Background: Physicians increasingly utilize electronic health records (EHR) to deliver healthcare, and the EHR has been identified as leading source of physician burnout and frustration [Shanafelt et al]. Studies report up to 52.6% of hospitalists exhibit symptoms of burnout [Roberts et al]. However, there is no data to inform how hospital medicine physicians spend their time in EHRs. We sought to understand how hospital medicine physicians partition their time within the EHR as well as the variability among physicians.
Methods: We conducted a retrospective cohort study of 44 full time equivalent, day-shift hospital medicine physicians performing direct patient care at our hospital, which uses Epic EHR. We obtained each hospitalist’s Epic activity logs for six non-consecutive months between March 2017 and March 2019. Practitioners who were responsible for admitting patients, consulting, moonlighting, or on teaching team with residents for more than 10% of their total shifts within the study periods were excluded from analysis. If a provider worked a number of different shift types within the same month, only hospitalists who conducted daytime, direct care, rounding shifts for 80% or more of a given month were included. Physicians on rounding shifts have on average 14 patient encounters each day. We ranked physicians by total time spent interacting with the EHR and divided them into quartiles. Descriptive analysis was performed using SAS statistical software.
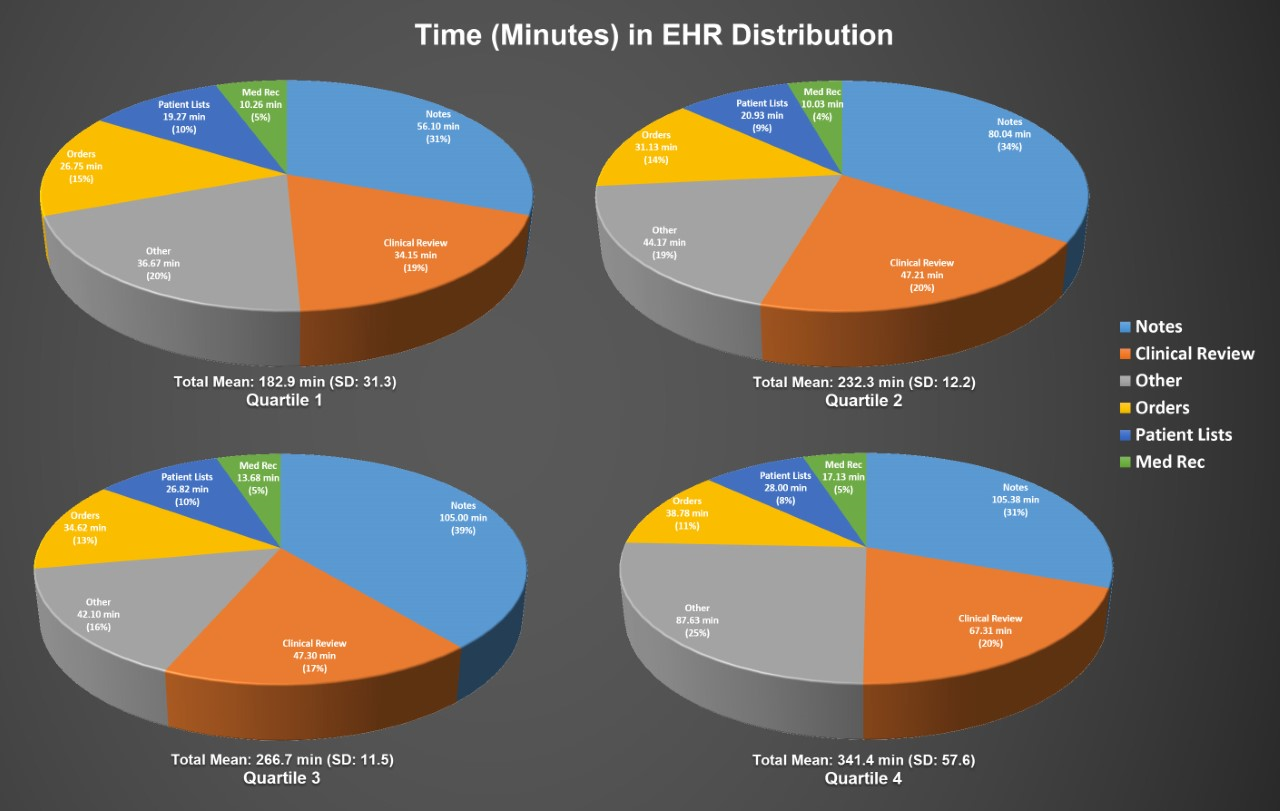
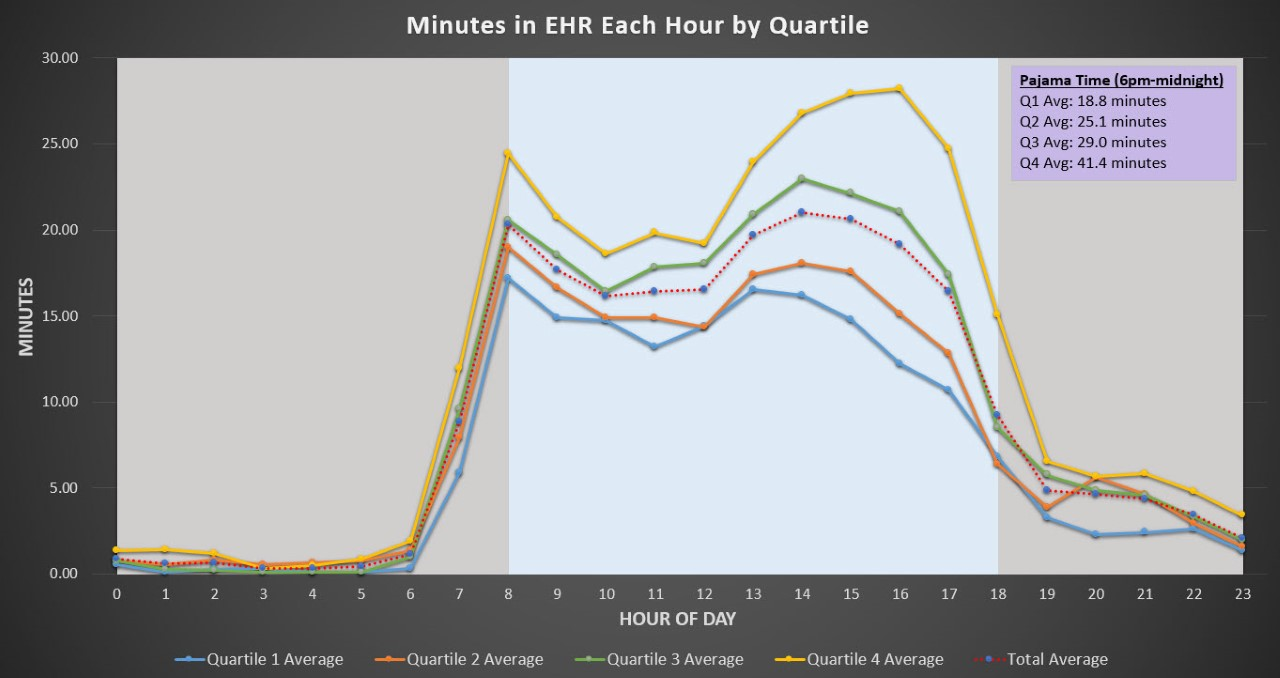
Results: We found that hospital medicine physicians at our institution spend a mean of 4.3 hours (± 66.9 minutes) a day in the EHR with a range of 2.2 hours/day to 7.4 hours/day in the EHR. Physicians in the top quartile spent a mean of 3.0 hours ± 31.3 minutes/day in the EHR while physicians in the bottom quartile spent a mean of 5.7 hours ± 57.6 minutes/day in the EHR, with nearly twice as much time in note writing and clinical review. Physicians in the top quartile spend 56 minutes, on average, writing notes while physicians in the bottom quartile take nearly 50 minutes longer, on average, to complete their notes (Figure 1). Physicians spent the most time in the EHR writing notes (mean 86.6 ± 39.9 minutes) and in clinical review (49.0 ± 18.6 minutes), followed by time writing orders (32.8 ± 10.0 minutes) and navigating patient lists (23.8 ± 7.6 minutes) (Figure 1). Physician time in the EHR showed a bimodal distribution with a sharp peak at 0800 and a second, flatter peak between 1300 and 1600 (Figure 2). On average, physicians spend 18.8 (Q1) to 41.4 (Q4) minutes in the EHR between 1800 and 0000 (“pajama time”).
Conclusions: For the same tasks, there is large intragroup variation amongst hospital medicine physicians in EHR usage and efficiency. Hospitalists spend a significant amount of “pajama time” in the EHR, potentially contributing to burnout. It is not clear whether those who spend less time in the EHR do so at the cost of quality. EHR customization and EHR proficiency have been suggested to prevent burnout [Dastagir et al]. Physicians who are able to minimize time in the EHR and maintain high quality clinical review, documentation, and patient care may be able to share their EHR practices to optimize the value of time spent in the EHR for others and minimize burnout associated with the EHR.