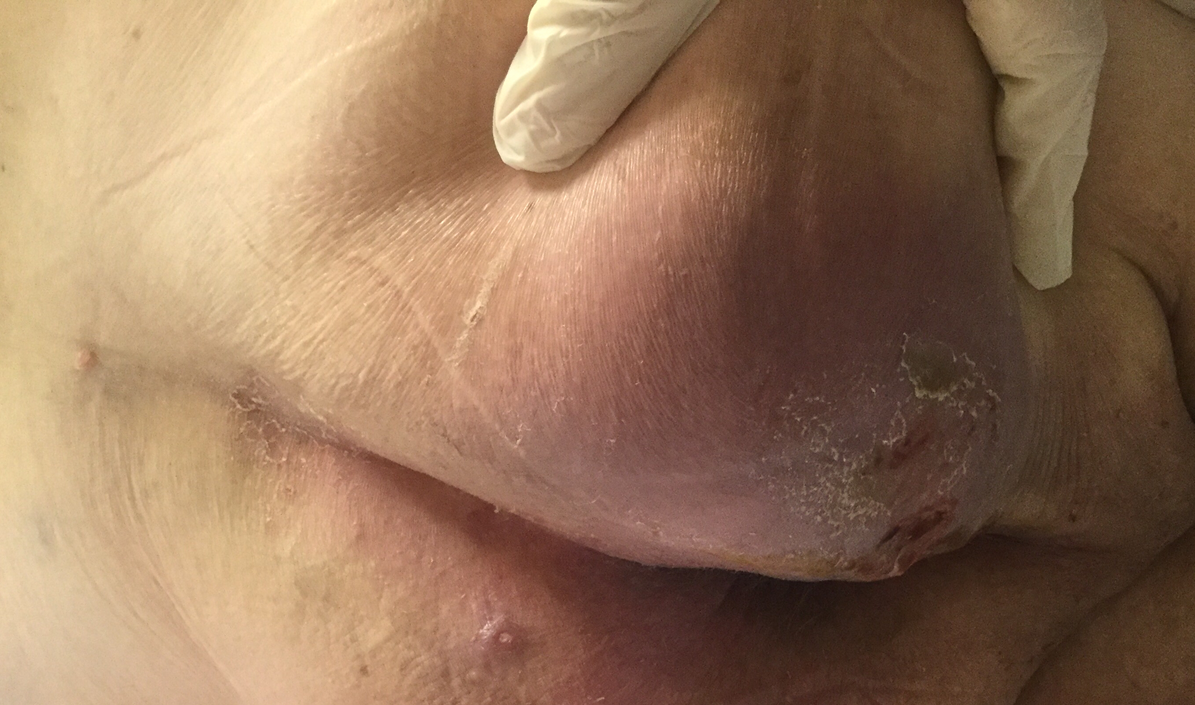
Case Presentation: A 76-year old man presented to emergency department for 2-week history of right buttock pain, swelling, and drainage. On presentation, he had a temperature of 101.3 F, otherwise hemodynamically stable. Physical examination revealed right buttock erythema and serosanguinous purulence (figure). There were no cardiac murmurs. Leukocytes count was within normal limits. CT abdomen and pelvis demonstrated subcutaneous inflammation consistent with right gluteal cellulitis without no abscess. Empiric antimicrobial therapy included IV vancomycin, cefepime, and metronidazole. Next day, blood cultures grew methicillin-resistant Staphylococcus aureus (MRSA). There were no valvular vegetations on echocardiogram. Few days later, the patient developed left eye pain and blurry vision with subsequent loss of vision in left eye. Ophthalmology evaluation revealed chemosis, conjunctival injection, 4+ anterior chamber cells, hypopyon, , consistent with endophthalmitis. Intravitreal vancomycin and ceftazidime were administered and intraocular cultures were sent (reported negative). The patient was discharged with 4-week course of IV daptomycin and ophthalmology follow up. He subsequently underwent complex retinal detachment repair and vitrectomy with slight improvement in visual acuity (able to count fingers from 2 inches).
Discussion: Endogenous endophthalmitis, also known as malignant endophthalmitis, is an uncommon but potentially devastating infection secondary to hematogenous seeding of pathogens. It accounts for 2 to 15% of all endophthalmitis cases. There is no age or sex predilection. Although it is caused by hematogenous spread, endogenous endophthalmitis tends to develop unilaterally. In general, gram negative organisms, especially Klebsiella pneumoniae, are responsible for most cases in East Asia, whereas, gram-positive organisms are the more frequent agents in North America. A high degree of suspicion is necessary to make an early diagnosis. Patients usually complain of eye pain, blurring of vision and ocular discharge. The diagnosis is established by clinical findings consistent with endophthalmitis with positive blood cultures or by positive vitreous or aqueous cultures. Blood cultures are positive in 75% of cases, as are vitreous cultures. Sources of bacteremia include endocarditis, skin infections, and procedures that may cause transient bacteremia. The treatment includes intravitreal and systemic antibiotics. Given the virulent nature of pathogens involved, vitrectomy is also indicated with antimicrobial therapy.
Conclusions: Endogenous endophthalmitis is a vision-threatening medical emergency. This case highlights how a seemingly benign skin infection can quickly evolve into a serious complication. It is important to consider endophthalmitis in the differential diagnosis in patient reporting acute onset vision changes in the setting of bacteremia, as prompt ophthalmological consultation can prevent potential vision loss.