his improved condition), and minocycline (often with patients treating acne) is pertinent. Other considerations when managing patients with DIV include a comprehensive substance use history or urine drug screen to assess for cocaine use, as levamisole is often used to adulterate cocaine and has been linked to DIV.
Conclusions: This case underscores the importance of considering hydralazine-induced ANCA vasculitis in patients presenting with unexplained pulmonary hemorrhage, particularly when other common causes are ruled out. Early recognition and management are crucial to prevent potentially life-threatening complications associated with this rare condition.