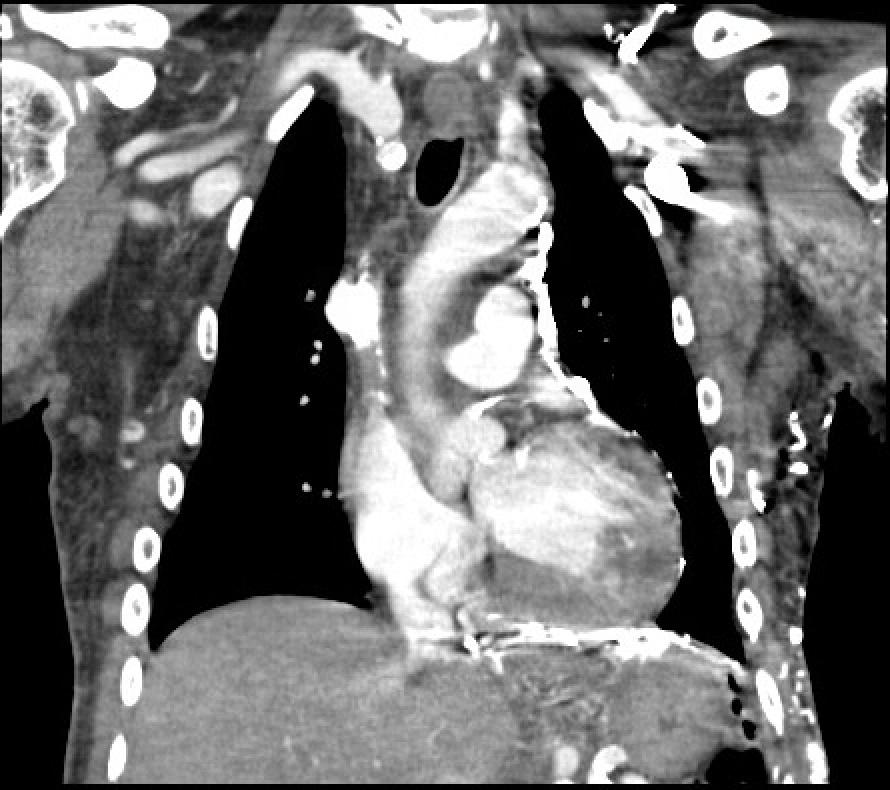
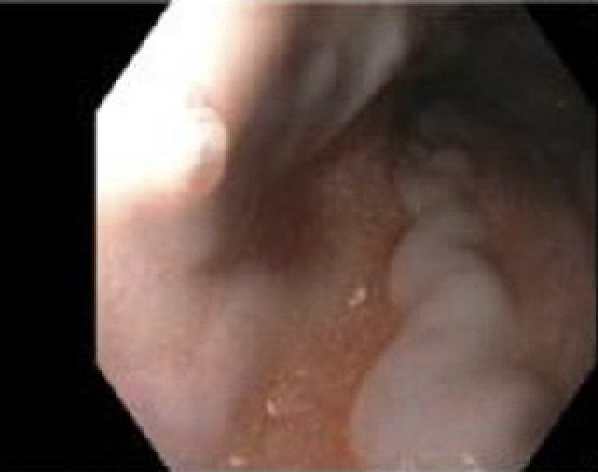
Case Presentation: A 59 year old male with history of End Stage Renal Disease (ESRD) on Hemodialysis, Cerebrovascular disease and Hypertension presents to emergency department (ED) with single episode of bloody emesis and hemoptysis without associated abdominal pain or melena. On exam he was afebrile, hypertensive without tachycardia. His mucous membranes were dry, sclera non-icteric, with no abdominal tenderness or stigmata of chronic liver disease. Laboratory evaluation was significant for anemia (hemoglobin 9.8 gm/dL), elevated BUN (50 mg/dL), elevated creatinine (8.74 mg/dL), with normal lactic acid (1.8 mmol/L). CT scan of chest was done in ED which was negative for pulmonary embolism but showed findings of esophagitis and chronic superior vena cava (SVC) occlusion with multiple chest wall collaterals with enlargement of azygous and hemiazygous veins. (Figure 1) After fluid resuscitation, EGD was performed which showed varices in middle third of esophagus (Figure 2) with stigmata of recent bleeding. Six bands were deployed for hemostasis. Ultrasound of abdomen with dopplers showed normal liver parenchyma and normal flow in hepatic vein and portal vein. Given his history of chronic hemodialysis with central line placement, diagnosis of Downhill Variceal Bleeding from SVC obstruction was made. Patient remained stable and underwent IR guided SVC stenting. Patient had repeat EGD in a month which showed trace prominent vein in upper and middle third of esophagus, with no obvious varices.
Discussion: Esophageal Varices from Liver Cirrhosis or portal hypertension is usually present in lower third of esophagus. “Downhill” or Upper esophageal varices involves upper or middle third of esophagus and their presence does not denote portal hypertension or cirrhosis. Finding of downhill varix should prompt evaluation of venous obstruction that drain the upper part of esophagus. Venous drainage of esophagus is intriguing. The upper esophageal plexus drains into the inferior thyroid veins. The middle esophageal plexus drains into the azygos, hemiazygos, bronchial, and intercostal veins. All the previous veins drain into the SVC. An obstruction in any of the aforementioned veins can cause upper esophageal varices. Downhill varices account for very rare cause of gastrointestinal bleeding. Downhill varices are less likely to bleed than portal hypertension-related varices, but when bleeding occurs, it can be severe and life-threatening [1, 2]. Endoscopic therapies are first step in temporizing active variceal bleeding, but relief of the underlying SVC obstruction is the cornerstone of treatment and should be pursued as soon as possible. Common causes of downhill varices include SVC obstruction from thrombosis related central venous catheter or pacemaker leads and mediastinal malignancy especially lung or lymphoma. ESRD patients with central venous catheters are at particular risk [2,3,4,5].
Conclusions: Downhill varices or Upper esophageal varices are extremely rare cause of gastrointestinal bleeding, estimated to account for only 0.1% of cases of variceal bleeding [1]. Their presence requires looking for venous obstruction, especially SVC obstruction as the cause of downhill varices. Downhill varices are distinct entity from lower esophageal varices requiring its own pathway of work up and management. Definitive treatment of downhill varices involves venous stenting or angioplasty.