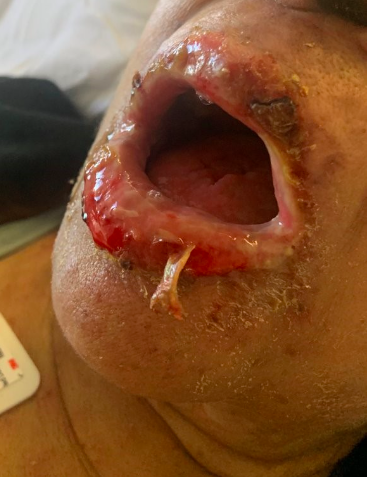
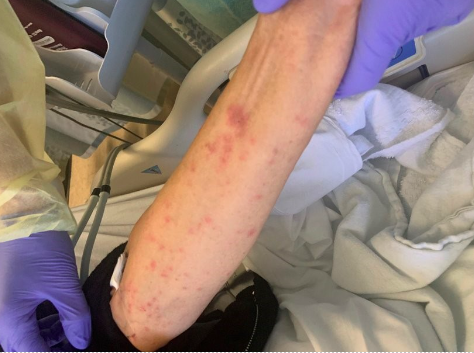
Case Presentation: 75 y/o F with metastatic anal cancer to lungs status post right lung lobectomy on leucovorin, oxaplatin and fluorouracil every 2 weeks, HTN and SLE presents with a 3-day history of weakness, sore throat, and mouth sores. Pt was in the Dominican Republic for 10 days and upon return, endorsed fatigue and sore throat which progressed to lip swelling and then purulent/pustular lip lesions. Associated symptoms included diarrhea and lightheadedness. Of note, the patient began chemotherapy 4 months prior with her last session 2 weeks before presentation. Chronic medications included hydralazine and labetalol. She denied any toxic habits or sexual activity. Vital signs were notable for persistent fevers up to 103F. Skin exam revealed hemorrhagic and yellow crusting of the lips, erosions of the buccal mucosa and nontender pink papules with purple to dusky centers, some coalescing, diffusely across her body including palms, sparing the face. Vaginal exam showed scattered similar ulcerations. Labs notable for positive covid PCR and ANA. Lupus flare and vasculitis serology, and extensive infectious work-up for bacterial, viral and parasitic causes were negative. Dermatology was consulted, had low suspicion for SJS and offered a broad differential including vasculitis, disseminated HSV/VZV, and reactive infectious mucocutaneous erosions (RIME) disease. Punch biopsies demonstrated extensive interface dermatitis resulting in subepidermal separation with overlying epidermal necrosis, narrowing the differential to SJS and RIME. Given her nontoxic appearance, a diagnosis of RIME disease was made and patient was started on prednisone 1 mg/kg for 3 days and clobetasol ointment, with subsequent clinical improvement. Patient discharged on steroid ointment with dermatology follow-up.
Discussion: RIME disease was formerly known as Mycoplasma-induced rash and mucositis (MIRM) disease because it was thought to be characterized by mucositis of 2 or more sites, and either no skin changes or a sparse vesiculobullous and/or targetoid eruption, typically associated with Mycoplasma pneumonia. The pathophysiology of RIME is poorly understood, but is thought to occur with molecular mimicry, namely between viral or bacterial proteins and keratinocyte antigens, leading to immune complex deposition. Since the categorization of this disease in 2015, other infectious triggers have been found, including chlamydia, influenza B, enterovirus, EBV, and hepatitis A. Few case reports in the literature have established a link between COVID and RIME. Our patient’s presentation supports COVID-induced RIME disease. This case will add to the literature for patients with mucositis and skin lesions in the setting of COVID. The case highlights teaching points to help differentiate SJS and RIME. RIME disease has predominantly mucosal involvement with variable cutaneous involvement, and good prognosis while SJS is characterized by rapidly progressive painful lesions encompassing a greater percent of body surface area, with an inciting trigger, and a poor prognosis. Treatment for both conditions typically consists of supportive care, steroids, and IVIG in select cases, in addition to treating any underlying triggers, or removing the offending agent.
Conclusions: When managing a patient with mucositis and significant cutaneous skin lesions, an internist must diligently rule out medical emergencies such as SJS/TEN. Being aware of COVID-induced RIME can help internists reach a correct diagnosis and provide proper management.