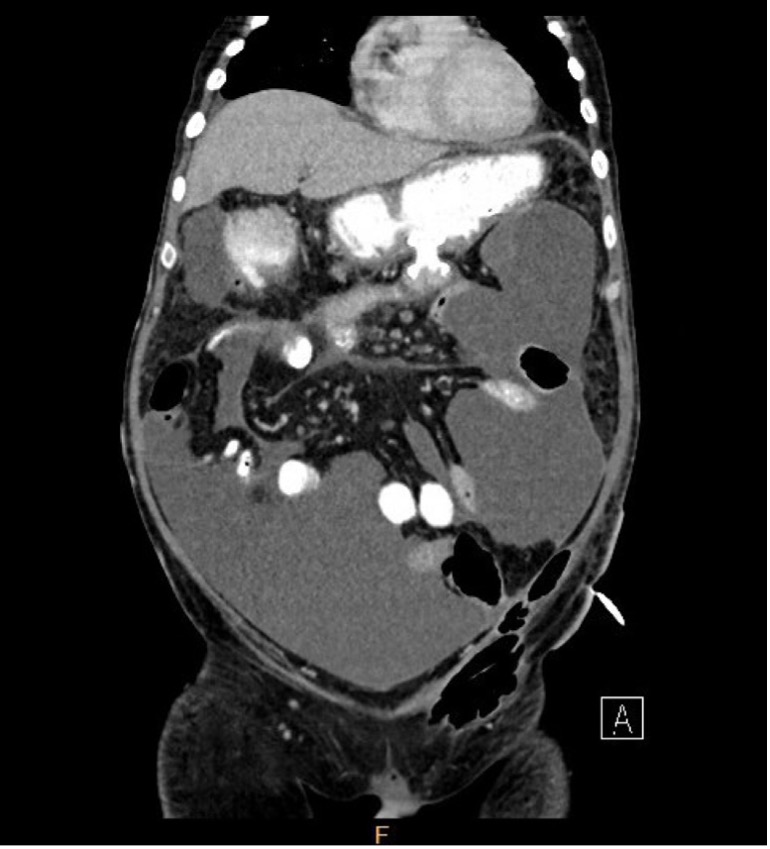
Case Presentation: A 61-year-old male with PMH of sleep apnea was re-admitted to the hospital 3 weeks after a laparoscopic cholecystectomy secondary to gallstones and 1 week after an episode of acute pancreatitis with necrotizing pancreatitis and a large walled off necrotic peripancreatic collection. He underwent EUS guided cystgastrostomy with gastric and duodenal stenting and has had 6 subsequent endoscopic necrosectomies. His prolonged hospitalization has been further complicated by small bowel obstruction, multiple retroperitoneal abscesses (MRSA and Enterobacter cloacae) requiring numerous intraabdominal drains, and multiple ICU admissions for hemorrhagic and septic shock. Four months into his hospitalization, he continued to have severe abdominal pain and developed worsening abdominal distention and lower extremity edema. Repeat imaging revealed large volume ascites with enhancement of the peritoneum that was not seen on CT just one week prior. Paracentesis was performed and revealed chylous ascites with triglyceride content of 424 mg/dL. Ascitic fluid amylase, cultures, and cytology were normal.
Discussion: Chylous ascites (CA) is an uncommon clinical finding when lymph accumulates in the peritoneal cavity causing ascites. The ascitic fluid is milky appearing with a high triglyceride content (>200 mg/dL). CA is a rare cause of ascites, with trauma, abdominal malignancy, and cirrhosis accounting for most cases in developed countries, and infectious etiologies (tuberculosis or filariasis) being most common in developing countries. There are few cases in the literature describing CA secondary to necrotizing pancreatitis. The underlying pathophysiology is thought to be the result of severe inflammatory changes causing disruption to the thoracic duct or lymphatic system. Clinical consequences include dehydration, electrolyte imbalance, malnutrition, and immune suppression. Management of CA is challenging when the underlying cause is not easily treatable. The few described cases in the literature of necrotizing pancreatitis causing CA have shown some response to parenteral nutrition with medium chain triglycerides (which are absorbed directly by intestinal cells and bypass the lymph system) alone or in combination with octreotide. Some cases require serial paracentesis and diuresis for symptomatic relief. Our patient received diuresis and had 2 paracenteses which provided some symptomatic improvement. However, due to strong family preference to avoid parenteral nutrition, he continued to receive enteral nutrition with medium chain triglyceride formula. Octreotide was not given due to lack of clear data showing benefit in setting of potential adverse side effects. Unfortunately, he continued to experience recurrent complications and ultimately transitioned to hospice. Because CA is a rare consequence of pancreatitis, further study is needed as the evidence for improvement with parenteral nutrition and octreotide remains anecdotal, and no studies have shown an optimal therapeutic approach.
Conclusions: Chylous ascites is an uncommon cause of ascites, and a rare complication of necrotizing pancreatitis. Accumulation of lymph in the abdominal cavity can lead to dehydration, electrolyte derangements, and immunosuppression, thus making recognition and management essential for hospitalized patients to mitigate further complications.