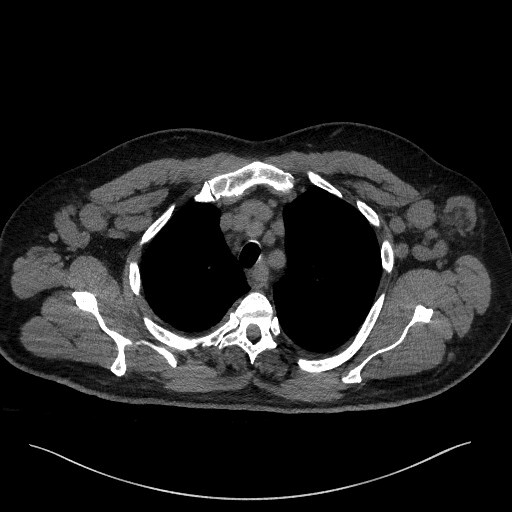
Case Presentation: A 63-year-old male with hypertension and a history of thalassemia trait presented to the ED for evaluation of two weeks of progressive malaise and widespread tender lymphadenopathy. One week prior, the patient started a course of doxycycline for presumed tick-borne illness by his primary care provider, but worsening symptoms along with diarrhea, vomiting, exertional dyspnea, and decreased urination despite the antibiotic therapy prompted presentation to the ED. Physical exam revealed posterior bilateral cervical, auricular, occipital, and axillary lymphadenopathy; and abdominal tenderness and distension. Initial differential diagnosis prioritized hematologic malignant versus infectious (viral or bacterial) etiologies, as prior tick-borne panel was negative. In the ED, the patient received supplemental oxygen for hypoxia, fluids, and empiric broad-spectrum antibiotics. CT imaging showed bulky multistation adenopathy throughout neck, thorax, and peritoneum, raising further concern for lymphoma. He developed thrombocytopenia, leukocytosis; acute kidney injury associated with decreasing urine output; and electrolyte imbalances including hyperuricemia, hypokalemia, and hyponatremia. He received rasburicase and allopurinol for presumed tumor lysis syndrome and a tunneled line was placed for expected chemotherapy. During admission, hematologic workup was unremarkable. Immunoglobulin testing did not show monoclonal growth patterns. Initial core lymph node biopsy showed only necrotic cells, and excisional lymph node biopsy redemonstrated predominantly necrotic cells with some viable immune cells without evidence of lymphoma. Renal biopsy was consistent with acute interstitial nephritis. Investigation of numerous infectious causes was also unremarkable aside from an elevated Epstein-Barr virus (EBV) by quantitative PCR to 9600 IU/ml. Considering decreased lymphadenopathy on repeated imaging studies and spontaneous symptomatic improvement with conservative management following antibiotic discontinuation, we concluded that the patient experienced an atypical EBV reactivation progressing to EBV viremia and he was discharged.
Discussion: While age and bulky diffuse lymphadenopathy on imaging were highly concerning for malignancy, this case identifies a severe presentation of EBV reactivation leading to acute renal failure, respiratory failure, and necrotic lymph nodes despite immunocompetent status. EBV viremia in symptomatic young adults is considered a primary infection, but cases of EBV viremia in older adults are considered to be reactivations of the latent virus (1). Oliguria and renal failure secondary to EBV infection, while rare, is most often manifested as acute interstitial nephritis (2) as was the case for this patient. The patient’s oliguria and fluid retention were believed to be the cause of his respiratory failure and ascites.
Conclusions: Over 90% of the global adult population has been infected with EBV and are seropositive upon testing (3). Though it is best known for its clinical presentation in young adults as infectious mononucleosis, most manifestations of primary EBV infections are subclinical (4). Reactivation is rare and typically triggered by host stress or immunocompromise (1,4). Despite its uncommon occurrence, EBV viremia must be considered in the differential when caring for patients with lymphadenopathy and vague symptoms of any age, particularly when bacterial and hematologic etiologies remain unsubstantiated.