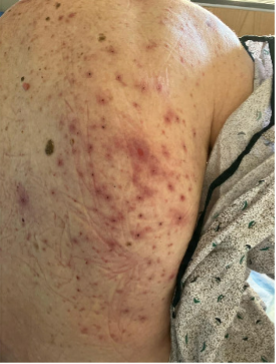
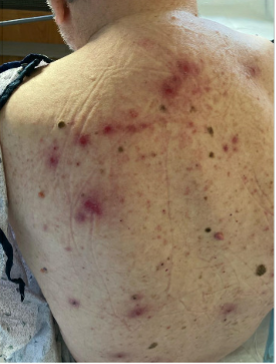
Case Presentation: Patient is a 96 year-old male with significant medical history of hypertension, hyperlipidemia, hypothyroidism, prior left thalamic and internal capsule stroke, shingles, and bilateral blindness who resides in a skilled facility presenting with unsteady gait and garbled speech. Patient presented to an outside hospital on 10/3/2024 for aphasia, dysphagia and right-sided weakness, in which he was diagnosed with left-sided thalamic and internal capsule infarction. He was discharged to a rehabilitation facility five days after, after being managed with aspirin and statin. On 11/3, one of the staff in a skilled facility noticed garbled speech and foot drag, leading the patient to be transported to our ED for a possible brain attack. CT/CTA was negative for acute abnormalities. Brain MRI on 11/4 showed no new lesions. The only significant finding upon admission was elevated LFTs, with AST of 326 and ALT of 303 (baseline: AST 26, ALT 20, alkaline phosphatase 54). A transaminitis work-up was started, which includes abdominal ultrasound, acetaminophen level, HepB/C serologies, monospot test, and iron panel. Due to the patient’s chronic history of shingles and ongoing management with valacyclovir, HSV and VZV IgM testing was also ordered, which returned positive. On examination, the patient had painful ulcer-like lesions across the entire back, consistent with a similar papulopustular rash noted in October per outside records (Figure 1 and 2). A positive PCR result for HSV type 2 confirmed disseminated HSV infection, likely causing HSV hepatitis and encephalopathy. The patient was started on IV acyclovir 350mg q12h and later transitioned to PO valacyclovir 1g q12h for two weeks prior to discharge.
Discussion: Herpes simplex virus (HSV) is one of the common sexually transmitted diseases in the United States. Primary HSV-2 infection is a sexually transmitted disease that presents with painful genital or mucocutaneous lesions (1). Disseminated HSV-2 is a very rare yet serious infection that can initially manifest as transaminitis with no significant findings on imaging as in this patient (2). HSV viremia is more commonly seen in patients with immunodeficiency (4). Our patient presented with non-pruritic, non-vesicular disseminated skin lesions, which is an unusual feature for HSV presentation highlighting a unique presentation and diagnostic challenges involved. Findings of sparse skin lesions makes disseminated HSV infections difficult to distinguish from other common causes of transaminitis such as viral hepatitis, drug-induced liver injury, or auto-immune hepatitis. The involvement of the liver has been reported to occur in approximately 30% of disseminated HSV cases, with transaminitis being the initial remarkable finding. (3) However, few cases describe the simultaneous presence of extensive cutaneous lesions and transaminitis, as seen in our patient. HSV-induced hepatitis has been reported to have a mortality exceeding 75% if left untreated in patients where the majority are immunocompromised, highlighting the significance of early detection and treatment. (5)
Conclusions: Our case highlights the rare incident of disseminated HSV-2 leading to hepatitis and encephalopathy. Although rare and nonspecific, systemic HSV infection should be considered in patients with altered mental status, elevated liver enzymes, and focal neurological deficits. Early detection and treatment of disseminated HSV is essential for improved morbidity and mortality rates for patients.