Case Presentation:
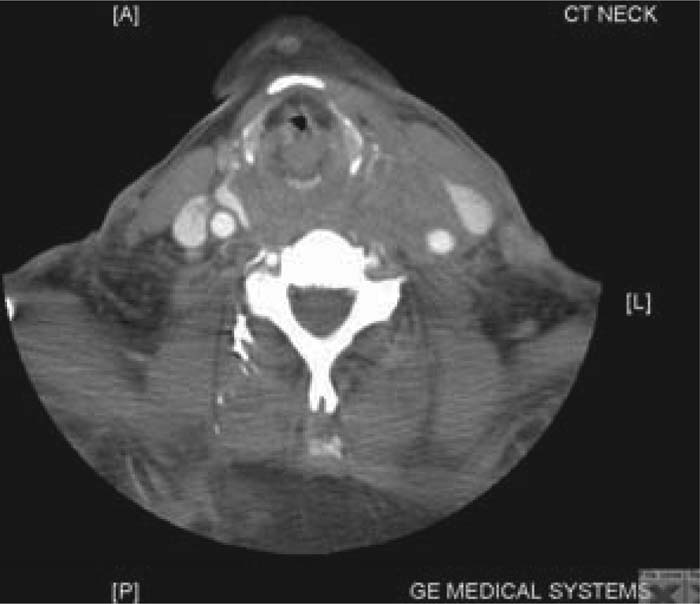
A 73‐year‐old man with diabetes and end‐stage renal disease was admitted with bilateral lower extremity cellulitis. He was also hypoglycemic, with a blood glucose of 29 mg/dL. Because of the difficulty obtaining peripheral IV access, cannulation of the left internal jugular vein using the Seldinger technique was attempted but was unsuccessful. No hematoma was present at the time. On day 2 in the ICU, he was noted to have fullness with mild bruising on the left side of the neck. He had no symptoms or signs of airway compromise. A CT scan of the neck showed extensive soft‐tissue swelling with severe airway narrowing. An emergent review by the ENT and vascular team was obtained. Because the patient was asymptomatic, the plan was to manage conservatively in the ICU with an endotracheal tube and a tracheostomy set at the bedside, 45° elevation of the head of the bed, frequent hematoma size checks, and daily soft‐tissue neck x‐rays. He did well, with evidence of gradual hematoma resolution, and he was discharged on the eighth day following diagnosis.
Discussion:
Central venous cannulation (CVC) is a frequent procedure, especially in the intensive care unit. Retropharyngeal hematoma as a complication of internal jugular vein cannulation is not common, even in patients with abnormal coagulation. In a large series of internal jugular vein cannulations in 1000 patients with abnormal coagulation from liver failure, only 1 patient, of 74 with inadvertent carotid artery puncture, developed a hematoma. A literature search from 1970 revealed 9 case reports of hematoma formation related to internal jugular vein cannulation, 5 of which had coagulopathy. The treatment of retropharyngeal hematoma in most cases is conservative, with close observation and repeated assessments of the size of the hematoma, as dyspnea can be sudden with a possible fatal evolution. The indications for surgical evacuation are airway compromise, very large size, and failure to improve with medical therapy.
Figure 1. CT scan of the neck with contrast showing extensive soft tissue swelling with severe airway narrowing.
Conclusions:
Ultrasound‐guided insertion of a central line is a helpful technique to gain venous access, especially in high‐risk patients such as those with coagulopathy, obesity, or unusual anatomy, as it is associated with a reduced number of attempts, better success rates, and reduced incidence of arterial puncture.
Author Disclosure:
O. Olaoye, none.