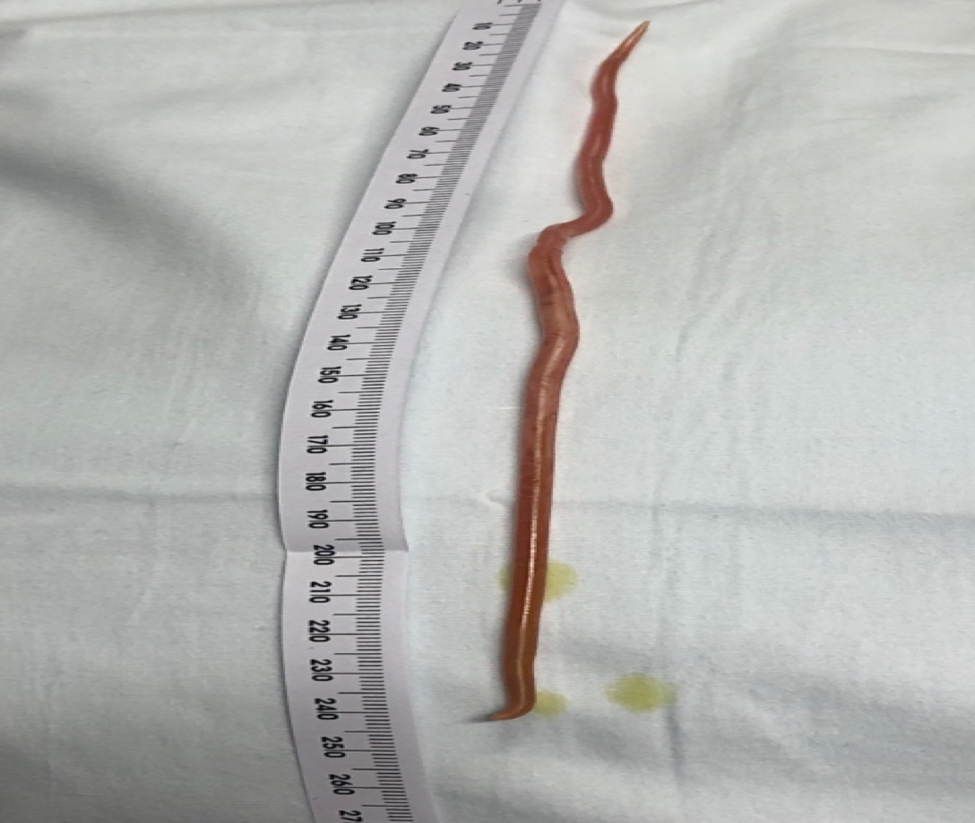
Case Presentation: A five year old male presents to the emergency department with abdominal pain and emesis. Labs were significant for hyponatremia, elevated alkaline phosphatase, mild hyperproteinemia, and leukocytosis with neutrophilia. Urinalysis showed ketones present. A plain film of the kidneys, ureter, and bladder showed distension of the transverse colon and stool in the rectum. Social history taken was limited to patient living with his siblings and parents. He received 2 normal saline boluses and was admitted to the pediatric floor for suspected viral gastroenteritis. On hospital day 1, the patient developed bilious emesis. An upper gastrointestinal/small bowel follow through study showed mildly delayed passage of contrast through the duodenum. The patient had another episode of bilious emesis containing a 22 centimeter live worm. It was determined the bilious emesis was due to a parasite burden. Patient underwent conservative management which included the placement of a nasogastric tube with suction, administration of intravenous fluids, and electrolyte correction before administering anthelmintic therapy. To further induce worm relaxation, mineral oil was administered through his nasogastric tube. Investigation by the infectious disease team revealed that the patient’s social history included living on a farm with daily exposures to various animals. The infectious disease team felt that the elevated alkaline phosphatase and the hyperproteinemia were a reflection of an acute helminthic infection. Patient received one dose of mebendazole in the hospital. The patient clinically improved. He did have stool passage of worms prior to discharge. Laboratory analysis identified the emitted worm as Ascaris lumbricoides.
Discussion: Ascaris is the leading helminthic infection worldwide. It disproportionally affects children in tropical and low and middle income countries. In developed countries, infection is rare in children. Individuals infected are often asymptomatic until a worm burden threshold is reached. Infection can lead to intestinal blockages and impaired growth. Eosinophilia is often the first indication of a parasitic infection. In an infection with Ascaris, eosinophilia only occurs through the larval migration through the lungs. Adult worms residing in the lumen of the gut do not produce eosinophilia.
Conclusions: While dehydration secondary to gastroenteritis is one of the most common inpatient pediatric diagnoses, a high index of suspicion should have been present for a parasitic infection in this patient due to exposure history. Obtaining a thorough social history is essential in creating a meaningful differential diagnosis. Eosinophilia does not necessarily need to be present as one may expect for ongoing parasitic disease. Correct identification and treatment with confirmation of cure is needed to prevent long term adverse effects in children affected by parasitic disease.