Background: Although 88% of inpatients with falls do not sustain injuries, those with fall-related injuries experience limitations in activities of daily living, residual disabilities, and additional medical costs. Therefore, predicting fall-related injuries is crucial. We previously developed a prediction model for fall-related injuries, the Saga Fall Injury Risk Model (SFIRM), in an acute care hospital as follows: Score = −8.672 + 0.034 × (age) + (sex: female = −0.641) + (emergency transport: presence = −0.887, missing = −0.551) + (medical referral letter: presence = 0.399, missing = 1.189) + (history of falls: presence = 0.542) + (bedriddenness rank: J = 1.597, A = 2.188, B = 1.986, C = 1.510, others = 0.154). The area under the curve (AUC) of SFIRM for internal validation was 0.772. We conducted external validation to assess the precision of SFIRM using data from several hospitals. Additionally, to enhance the model’s accuracy through redevelopment, we investigated the common predictors of fall-related injuries across diverse hospital settings.
Methods: This retrospective observational study included inpatients aged 20 years or older who were admitted to eight hospitals, including chronic, acute, and tertiary acute care hospitals, between April 2018 and March 2021. A random sample of appropriate size was selected from the entire dataset, and the AUC of the SFIRM was calculated.Facility-specific analyses were conducted using datasets from each of the eight hospitals. The AUC of the SFIRM was calculated for each hospital. To identify common predictors, eight multivariate analyses (logistic regression analysis, forced entry method) were performed using selected variables as explanatory variables with collinearity considered and fall-related injury as the outcome variable. To identify common predictors of fall-related injuries, significant variables from each analysis were compared across hospitals.
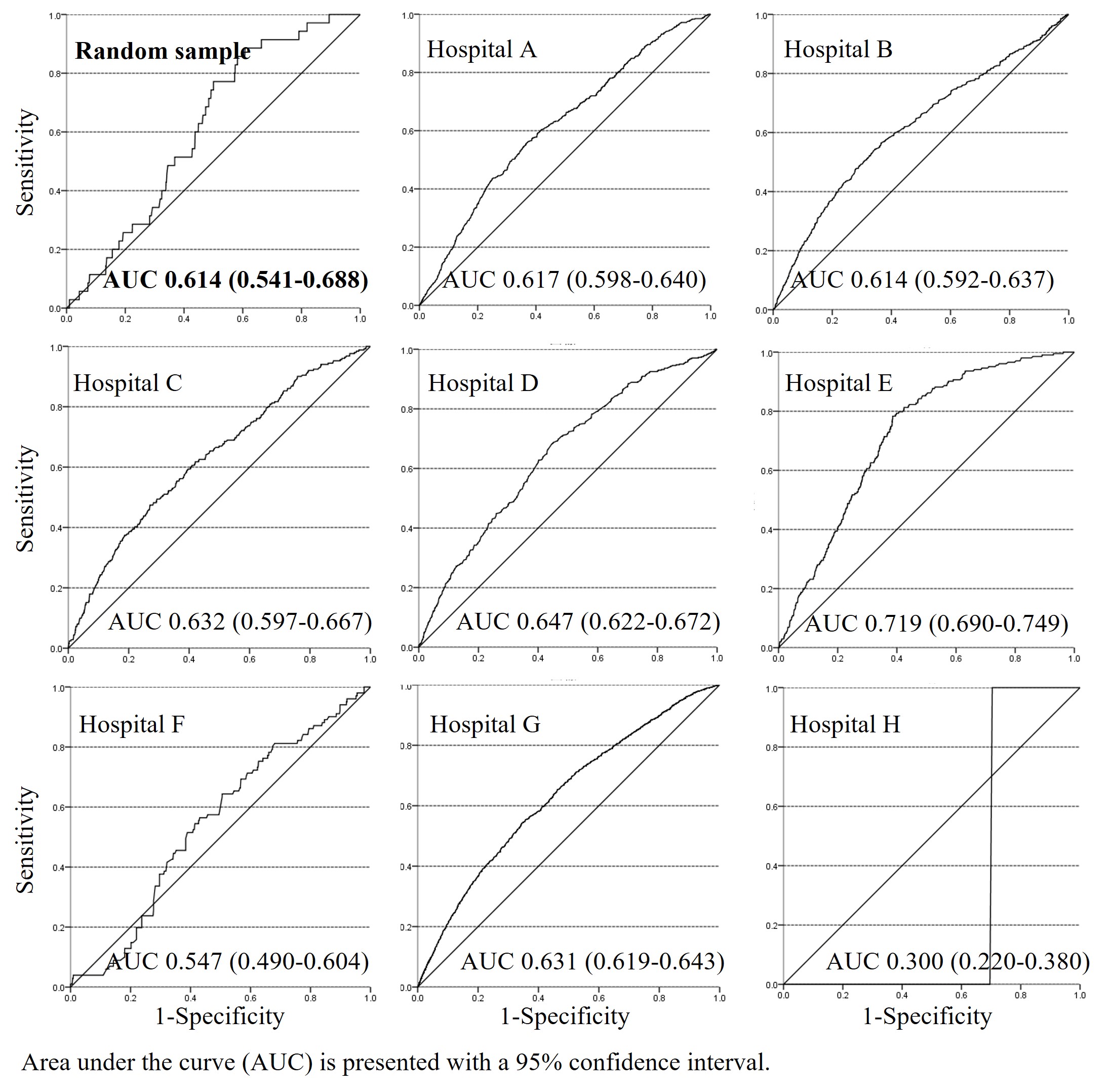
Results: From 144,777 patients, 2,376 were randomly selected for analysis. The median age was 70 years (interquartile range, 58–78), 1280 patients (54%) were male, and the median hospital stay was 9 days (4–16). Falls occurred in 51 patients (2.1%), and fall-related injuries occurred in 35 patients (1.5%). Among the injured patients, the median age was 76 years (66–86), 19 (54%) were male, and the median hospital stay was 26 days (16–47). The AUC for the SFIRM among all patients was 0.614 (95% confidence interval, 0.541–0.688).Facility-specific analyses indicated AUC ranging from 0.300–0.719 (Figure 1). In multivariate analyses, using 23 parameters as covariates, age and bedriddenness rank were found to be common predictors for fall-related injury across five hospitals, and male sex and diabetes across four hospitals.
Conclusions: External validation among patients with diverse backgrounds demonstrated that the discrimination of the SFIRM was lower than that observed in internal validation, suggesting a need for redevelopment and validation. Inaccuracies in the SFIRM parameters in some hospitals may have undermined the overall discrimination of the model.Significant predictors consistently identified across hospitals included age, male sex, bedriddenness rank, and diabetes. These four items have been repeatedly reported as factors associated with falls or fall-related injuries and could serve as key parameters in a simple prediction model for fall-related injuries.