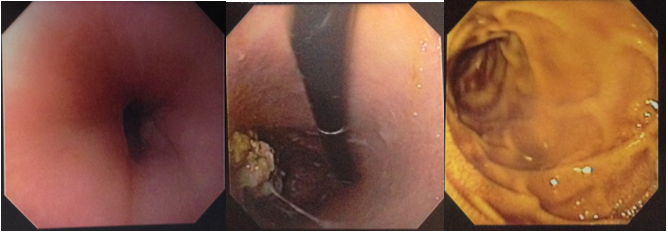
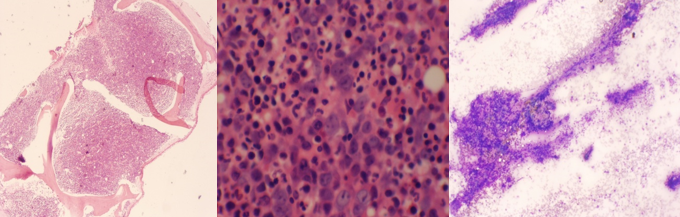
Case Presentation: The clinical manifestations of Pernicious Anemia are a result of cyanocobalamin deficiency and often slowly progressive and difficult to establish. In this case report we present a patient who presented with severe pancytopenia with constitutional symptoms including weakness, fatigue and weight loss mimicking a malignancy until after further workup proved otherwise. We describe a patient belonging to Hispanic/Latin-American Race ?Age with no significant past medical history who presented to the emergency department with complaints of epigastric abdominal pain, crampy, dull, constant, 10/10 in intensity and with no radiation. Patient admitted to feeling weak and lethargic for past 2-3 months. Also gave history of weight loss of 20 lbs in past 2 months prior to presentation. On examination the temperature 36.4C, pulse rate of 75/min, blood pressure of 113/69 and respiratory rate recorded 18 breaths/min. On physical exam pale conjunctiva were noticed. Patient was average built but with signs of mild to moderate malnourishment. Lab tests revealed an initial hemoglobin of 5.8 gm/dl, MCV of 100 fL, platelet count was 76,000 and WBC of 2,300 per mm3. Vitamin B12 levels were very low <50 pg/ml. Peripheral smear showed marked anisopoikilocytosis with tear drop cells and schistocytes. Bone marrow biopsy showed marrow consistent with severe cyanocobalamin deficiency and malignancy was ruled out. Anti- Parietal Cell (PC) antibody along with Anti-Intrinsic Factor (IF) Antibody were positive and a diagnosis of Pernicious Anemia was made.
Discussion: Pancytopenia with hemolysis as evident from elevated LDH, elevated bilirubin, schistocytes andthrombocytopenia in our patient. This is rarely seen in cyanocobalamin deficiency and seen in less than 5% of population in a study conducted by Anders E et al. There are some case reports where severe cyanocobalamin deficiency as masked as leukemias and thrombotic thrombocytopenic purpura. Antibodies to intrinsic cells are very characteristic of pernicious anemia and approach a sensitivity of 50-70% and specificity of 100% (8-9). These tests may help to make the diagnosis of PA in those patients who do not have positive anti-IF antibodies.
Conclusions: Our patient is very unique in the fact that he presented with not the classic features of pernicious anemia with neuropsychiatric symptoms including impaired memory, loss of dexterity and paresthesias. He also presented with a life-threatening hematological emergency which was fortunately recognized early. The patient was immediately started on Vitamin B12 intramuscular injections. His hematological parameters improved during the hospital stay. We thus propose an algorithm that may be very helpful in patients presenting with pancytopenia to help the clinician rapidly narrow the differential diagnosis. We advise strongly to include cyanocobalamin deficiency as one the top differential diagnosis in patients presenting with constitutional symptoms as this is a rapidly reversible and easily treatable disease. We also encourage retrospective, prospective and randomized control trials for finding the usefulness and importance of IF and PC antibodies in diagnosing pernicious anemia in pancytopenic patients with concomitant severe vitamin B12 deficiencies. Using these simple lab tests can quickly streamline such patients who can even get outpatient treatment with vitamin B12 supplementation.