Background:
End Stage Renal Disease carries a poor prognosis. Only half of dialysis patients are still alive three years after the initiation of renal replacement therapy. Furthermore, dialysis patients are hospitalized more often compared to the general population, averaging two admissions per year. We hypothesized that outcomes in dialysis patients are worse when they require hospitalization. Thus, we completed a population-based cohort study to measure the survival in dialysis patients following inpatient hospitalization, and to identify predictors of worse outcomes among these individuals.
Methods:
We retrospectively identified all Olmsted County, MN residents receiving dialysis who were admitted to a non-Intensive Care medical service at the Mayo Clinic Hospital in the calendar year 2014. Demographic information, and medical diagnoses based on ICD-9 codes were extracted from the electronic medical record. Patients with functioning kidney transplants were excluded. The primary outcome was patients’ survival after hospitalization. Kaplan Meier curve was generated for the cohort. Univariate Cox proportional hazards model was performed to test determinants of worse survival.
Results:
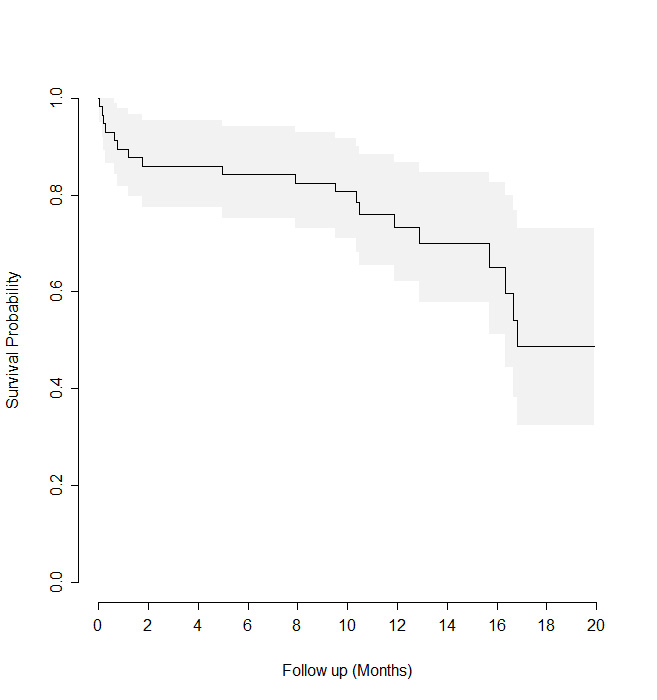
The cohort included 69 adult patients of whom 49% were male. Median age was 67 years (IQR 57-78). Median hospital stay was 3 days (IQR 2-3). Median number of admissions was 2 per year (IQR 1-3). Median Charlson score was 8 (IQR 6-10). Median follow up was 12 months. Median patient survival following hospitalization was 16 months.
There was a trend towards worse survival in patients with heart disease, pulmonary disease, liver disease, diabetes, and cancer. When these comorbidities were combined through a Charlson score calculation, the score was associated with worse outcomes (HR = 1.1, p = 0.05). There was also a trend towards worse outcomes in patients with frequent hospitalizations.
Conclusions:
Hospitalized dialysis patients have worse outcomes, with a survival that is around half that of the general dialysis population. Their survival correlates with their comorbidities, and each 1-point on the Charlson score carries a 10% decrease chance of survival after hospitalization. Identifying measures to keep these patients out of the hospital is important as it could potentially improve their long-term outcomes. Furthermore, it might be reasonable to consider a conservative/palliative approach in dialysis patients with multiple comorbidities who require frequent hospitalizations given their extremely poor survival.