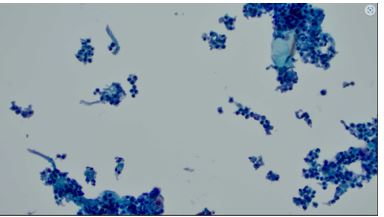
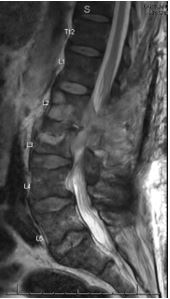
Case Presentation: A 69-year-old male with a significant past medical history of rheumatoid arthritis on methotrexate presented with acute-on-chronic lumbar pain. Initial imaging revealed an L3 compression fracture, with findings suggestive of discitis or osteomyelitis at L2-L3. MRI confirmed discitis/osteomyelitis, along with an epidural abscess and bilateral psoas abscesses. Further imaging also revealed cavitary pulmonary lesions. The patient tested positive for PPD during routine screening for initiation of infliximab therapy (Remicade). Subsequent diagnostic studies, including QuantiFERON-TB Gold and blood cultures, were unremarkable. Empiric antibiotic therapy with ceftriaxone and vancomycin was initiated, later replaced by daptomycin due to clinical suspicion of bacterial osteomyelitis. A comprehensive workup, including CT imaging and bronchoscopy with bronchoalveolar lavage (BAL), was pursued. Cultures ultimately identified MAC from both the lumbar abscess and BAL samples. Antibiotic therapy was adjusted to a regimen of clarithromycin, ethambutol, rifabutin, and amikacin. Despite surgical drainage and ongoing antimicrobial therapy, the patient’s treatment course is projected to extend over 12 to 18 months, with close monitoring for clinical and radiologic response.
Discussion: This case highlights MAC osteomyelitis, an exceedingly rare manifestation of MAC infection, typically associated with pulmonary or disseminated disease in immunocompromised individuals. MAC osteomyelitis accounts for less than 1% of osteomyelitis cases, with fewer than 20 reported cases worldwide. Diagnosing such a rare condition requires a high index of suspicion, particularly in patients with risk factors such as immunosuppressive therapy. The patient’s presentation with lower back pain, compression fractures, and abscesses initially suggested common causes such as bacterial osteomyelitis. However, the discovery of positive PPD testing, coupled with culture results confirming MAC, guided the diagnostic workup toward this atypical pathogen. Early consideration of MAC and other rare pathogens was critical, as a delay in diagnosis could have significantly impacted the patient’s outcome.
Conclusions: This case underscores the importance of a broad differential diagnosis in immunocompromised patients presenting with osteomyelitis. While Staphylococcus aureus and gram-negative organisms are common culprits, rare pathogens like MAC should be considered when clinical features deviate from typical presentations or initial treatments fail. A thorough and methodical diagnostic approach, informed by patient history and risk factors, enabled the timely diagnosis and management of this once-in-a-lifetime case of MAC osteomyelitis.