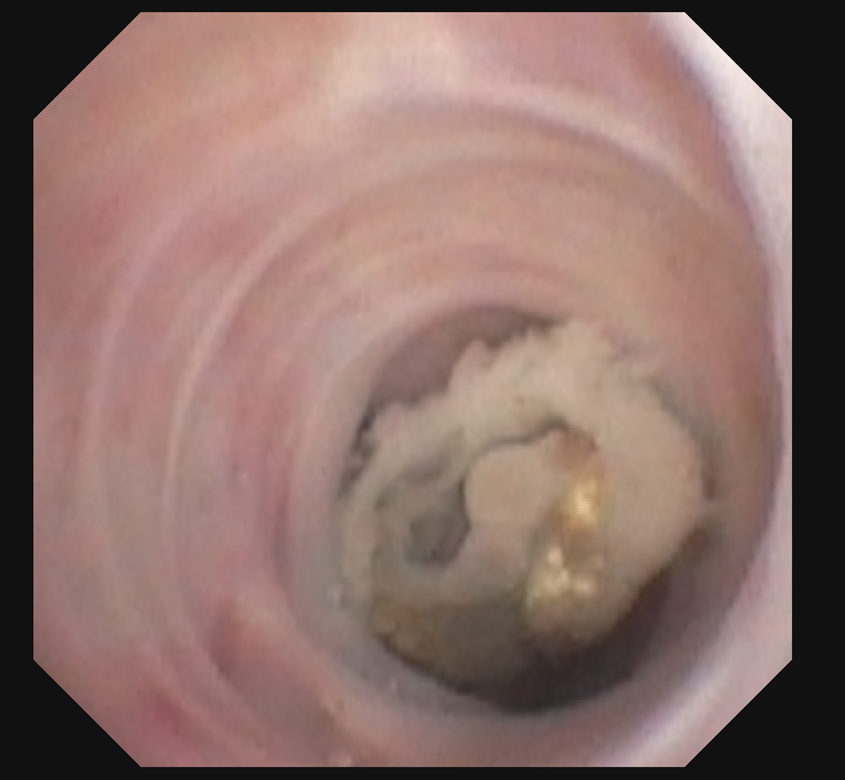
Case Presentation: A 56-year-old female with a prior history of acute myeloid leukemia, status-post allogenic stem cell transplant in 2016 (in remission), complicated by chronic graft versus host disease (on mycophenolate), and pulmonary coccidioidomycosis in 2000 presented due to hemoptysis. She experienced 7 days of blood-tinged sputum with upper respiratory symptoms preceding that. Five weeks prior, she received azithromycin for presumed pneumonia. Upon presentation, she was afebrile and tachycardic, but vitally stable. Workup showed a normal hemoglobin, an elevated white count of 13.4 x 109/L with slightly increased lymphocytes, monocytes, and basophils, along with marked eosinophilia.D-Dimer was found to be elevated. Therefore, a CT chest angiogram was acquired, which was negative for an acute pulmonary embolism. However, it revealed a nodular lesion in the anterior left upper lobe with distal bronchiectasis and mucous plugging. Review of prior imaging showed the presence of this nodule since at least 2016. A bronchoscopy was performed, which showed an endobronchial lesion in the corresponding left upper lobe area where the nodule was seen, with green necrotic debris. The patient was presumed to have invasive pulmonary aspergillosis; however, fungal cultures returned positive for Scedosporium species complex with mycetoma shown on biopsy. Serum and bronchoalveolar lavage aspergillus antigen were negative. Coccidioides, Blastomyces, and Histoplasma studies were negative. She was treated with voriconazole. After her diagnosis, she reported a remote history of fungal lung infection. She was also treated with cefepime for presumed superimposed bacterial infection. Less than three weeks after discharge, on follow-up with infectious disease outpatient, the cough and hemoptysis resolved. Repeat chest CT showed an interval decrease in the left upper lobe endobronchial nodule. The treatment plan was to continue voriconazole for at least 6 months.
Discussion: Scedosporium are fungi/mold that are present in soil and polluted areas and can cause opportunistic infections. They most commonly affect the respiratory tract and can lead to invasive disease and fungemia. Due to this, they are associated with high mortality rates. Hemoptysis, as seen with this patient, was the most common symptom in one review. The marked eosinophilia was indicative of fungal disease. Clinically, Scedosporium infection can be mistaken for aspergillosis by way of history, imaging, and pathology; therefore, cultures are critical in distinguishing Scedosporium from Aspergillus. Voriconazole has shown improved survival compared to liposomal amphotericin B and itraconazole and is the first-line treatment, as well as surgical debridement.
Conclusions: In patients presenting with hemoptysis and a markedly elevated eosinophil count, fungal disease should be on the differential. Even when the diagnosis may seem to be aspergillosis, it is prudent to obtain a fungal culture to assess for Scedosporium; particularly in immunosuppressed patients, such as this patient, but should also be considered in immunocompetent patients.