Background: With increasing integration of technology in healthcare, understanding factors influencing older adults’ willingness to adopt mobile health (mHealth) applications is crucial. This study aims to investigate the demographic, clinical, and behavioral factors associated with willingness to try an mHealth app among older adults.
Methods: We conducted a mixed methods study at a large tertiary academic medical center from July to August 2024. We screened and invited hospitalized medical patients aged 62 years and older who had been admitted for at least 2 days to participate. Patients with moderate to severe cognitive impairment were excluded. Using a standard questionnaire, we interviewed participants about their current personal device use and assessed digital literacy by testing their ability to set an alarm on their personal mobile device. Participants who did not have their personal smartphones available during the digital literacy assessment were classified as “Not Applicable”. Participants were asked if they would try an mHealth app promoting physical activity during hospitalization. Interview responses, digital literacy assessment, demographic data, and clinical data were compared between those willing to try the app and those unwilling. Statistical analyses included Fisher’s exact test and Welch Two Sample t-test, with significance set at p < .05.
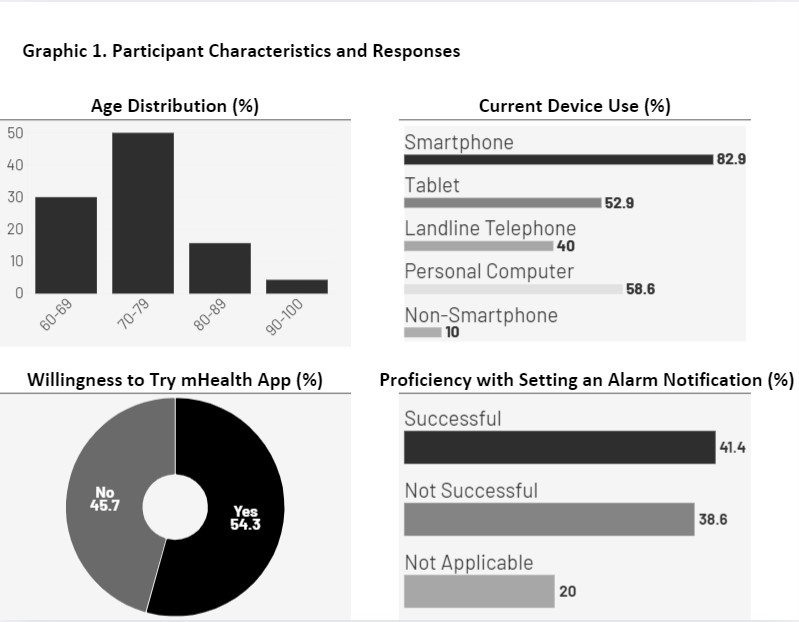
Results: Of 81 screened and invited patients, 70 (86.4%) agreed and were interviewed. Among them, 38 (54.3%) were willing to try the mHealth app while 32 (45.7%) declined. Those willing to try the app were younger (median age, 73 years [IQR, 68-76 years] vs 75 years [70-79 years], p=.15), had higher comorbidity burden (median Charlson Comorbidity score, 8 [QIR, 5-10] vs 6 [IQR, 4-7], p = .01), were more likely to have completed education beyond high school (84.2% vs 58.1%, p=.03), and were less likely to have history of dementia (0% vs 12.5%, p=.04). Sex distribution (% females, 52.6% vs 50.0%, p>.99) and median BMI (29.7 [IQR, 24.5-32.7] vs 28.4 [IQR, 23.9-31.2], p=.63) were similar between the two groups. Overall, 84% of patients owned a smartphone. Smartphone ownership was more common among participants willing to try the app than among those unwilling (89% vs 75%, p=.13). Personal computer ownership was 58.6% in the overall cohort and was higher among those willing to try the app, 71.1% vs 43.8%, p=.03. Compared to participants unwilling to try the app, those willing to try the app were more comfortable using a smartphone in general (89.5% vs 67.7%, p=.04), searching for information (86.8% vs 62.5%, p=.03), using the calendar (57.9% vs 28.1%, p=.02), and using the alarm or reminder notification function (50% vs 21.9%, p=.02). Participants willing to try the app were also more successful in demonstrating their ability to set an alarm notification (63.2% vs 15.6%, p<.001).
Conclusions: More than 3 in 4 older adult hospitalized patients own smartphones, and the majority are willing to try an mHealth app promoting physical activity during hospitalization. Those willing to try were younger, had a higher level of education, utilized more smartphone functions, and were more proficient in setting an alarm notification. These findings underscore the importance of creating easy-to-use mHealth applications designed with the older adult patient in mind. Tailoring apps to the needs and preferences of older adults could significantly enhance their adoption and effective use in healthcare settings.