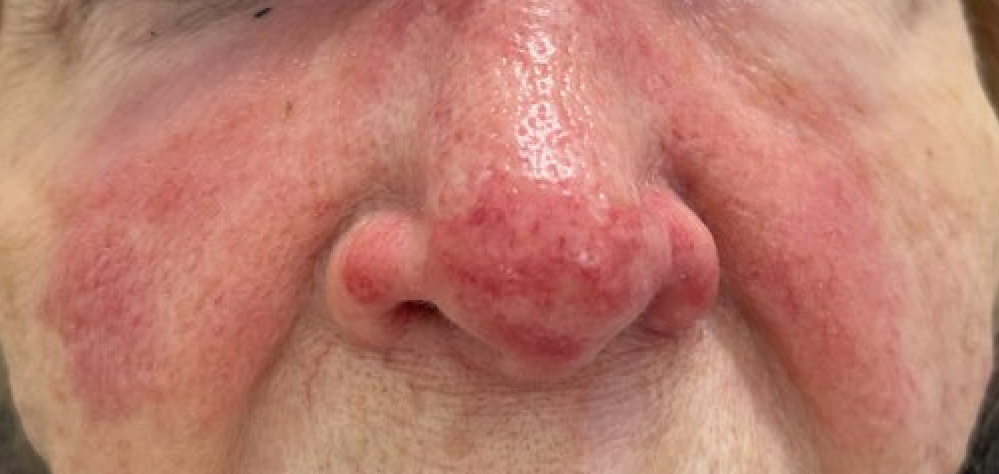
Case Presentation: An 86-year-old female with well-compensated cirrhosis due to primary biliary cholangitis (PBC) visited her PMD complaining of a fever of 102.2, nasal congestion, and sore throat that had started 2 days prior and was followed by a rapidly spreading malar rash that developed on the day she presented. The rash started with tiny pustules and erythema over her nasal bridge and then spread to cheeks and nasolabial folds. The patient was referred to the ED, where physical examination revealed normal vital signs, pharyngeal erythema without tonsillar exudates, and painful bilateral cervical lymphadenopathy. Oral examination did not show caries or periodontal disease. The skin exam revealed raised well-demarcated erythematous facial plaques in a butterfly pattern. The involved area was swollen, warm, and exquisitely tender to palpation. Labs were unremarkable except for chronic thrombocytopenia. Due to the rapid spread of the facial rash, the patient was admitted for treatment with IV antibiotics and started on ceftriaxone and vancomycin. Tests for influenza, COVID, and respiratory PCR panel were negative. A rapid strep test was positive for Group A streptococcus (GAS or Streptococcus Pyogenes). Antibiotics were de-escalated to ceftriaxone. The patient’s rash faded over the next 2 days, and pharyngeal discomfort also subsided. The patient was eventually discharged home on oral antibiotics.
Discussion: Our patient is an immunocompromised elderly woman who presented with both acute pharyngitis and a rapidly spreading facial rash. The simultaneous presentation of skin and soft tissue infection and upper respiratory infection was felt to be linked by the common causative agent, GAS. GAS is by far the most common cause of erysipelas with Staphylococcus aureus occurring much less frequently. The infection rapidly spreads through the superficial lymphatic vessels of the skin giving the appearance of raised erythematous plaque with sharply demarcated margins. Half a century ago erysipelas classically involved the face but in current times the predominant location is the lower extremities. There are multiple portals of entry for streptococci including surgical incisions, insect bites, venous stasis ulcers, and small facial abrasions. In rare instances, facial erysipelas may be caused by a recent infection in the nasopharyngeal passage as in our case. GAS is an important cause of invasive disease and death affecting persons over the age of 65 at a very high incidence and at a particularly high incidence in residents of long-term care facilities. Complications of facial erysipelas include spread to deeper fascial spaces and necrotizing fasciitis. Immunosuppressive state and diabetes are among the predisposing factors for necrotizing fasciitis. Recurrent erysipelas at the same site is also something that has been reported.
Conclusions: GAS infections include many body sites and varying degrees of severity ranging from asymptomatic pharyngeal colonization to potentially lethal toxic shock and necrotizing fasciitis. Among the most common sites of GAS infection are the skin and the pharynx. Our patient presented with simultaneous microbiologically confirmed GAS pharyngitis and facial erysipelas almost certainly caused by the same agent. Distinctive to this case was the indirect confirmation of the suspected causative agent of a skin infection via sampling of a throat specimen.