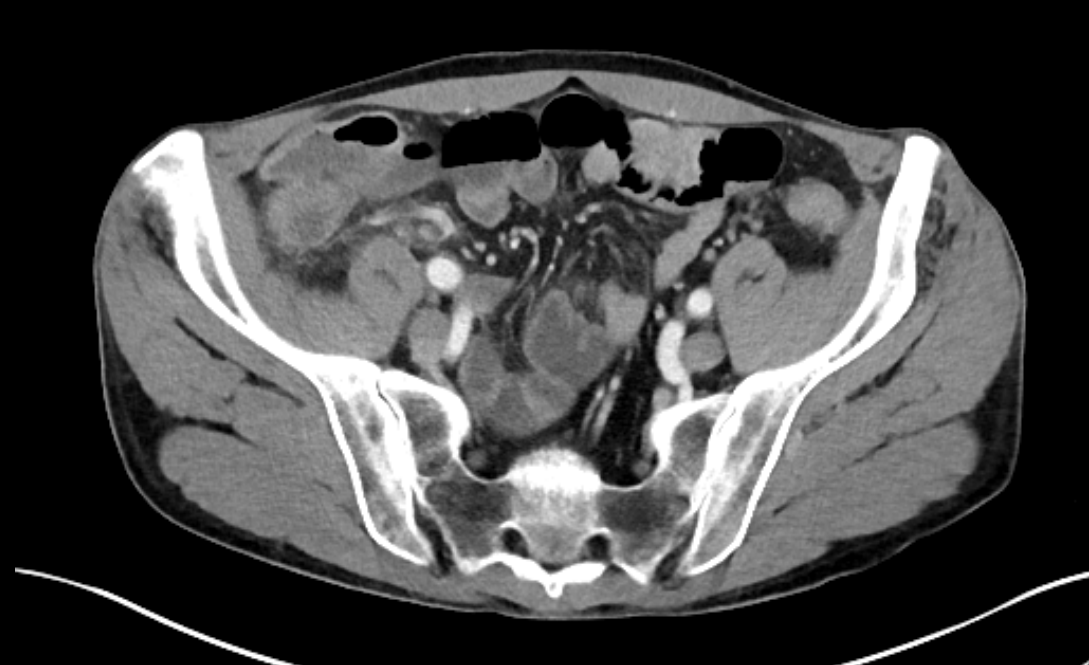
Case Presentation: A 41-year-old male with past medical history of ulcerative colitis (UC) currently on vedolizumab infusions every 8 weeks presented to the hospital with right lower quadrant abdominal pain. The patient endorsed nausea, vomiting, and 15-20 loose, bloody bowel movements per day. Upon admission, the patient was afebrile, normotensive, and non-tachycardic. Physical exam revealed significant tenderness to the right lower quadrant, no abdominal distention, or mass. Pertinent labs included hemoglobin 8.7 g/dL (13.2-16.6) and WBC 6.9 x 10(9) (3.4-9.6). CT abdomen/pelvis revealed periappendiceal inflammatory changes with disruption in the wall of the appendix consistent with acute appendicitis with possible perforation. There was no abscess or fluid collection visualized. He was admitted to the hospitalist team, and IV ciprofloxacin and metronidazole were initiated. Gastroenterology was consulted for refractory UC and started the patient on IV Solumedrol 30 mg b.i.d. General surgery was consulted and recommended appendectomy but informed the patient that colectomy may be required if the colonic tissue was poor. The patient subsequently refused appendectomy. Interventional radiology was consulted, and the patient underwent percutaneous drainage of an abscess which was seen on repeat CT scan two days later. He was stabilized, his bowel movements decreased with IV steroids, and he was discharged to complete his course of antibiotics. Outpatient follow up was scheduled, and his vedolizumab infusion was held due to active infection.
Discussion: Appendectomy and UC is a well-studied topic, but the data has been conflicting. Past studies have shown that an appendectomy may be a protective factor against development of UC or, if undergone prior to diagnosis of UC, may predict a less severe disease course and lower the odds of colectomy. Appendectomy has also been studied as a treatment modality in refractory UC. However, a recent study showed that appendectomy may be associated with increased odds of future colectomy, while yet another meta-analysis suggested there may be no correlation between the two. Even though the definitive treatment for acute appendicitis is an appendectomy, there is inconclusive data on whether this could increase the risk of colectomy in patients with UC who present with appendicitis.
Conclusions: Appendectomy may increase the risk of colectomy in patients with ulcerative colitis, but the data has been conflicting. Patients with UC who develop acute appendicitis may require an appendectomy, but medical management with antibiotics and percutaneous drainage is a viable treatment option, as was in this case. Future studies may be beneficial on whether appendectomy could predict disease severity or odds of colectomy. Hospitalists need to be informed on this topic as it could impact the care provided to this specific patient population who would potentially benefit from medical management of appendicitis rather than a surgical approach.