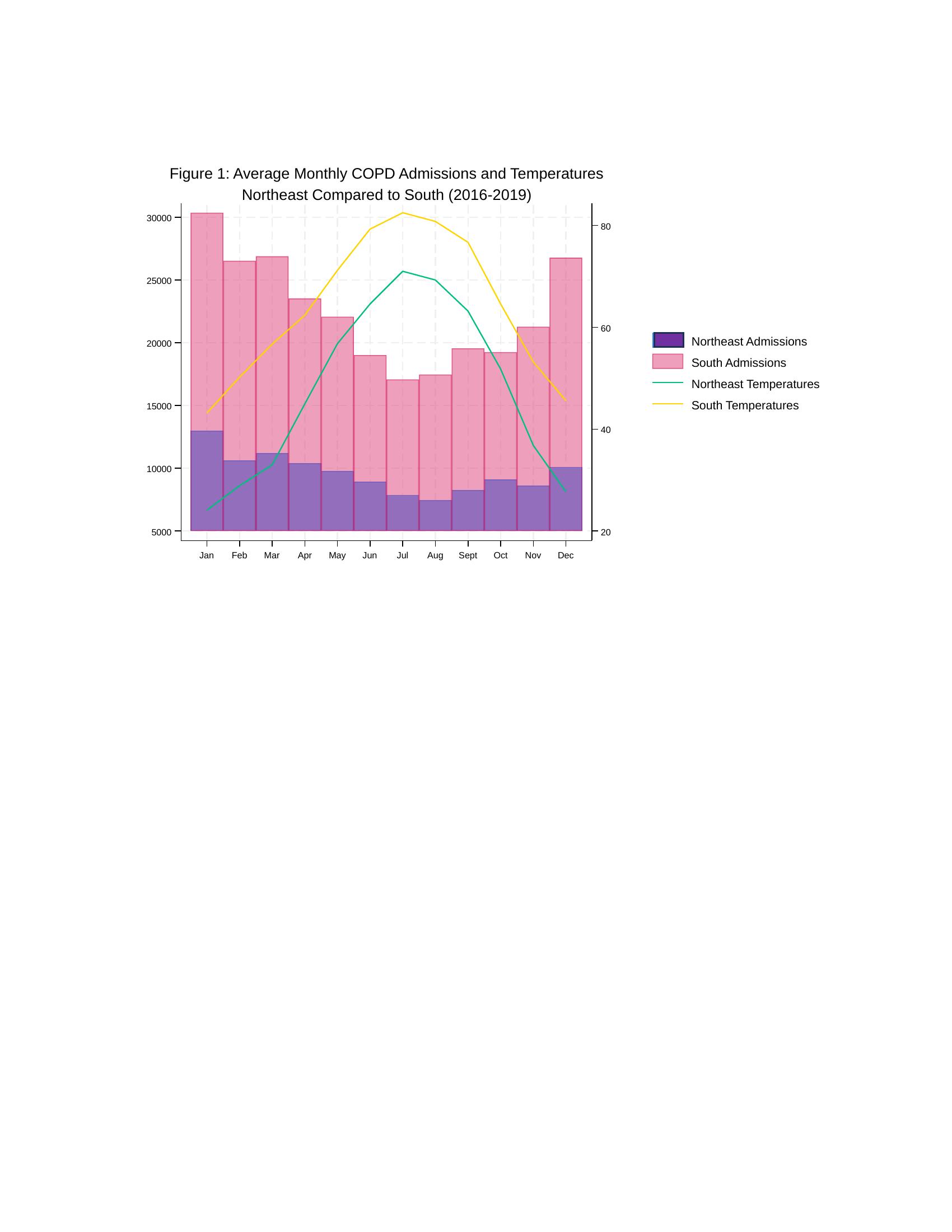
Background: Chronic Obstructive Pulmonary Disease (COPD) exacerbations result in significant morbidity, mortality, and healthcare costs. Understanding regional differences in clinical outcomes and healthcare utilization among patients hospitalized with COPD may provide insight into best practices in caring for this vulnerable patient population.
Methods: Using the National Inpatient Sample (NIS) database for the years 2016 to 2019, we compared adults hospitalized in the U.S. with COPD in the Northeast with those in the South regions. We conducted multivariable regression analyses to study in-hospital mortality, resource utilization, and post-hospital discharge disposition. By coupling ambient average temperature data for these regions that are contrasting in hotness, from the National Centers for Environmental Information database, to hospital admissions for COPD in the NIS, we explored associations and variations between the Northeast and the South
Results: From 2016 to 2019, 1,542,760 patients were admitted with COPD in these 2 regions; 463,830 (30%) were in the Northeast, and 1,078,930 (70%) were in the South; more admissions occurred in the coldest months. Those in the Northeast had higher odds of dying in the hospital (adjusted odds ratio {aOR}: 1.1 [1.0 to 1.2]; p = 0.03]) and were less likely to be discharged home after their hospitalizations (aOR,: 0.63 [0.61 to 0.65]; p = 0.03]) than those in the South. Patients in the Northeast had longer hospital stays (adjusted mean difference {aMD}= 0.23 days; 95% CI: 0.17 to 0.28; p < 0.01) and incurred greater hospital charges (aMD = $3,894; 95% CI: 2,358 – 5,429; p < 0.01) versus patients in the South. Throughout all months across the four-year study period, the average monthly temperatures in the Northeast were lower than in the South.
Conclusions: This study highlights significant disparities in outcomes for patients with COPD between the Northeast and South from 2016 to 2019. One striking difference between these regions is ambient temperatures; this is known to influence many factors associated with dyspnea – both patient and environmental variables. These results should remind clinicians and health systems to be poised to offer be even more diligent and attentive care to patients hospitalized with COPD during the colder periods.