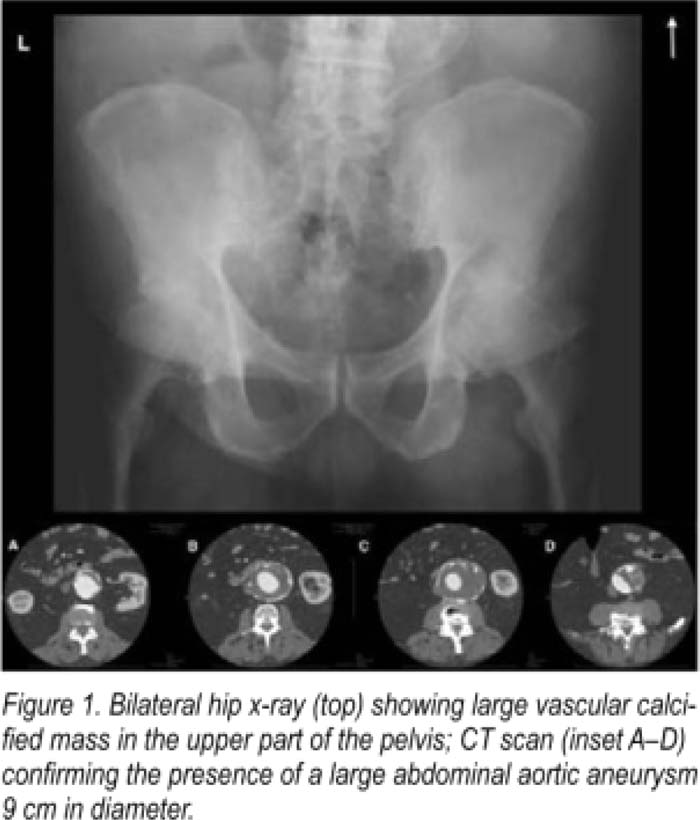
Case Presentation:
A 73‐year‐old white male with well‐controlled hypertension, type 2 diabetes, osteoarthritis, and gout presented to our preoperative clinic in anticipation of undergoing left hip arthroplasty. The patient had experienced left hip and back pain for 2 years that had become refractory to medical therapy. On clinical exam, the left hip was irritable to flexion, extension and internal rotation. There was mild tenderness over the greater trochanter. Mo abnormal chest, cardiac, neurological, or abdominal findings were noted. The patient's exam and Revised Cardiac Risk Index indicated a low risk for cardiac events (RCRI Zero, absolute risk = 0.6%). However, our perioperative consultant decided to review all imaging findings prior to proceeding. Routine x‐ray (Fig. 1, top) of the left hip performed earlier (read pending) confirmed osteoarthritis but also showed what appeared To be a large vascular calcification in The tower abdomen. An urgent CAT scan was ordered. (Fig. 1, A‐D, inset) confirming a large infrarenal abdominal aortic aneurysm measuring 9 cm in maximal diameter. The patient's hip surgery was cancelled and he was immediately started on statin and beta‐blocker therapy. Given the size of his aneurysm, he was urgently referred To vascular surgery for a same‐day evaluation.
Discussion:
Perioperative evaluation frequently involves a template, a “cookbook” approach usually inclusive of The eslimation and amelioraTion of cardiac risk (via RCRI), evaluation of functional and physical status, medical reconciliation, and recommendations on stress dose steroids or DVT prophylaxis. Our patient presented with what appeared to be a straightforward story without clinical findings of concern. It was only when “routine” x‐rays of the hip were reviewed that the imminent danger of a large aortic aneurysm was discovered. Our case thus highlights the often unspoken, yet crucial role of the perioperative consultant in reviewing evaluating and detecting abnormal disease via clinical, laboratory or imaging modalities that directly impacts operative risk. A through physical examination and a review of all testing is The foundation of perioperative risk evaluation. A simple “templated” algorilhm may have led to our patient undergoing operative intervention with the hemodynamic stress of surgery (sans beta‐blockers or statin treatment) potentially leading to a catastrophic outcome.
Conclusions:
Our patient underwent emergent endovascular repair of his large abdominal aortic aneurysm. His postoperative course was uncomplicated. He continues on lifelong statin and beta‐blocker therapy. He hopes to undergo hip replacement in the near future but vows to return to our clinic for perioperative evaluation prior to doing so!
Author Disclosure:
V. Chopra, none; J. Rohde, none.