Case Presentation:
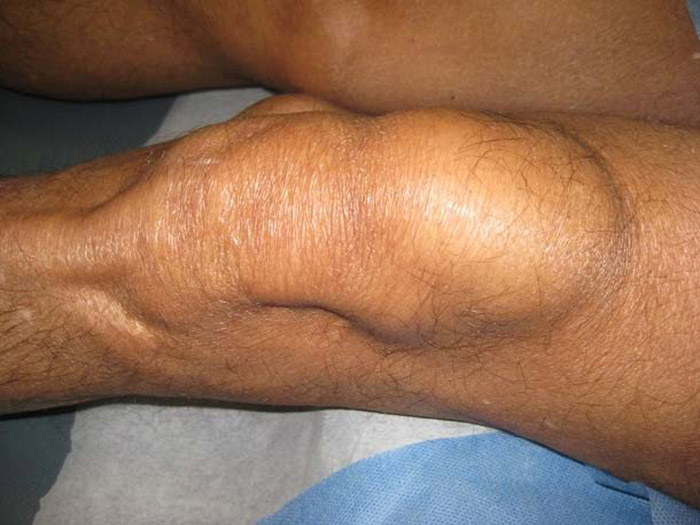
A 74 year‐old Venezuelan man presented to the emergency room with a one‐year history of tender masses on both arms and legs. He had also experienced fever, night sweats, and thirty‐five pound weight loss over the past year. In addition, he endorsed mild dyspnea on exertion. On exam, he had sunken cheeks and appeared emaciated. There were no palpable lymph nodes. There were crackles heard at both lung bases. No organomegaly was appreciated. He had large, oval, indurated, tender, subcutaneous nodules on the extensor surfaces of both forearms and on the anterior and medial aspects of his left and right knee. On laboratory evaluation, he was noted to have mild anemia, mild thrombocytosis, and normal leukocyte count with monocytosis. Fungal serology and Quantiferon were negative. Chest x‐ray and CT Chest revealed diffuse fine parenchymal infiltrates. Plain films of the long bones were normal. Biopsy of the left knee nodule revealed extensive noncaseating granulomatous inflammation with giant cells. Special stains for mycobacterium and fungi were negative.
Discussion:
Sarcoidosis is not a common disease, however its presentation should be familiar to the hospitalists as they will likely diagnose it in their lifetime. It can affect almost any organ system. Pulmonary complaints of dyspnea on exertion, cough, and chest pain are the most commonly encountered symptoms. Systemic symptoms of fever, weight loss, and anorexia are seen in about half of the patients. Skin nodules are not as common, however, these can easily be biopsied for possible diagnosis. Diagnosis is made by clinical and radiographical manifestations, exclusion of other diseases, and biopsy of the most accessibly involved organ. In almost all cases, chest x‐ray will be abnormal, showing bilateral hilar lymphadenopathy, interstitial infiltrates, or fibrocystic lung disease. Histology reveals noncaseating granulomatous inflammation. The diagnosis requires evidence that granulomatous inflammation is present in at least two organs, but biopsy of both is not required. As in this patient, he had evidence of granulomatous inflammation on skin biopsy as well as a typical chest x‐ray for stage three pulmonary sarcoidosis.
The most important diseases to exclude when evaluating a patient for sarcoidosis are malignancies and infectious granulomatous diseases. Lymphoma and lung cancer should be excluded during the work up when hilar or mediastinal lymphadenopathy is present. Testing includes transbronchial needle aspiration, endobronchial ultrasound guidance, or thorascopic biopsy if necessary. Infections like tuberculosis and fungi should be tested for by serology as well as special stains on biopsy.
The pathogenesis of sacroidosis is unclear, but most evidence suggests that the granulomas are formed in response to environmental, infectious, or occupational agents. Antigens are phagocytosed by antigen presenting cells and then presented to HLA class II molecules on certain T‐cell receptors. This causes cellular recruitment, proliferation, and differentiation as well as dysregulated expression of pro‐inflammatory cytokines leading to formation of the granuloma.
Conclusions:
Sarcoidosis is an uncommon disease with a wide variety of clinical presentations. An understanding of the pathology and diagnosis is important for every hospitalist as they are likely to come across this disease in their career.