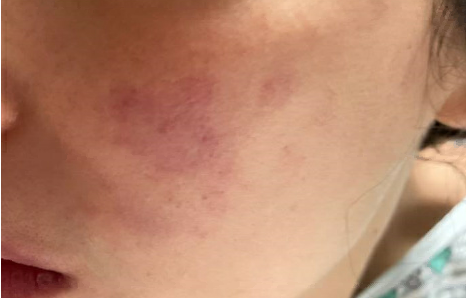
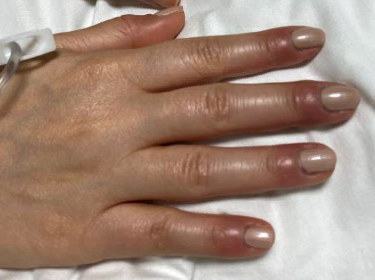
Case Presentation: A 30-year-old female with limited past medical history presented to the emergency department (ED) with 5 days of recurring fevers, nausea, and new rash. The rash was noticeable along her face and arms with pronounced swelling, tenderness, and erythema in her fingers. Initial work-up was significant for hyperferritinemia over 15,000, aspartate aminotransferase of 6,700 and alanine transaminase of 4,270, bicytopenia with white blood count of 4.29 and platelets of 131. Infectious disease was consulted for further evaluation, and she was started on acetylcysteine. A concomitant rheumatologic work-up was initiated and significant for SSA, SSB, and Anti-U1-RNP indicating possible Sjogren syndrome and Mixed connective tissue disease (MCTD). Given elevated ferritin, bicytopenia, and fevers: Macrophage Activation Syndrome (MAS) was on the differential. Rheumatology and hematology were consulted, and she was started on dexamethasone 10mg daily within 28 hours of admission. On day 3 of admission, a bone marrow biopsy (BMB) demonstrated hemophagocytosis. Her symptoms and labs quickly improved following steroid initiation. She was discharged home on dexamethasone 10mg daily, prophylactic sulfamethoxazole-trimethoprim with close rheumatology and hematology follow-up.
Discussion: The differential for such a presentation is broad, and early detection of MAS is dependent on high clinical suspicion. Unfortunately, higher specificity markers for MAS including Natural Killer (NK) levels and Interleukin-2 (IL-2) receptors are not readily available. This leads to increased dependence on rapid, though nonspecific, serum labs such as ferritin, or invasive BMB. Hyperferritinemia presents in a limited number of diagnoses with similar presentation. Once recognized, evaluation for the underlying cause of MAS is pivotal to management and remission. In our patient’s case, her infectious work-up was negative and she improved without antibiotics. Computed Tomography of head, chest, abdomen, and pelvis did not demonstrate any mass or lymphadenopathy that would be concerning for an oncologic process. The inciting factor was likely the newly diagnosed Sjogren’s with MCTD. At the time of presumptive diagnosis and treatment, our patient had 3 of 8 criteria using HLH-2004 out of the needed five. BMB performed after starting dexamethasone demonstrated hemophagocytosis. After discharge, her NK levels were low at 74 cells/mcL and soluble IL-2 receptors were elevated to 2689. These additional studies meet the majority criteria needed to establish a diagnosis.
Conclusions: The mortality of adult patients with MAS has been estimated to be nearly 50%. Thus, early identification and treatment can potentially be lifesaving. Currently, there are two commonly accepted diagnostic tools for MAS: HLH-2004 and 2016 EULAR/ACR/PINTO criteria. There are several problems that present with the use of these criteria: these were developed specifically with pediatric populations in mind and portions of the lab analysis will not be readily available during the acute presentation. More rapid tools exist to evaluate likelihood of HLH/MAS including HScore, though this has poor specificity in adult populations. Ultimately, further research is needed to validate criteria in adult populations for rapid assessment of MAS. Further, if MAS is suspected, it requires a multidisciplinary approach with rheumatology, hematology, and infectious disease for acute and ongoing management.