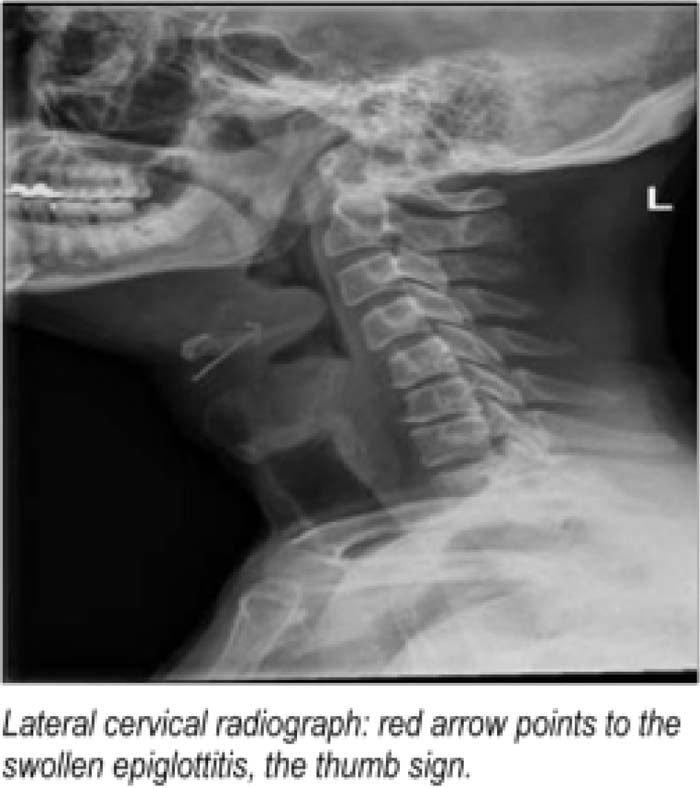
Case Presentation:
Acule epiglottitis is potentially fatal as it can cause sudden airway obstruction. With an infrequent occurrence in adults, it is underrecognized and misdiagnosed often. We report an adult patient with acute epiglottitis who was initially Treated as a simple sore throat. A 48‐year‐old male patient presented to the emergency department with a 2‐day history of sore throat and odynophagia. Initially seen in an outside clinic 36 hours earlier, he was prescribed Augmentin. However, his symptoms worsened over 24 hours, and he had difficulty in swallowing saliva. Vital signs were normal. Physical examination revealed hyoid area tenderness, edematous uvula and Tonsils with no exudates. He had leukocytosis (21.500 cells/mm3) with neutrophilia. Rapid strep screen, heterophile test, and chest x‐ray were normal. A lateral neck x‐ray revealed a swollen epiglottis — a thumb sign. CT scan of neck confirmed acute epiglottitis with near‐complete airway obstruction. Patient was closely monitored in the intensive care unit. Subsequent flexible laryngoscopy demonstrated inflammation of the epiglottis and supraglottic structures. With Unasyn and Decadron. he improved symptomatically in 2 days without the need for an artificial airway.
Discussion:
Acute epiglottitis in adults is often referred to as supraglottitis, as it is an inflammation of the epiglottis, aryepiglottic folds, base of the Tongue, uvula, and pharynx. Studies show a steady increase in its incidence. Mortality rate is 7% in contrast to >1% in children. Usually presenting with only a severe sore throat out of proportion to oropharyngeal examination, a diagnosis can be missed easily, as in our case. A third of adults present with respiratory compromise. Hence, security of the airway is paramount. The presence of stridor, drooling, cyanosis, or respiratory distress mandates an artificial airway. Paradoxically, bag and mask ventilation can worsen obstruction. Although 71%—90% of adults can be managed without an artificial airway, the potential threat to airway warrants ICU care and consultation by an otolaryngologist/anesthesiologrst. In the absence of respiratory distress, a cervical radiograph can be obtained that shows the characteristic thumb sign (as indicated by the red arrow in the picture). Flexible laryngoscopy in a controlled setting is the preferred method of diagnosis. The treatment includes a combination of third‐generation cephalosporins with clindamycin. Steroid use is controversial, as retrospective studies have not shown reduction in hospital or ICU stay or duration of intubation.
Conclusions:
Our case serves as reminder of this uncommon condition that can be potentially dismissed as just another sore throat. The threat of airway compromise and mortality of 7% necessitates cognizance of this condition among hospitalist physicians.
Author Disclosure:
L. Reddy, none; R. Yarlagadda, none; D. Lingutla, none; A. Rohatgi, none; R. Pulli, none; J. Giangreco, none; A. Khan, none.