Background: Correct inhaler technique for COPD medications is essential to achieving optimum delivery into the lungs. Evidence suggests that poor technique is widespread and linked to poor efficacy and adherence. However, the direct relationship between inhaler technique and health status has not been investigated.
Methods: Data from a 2013 US survey dataset of COPD patients collected from primary care physicians and pulmonologists were analyzed. Physicians completed patient record forms on 5 consecutive COPD patients seeking routine care consultation. The same set of patients were invited to complete a questionnaire about their COPD. Assessments included physician reports on patient characteristics (eg, demographics, disease severity, comorbidities), physician and patient reports on patient confidence of correct inhaler usage via a 5-point Likert scale (“not at all” to “completely confident”), patient satisfaction, health status measures including EuroQOL-5 Dimension (EQ-5D) utility and visual analogue scale (VAS) scores, and COPD Assessment Test (CAT). Multiple linear regressions were used to demonstrate relationships between confidence with correct inhaler usage and health status, and logistic regressions were used to assess the relationship between confidence with correct inhaler usage, quality of life, and patient-reported satisfaction. Covariates were age, COPD severity, inhaler education provider, number of comorbidities, education level, adherence, and concomitant nebulizer use (yes/no).
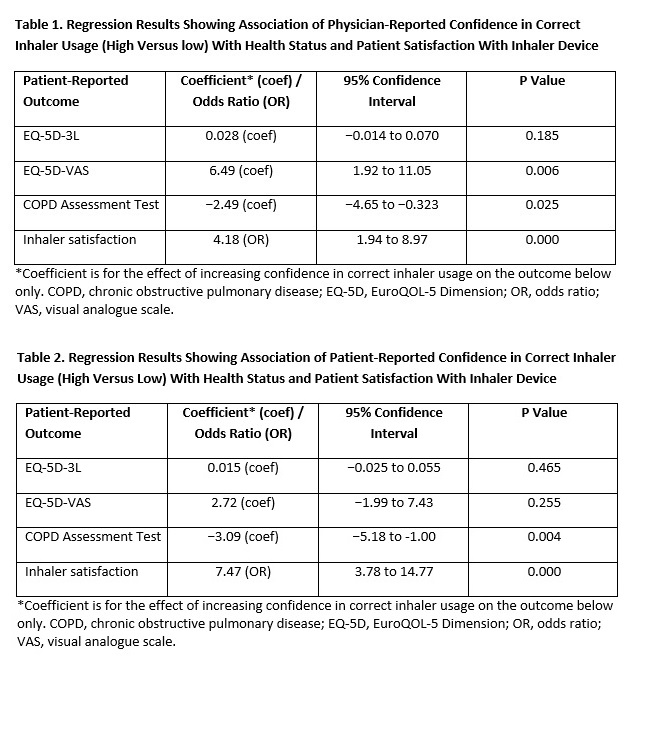
Results: 294 patient record forms (median age 67.5 years, 45% female) from 119 physicians were analyzed. Low confidence in device technique was reported by 37% of patients on dry powder inhaler and 33% on metered dose inhaler. Physicians reported that 43% and 44% of patients had low confidence in the use of these devices, respectively. Both physician- and patient-reported high confidence in inhaler usage were significantly associated with higher patient treatment satisfaction (odds ratio [OR] 4.18, P<0.001; OR 7.47, P<0.001, respectively; Tables 1 and 2). High physician-reported confidence in inhaler usage was also significantly associated with a lower CAT score (coef −2.49, P=0.025), and higher EQ-5D VAS (coef 6.49; P=0.006). The results were mostly consistent when considering patient-reported confidence with inhaler usage.
Conclusions: In this study, poor inhaler confidence levels were reported by physicians and patients in at least 1 in 3 COPD patients regardless of device type. Poor inhaler confidence was associated with lower COPD-related health status. The study findings have implications for assessment of inhaler technique in COPD patients in the community or when discharged from a hospital. Approaches to optimizing patient inhaler technique should be considered for improving health outcomes. Nebulized delivery provides an alternative where poor inhaler technique is related to low peak inspiratory flow rate or difficulties with handling inhaler devices.