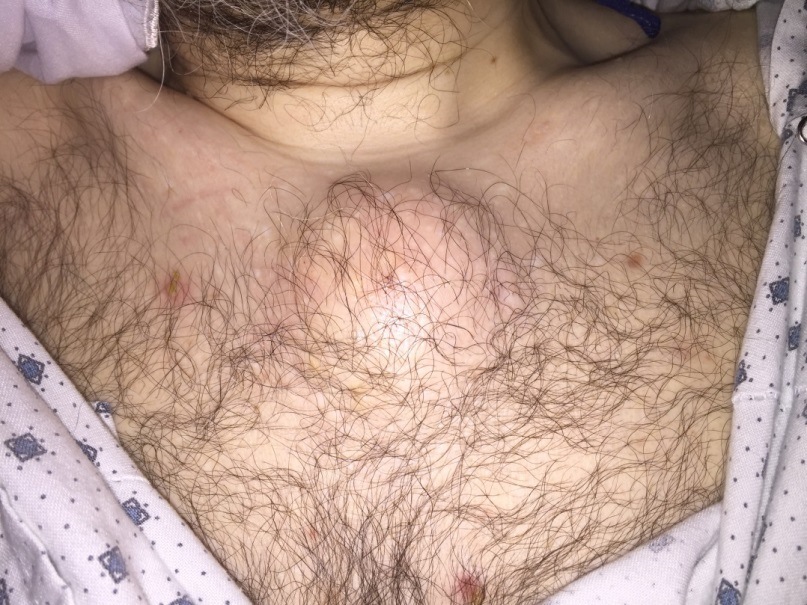
Case Presentation: A 55 year old male with history of ulcerative colitis and iron deficiency anemia presented to the emergency department with a 1 week history of progressive swelling, tenderness and erythema of a circumscribed area of his anterior chest. Similar lesions erupted over right 4th finger and right ankle 2 days prior to presentation. The patient denied hematochezia, melena, fevers, chills, or abdominal pain. Ulcerative colitis had been well controlled on sulfasalazine with no recent flares. He was admitted to hospital one year prior for osteomyelitis of left ankle, for which he completed 6 weeks course of antibiotics. Physical exam was notable for 4x3cm soft, tender, erythematous and fluctuant lesion overlying the sternum. No ulceration or drainage was noted. Similar erythematous and tender lesions were noted between MCP and PCP joints of right 4thfinger and lateral aspect of right ankle. Laboratory testing was unremarkable with exception of iron deficiency anemia. A CT scan of the chest was notable for a 2.6 x 4.2 x 2.1cm hypodesity concerning for abscess. Xray of hand and ankle revealed soft tissue swelling without evidence of osteomyelitis. Incision and drainage of chest wall lesion attempted, but no fluid was able to be aspirated. Blood cultures were negative, and TTE did not reveal evidence of endocarditis. The patient was admitted for IV antibiotics, however after several days his symptoms had not improved, so antibiotics were discontinued due to lack of evidence of active infection. Punch biopsy of right ankle lesion revealed pyoderma gangrenosum with vasculopathic pattern. Oral prednisone was subsequently initiated, resulting in rapid clinical improvement.
Discussion: We present an atypical case of pyoderma gangrenosum(PG) masquerading as abscess in a patient with ulcerative colitis. Pyoderma gangrenosum is an inflammatory, non-infectious, ulcerating skin disease associated with inflammatory bowel disease. PG incidence is not correlated with disease activity, in contrast to erythema nodosum.PG generally presents as an ulcerative or pustular lesion, unlike the erythematous and fluctuant lesions this patient exhibited. In absence of clear evidence of infectious process, and lack of improvement after antibiotics, skin biopsy was performed for definitive diagnosis of PG in this case. Pathology in PG typically reveals sterile dermal neutrophilia. Skin biopsy is valuable when differentiating PG from infectious ulcers, abscesses, or other inflammatory processes.
Conclusions: This case highlights an atypical extraintestinal manifestation of inflammatory bowel disease mimicking soft tissue abscess. When managing skin lesions in patients with IBD, clinicians should consider biopsy to definitively differentiate between infectious and inflammatory etiologies.