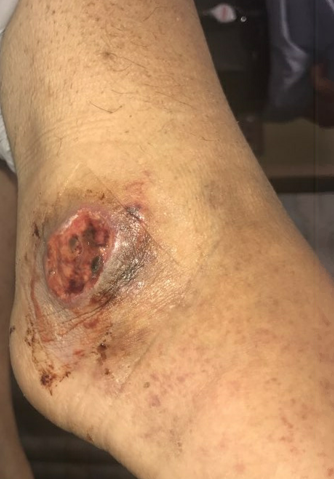
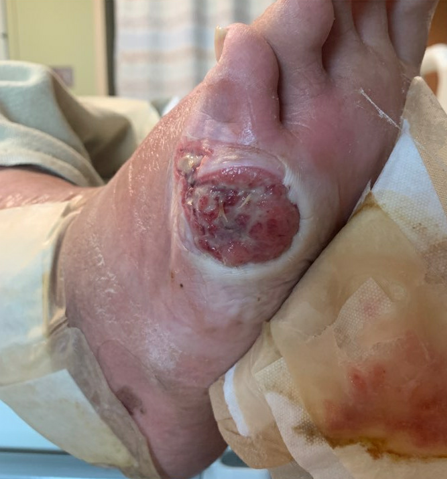
Case Presentation: A 28-year-old female with a known history of seropositive rheumatoid arthritis presents with a non-healing ulcer on her right ankle. She received local wound care and antibiotics for three months prior to this admission. She also complained of increasing pain and stiffness in the small joints of hands and feet as well as numbness, paresthesia, and increasing lower extremity weakness. On admission, Temperature 99.8 F, HR 148/minute, BP 175/119 mmHg, and RR 20/min. On exam, there was retiform purpura and livedo reticularis on the upper and distal lower extremities, respectively. There were two circular ulcerating lesions: 1.5 x 1.5 cm on the right lateral malleolus and 2 x 2 cm at the base of the right small toe with well-demarcated borders and deep central ulceration. Neurologic exam revealed motor weakness and diminished sensation in both upper and lower extremities.Labs were significant for ESR 108 (0-20 mm/HR), CRP 28.1 mg/dL (0-0.8 mg/dL), RF 137 IU/mL (0-20 IU/mL), ANA 1:1280, anti-Smith positive, anti-dsDNA positive, anti-RNP positive, C3 38 mg/dL (86-184 mg/dL) and C4 6 mg/dL (20-59 mg/dL). Electromyography (EMG) and Nerve Conduction Study showed asymmetric axonal sensory-motor neuropathy, suggestive of mononeuritis multiplex. Magnetic Resonance Imaging of the ankle was negative for osteomyelitis.In the setting of RA, the clinical picture was consistent with the diagnosis of vasculitis with predominant cutaneous (livedo reticularis and retiform purpura) and neurologic (mononeuritis multiplex) involvement. The non-healing ulcer of the right ankle was also thought to be due to active vasculitis. The patient was started on high dose IV steroids and plasmapheresis. She was then transitioned to Rituximab infusion. On six weeks follow up, there was marked clinical improvement with continued healing of the wound.
Discussion: Non-healing wounds that are non-responsive to standard wound care affects close to 6.5 million people in the United States. Non healing leg ulcers are often due to peripheral arterial disease and venous stasis. It can also be due to vasculitis or autoimmune etiologies. Vasculitis is often diagnosed late. Due to concern for risk of infection, clinicians often delay initiating aggressive immunomodulatory therapy in patients with RA-associated leg ulcers. Early recognition of the active vasculitis is important to initiate targeted biologic therapy in these patients.
Conclusions: This case highlights the importance of considering vasculitis as the cause of non-healing leg ulcers in a patient with rheumatoid arthritis. These ulcers are often refractory to standard therapy including antibiotics and local wound care. In these cases, it is important to escalate immunomodulatory therapy for the management of vasculitis and healing of ulcers.