Background:
The landmark article on “application of external cardiac massage” published in 1961 reported survival to discharge in 24% of patients sustaining cardiac arrest. Cardiopulmonary resuscitation (CPR) emerged as a strategy of care for “hearts too young to die,” with the goal being neurologic viability. Given the changes in prehospital care, improved outcomes, and mortality in patients with cardiovascular diseases and other diseases, balanced with the dissemination of advanced directives, this study explored the profile of patients commonly being resuscitated 50 years later to examine whether we were actually limiting CPR to hearts “too young to die.”
Methods:
Over a period of 24 months, we evaluated 45 consecutive survivors of nontraumatic out‐of‐hospital cardiac arrest. Data were collected according to a standardized protocol following the Utstein guidelines. The subgroup with “hearts too young to die” (group A) was defined as having age < 75 years, ventricular fibrillation/ventricular tachycardia as the initial arrest rhythm, and an interval of collapse–return of spontaneous circulation < 20 minutes. Group B constituted the rest of the cohort.
Results:
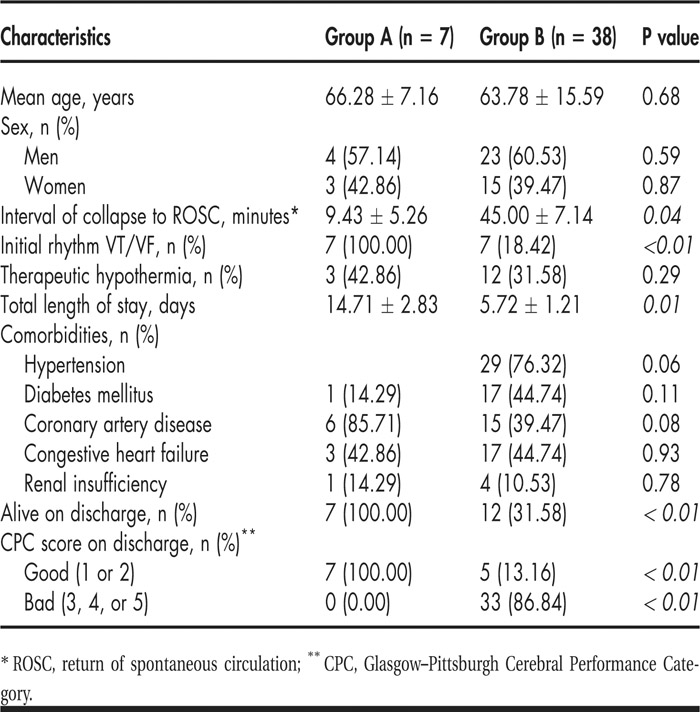
Overall survival to discharge in this study was 42.22% (19 of 45); however, selecting patients with “hearts too young to die” increased the survival rate to 100% (group A) versus 31.58% (group B); P < 0.01 (see Table 1).
Conclusions:
These data suggest that patients with “hearts too young to die” are in a conspicuous minority but continue to be effectively resuscitated with excellent neurological outcomes. However, CPR is most often performed in patients who do not have viable heart rhythms, and although they may survive to discharge, they are often severely impaired. We concluded that the original premise of CPR has been abandoned, with no obvious evidence of benefit to the extended population.
Disclosures:
S. M. Eid ‐ none; U. Lakshmanados ‐ none; D. Dobrosielski ‐ none; J. M. Palachuvatil ‐ none; S. M. Carey ‐ none; K. J. Stewart ‐ none; N. Chandra‐Strobos ‐ none