Background: Venous thromboembolism, in particular, pulmonary embolism (PE), is a significant contributor to morbidity and mortality associated with COVID-19. In comparison to influenza, COVID-19 leads to a more pronounced hypercoagulable state secondary to endotheliopathy and hyperinflammatory state which results in the formation of venous and arterial thrombosis. Based on prior literature, patients with COVID-19 have a 7-fold higher risk of PE than patients without COVID-19. There is no large-scale study comparing outcomes in COVID-19 patients with and without PE.
Methods: In this study, we utilized National Inpatient Sample (NIS) database 2020 to evaluate and compare clinical outcomes in patients with COVID-19 patients with and without PE. Our sample includes 1,659,040 patients hospitalized with COVID-19 pneumonia between January 2020 till December 2020. We performed propensity-matched analysis for patient characteristics and in-hospital out-comes, including the patient’s age, race, sex, insurance status, median income, length of stay, mortality, hospitalization cost, comorbidities, mechanical ventilation, and vasopressor support.
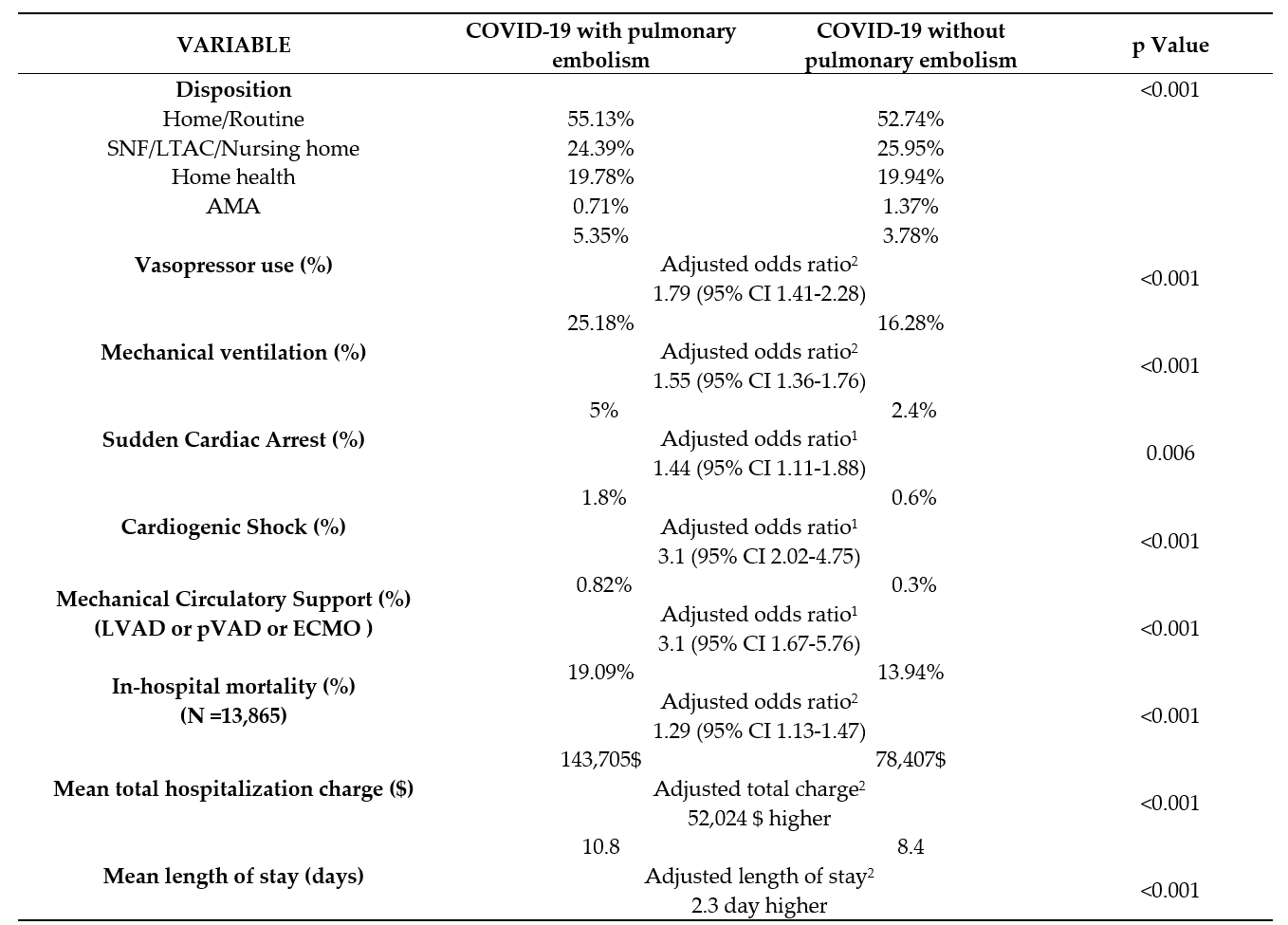
Results: After propensity matching, COVID-19 patients with PE had a higher in-hospital mortality (19.1 vs. 13.9%, adjusted OR of 1.3, 95% CI: 1.1-1.5, p < 0.001), increased need for mechanical ventilation (25.7% vs. 15.6%, adjusted odds ratio 1.4, 95% CI 1.4-1.5, p < 0.001), greater vasopressor dependence (5.4% vs. 2.6%, adjusted OR 1.6, 95% CI 1.4-1.8, p < 0.001), higher incidence of cardiogenic shock (1.8% vs. 0.6%, adjusted OR 3.1, 95% CI: 2.02-4.75, p< 0.001]), greater dependence on mechanical circulatory support (0.82% vs. 0.3%, adjusted OR 3.1, 95% CI: 1.67-5.76, p< 0.001), and sudden cardiac death (5% vs. 2.4%, adjusted OR 1.44, 95% CI 1.11-1.88), and longer hospital stays (10.8 vs. 7.9 days, p< 0.001). Male gender and old age predicted a higher incidence of mortality in COVID-19 patients with PE.
Conclusions: This study highlights the need for more aggressive management of PE in COVID-19-patients with the aim to improve early diagnosis and treatment in order to reduce morbidity, mortality, and healthcare costs.