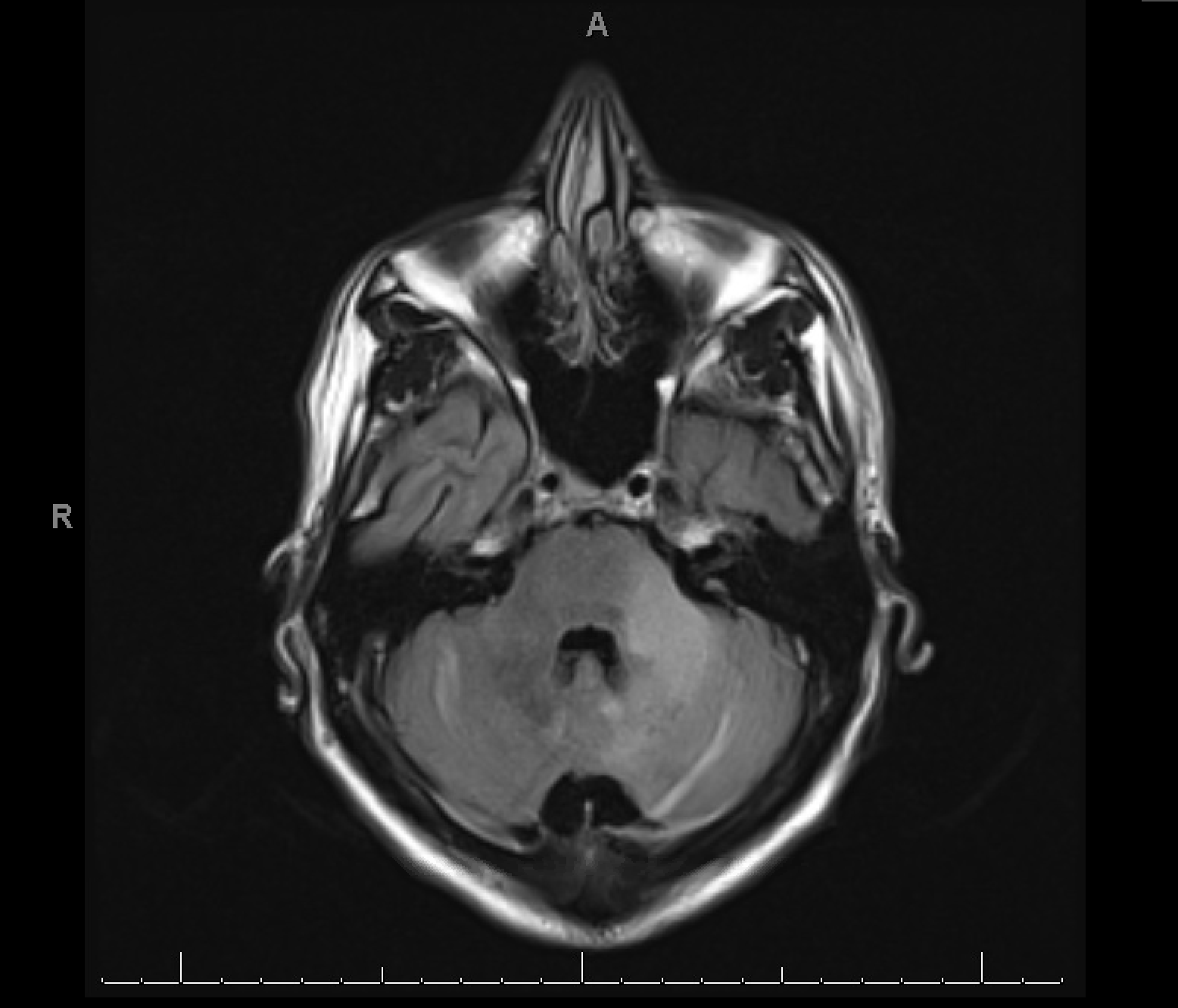
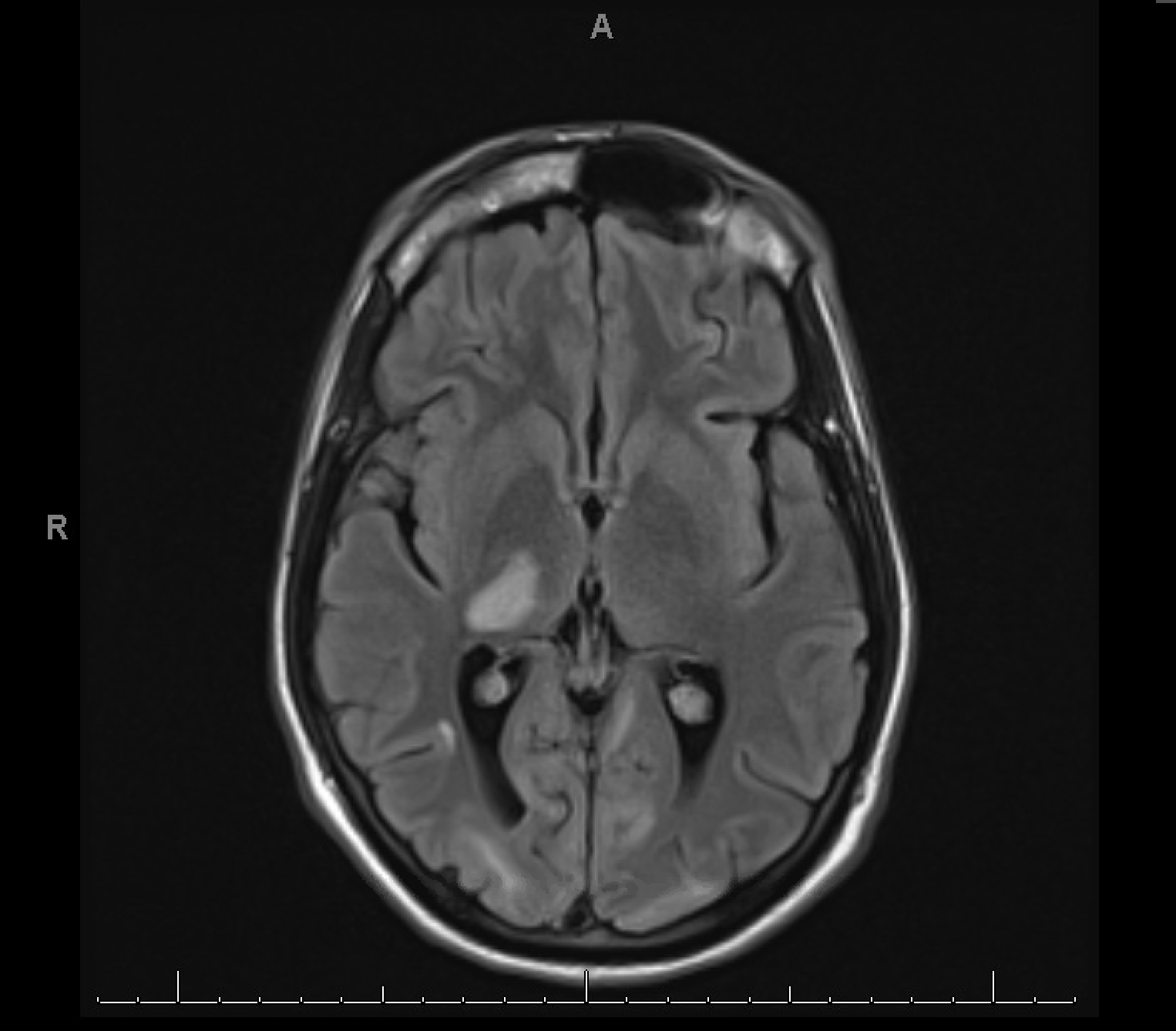
Case Presentation: A 33-year-old male without significant medical history experienced visual changes, left-sided tingling and weakness, vertigo, nausea, and mild expressive aphasia for 2 months. At that time, he had mild upper extremity tremor and was able to walk, drive, and perform activities of daily living. On physical exam, the patient demonstrated left upper extremity dysdiadochokinesia, bilateral upper extremity dysmetria, slowed speech, and extreme nausea and vomiting. Lower extremities showed bilateral dysdiadochokinesia although no dysmetria. He had moderate strength (3-4/5) throughout, although movements were limited by severe nausea. The patient denied intravenous drug use (IVDU) or male sexual partners, but reported having multiple female sexual partners.His primary care physician had ordered magnetic resonance imaging (MRI) for suspected multiple sclerosis, which showed demyelination and a large left cerebellar lesion with high signal intensity on T2/FLAIR. Smaller lesions with similar characteristics were present in the cortex of the right thalamus, bilateral occipital lobes, right parietal lobe, and left frontal lobe. In the inpatient setting, a human immunodeficiency virus (HIV) test was positive with a CD4 count of 35 cells/μL. Positive cerebrospinal fluid polymerase chain reaction for John Cunningham (JC) virus confirmed the diagnosis of progressive multifocal leukoencephalopathy (PML).
The patient was started on antiretroviral therapy (ART). He was encouraged to participate in physical and occupational therapy with the hope of optimizing his functional ability. He was closely monitored in the hospital for signs of immune reconstitution inflammatory syndrome (IRIS).
Discussion: PML is caused by JC virus reactivation, almost exclusively manifesting in immunodeficient patients and most often affecting those with CD4 counts < 200 cells/μL. The disease causes white matter demyelination by infecting glial cells, although newer reports have shown demyelination in gray matter and viral infection of neurons. The neurologic sequelae of disease are thus variable and dependent on lesion burden and location. ART has improved outcomes in patients with HIV-associated PML, despite initial clinical deterioration. This deterioration is due to IRIS, where CD4 T-cell counts increase and HIV viral loads decrease.
Conclusions: This patient was a unique case of a first-time HIV diagnosis presenting with PML. His nonspecific neurologic presentation and lack of common risk factors (e.g. IVDU, male sexual partners) serve as a warning for clinicians to broaden their suspicion for HIV. We advise clinicians to consider HIV testing on patients presenting with unexplained neurologic symptoms.