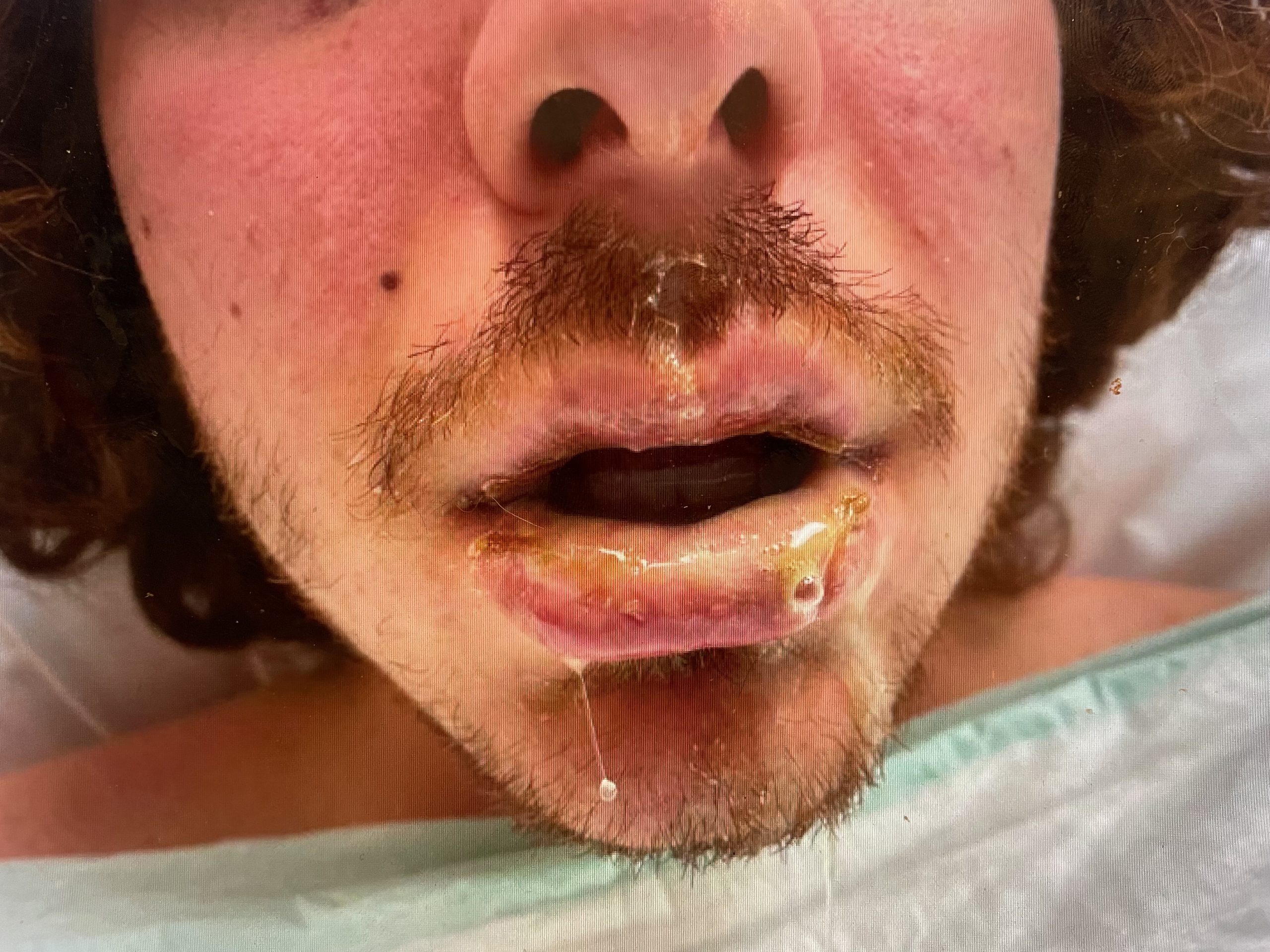
Case Presentation: A 22-year-old man with a history of recurrent oral ulcers presented with severe oral pain and ulcers following a recent respiratory illness. He had initially developed a cough and sore throat one week prior. Soon after, he experienced progressive oral ulcers, resulting in profound difficulty speaking and eating due to pain. He reported no new medications. Vitals were notable for temperature of 102.3°F. Physical examination was notable for bilateral conjunctivitis, severe intraoral erosions, and mucositis with sloughing along his soft and hard palate, lips, and tongue. There was no additional skin involvement over the rest of his body. Laboratory testing revealed mild leukocytosis, and chest radiography was normal. Swabs of the oral lesions tested negative for herpes simplex virus (HSV) and varicella zoster virus (VZV). A nasal swab viral PCR was positive for Mycoplasma pneumoniae and Mycoplasma serologies showed positive IgM and IgG antibodies. He was diagnosed with reactive infectious mucocutaneous eruption (RIME) and was treated with intravenous steroids and a steroid mouth rinse in addition to azithromycin for his Mycoplasma infection. During his hospital stay, he experienced dysuria and hematochezia, both attributed to RIME affecting the urinary and rectal mucosa, respectively. His mucositis improved over the next three days, and he was discharged with an oral steroid taper.
Discussion: RIME is a severe mucocutaneous eruption that occurs in response to an infectious trigger, predominantly in the pediatric or adolescent population (1). While it is most seen with Mycoplasma pneumoniae infections, it can also occur following other bacterial or viral respiratory infections (2). It is characterized by a prodrome of cough, malaise and fever that is followed approximately a week later by mucositis and variable vesiculobullous cutaneous lesions. The mucositis is often severe and can present as purulent conjunctivitis, urogenital or anal lesions, hemorrhagic crusting of the lips, tongue, and buccal mucosal erosions (1). While the differential diagnosis for oral ulcerations can be broad and include aphthous ulcers, various viral infections such as HSV and coxsackie, autoimmune blistering conditions, and drug reactions such as Stevens-Johnson syndrome (SJS) or toxic epidermal necrolysis (TEN), our patient was ultimately diagnosed with RIME. Management of RIME includes supportive care for any mucosal or skin involvement with occlusive ointments, oral and eye care, nutritional support, and pain management. In addition, systemic corticosteroids to decrease inflammation and empiric antibiotics with coverage against M. pneumoniae are frequently used (1). Our patient had the classic features of RIME with his presentation — a preceding Mycoplasma upper respiratory infection, negative drug exposures, and involvement of multiple mucosal membranes — and intravenous steroid therapy and antibiotics were initiated early in his course with good clinical improvement.
Conclusions: Hospitalists frequently encounter oral ulcerations as a common patient complaint. While the differential is broad, severe oral ulcerations following a respiratory illness should prompt consideration of RIME. Early recognition of this clinical syndrome and initiation of corticosteroid and antibiotic therapy is crucial.