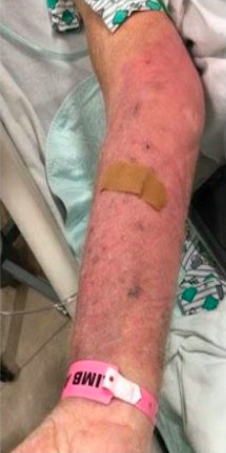
Case Presentation: A 76-year-old man with a history of chronic obstructive pulmonary disease (COPD), chronic kidney disease, and type II diabetes presented with dyspnea. He was diagnosed with a COPD exacerbation and COVID-19 infection and treated with IV and oral steroids during an 18-day hospitalization. Two days after discharge, he presented with right upper extremity pain and swelling. He recalled a dog scratch on his right arm a few days before his recent admission for dyspnea. He was admitted for cellulitis and treated with broad spectrum antibiotics and ultimately discharged on a short course of oral antibiotics. Over the next 2 months, he was hospitalized several times and prescribed numerous courses of varying antibiotics for refractory cellulitis with little improvement of his symptoms. Notably, he was maintained on steroids throughout this time due to ongoing wheezing and dyspnea. Skin biopsy 5 weeks after initial diagnosis of cellulitis yielded necrotizing granulomatous inflammation with numerous yeast forms. He was placed on itraconazole but was transitioned to IV amphotericin after fungal cultures grew Prototheca. After one month, he was transitioned to oral posaconazole due to worsening renal function. Steroids were also discontinued at this time. Therapy was changed to isavuconazole due to delirium and active infection on repeat biopsy. He achieved disease resolution after a 3-week course of isavuconazole and did not have recurrence.
Discussion: Prototheca is a genus of parasitic achlorophyllous algae of the family Chlorellaceae found ubiquitously in nature. Infection in humans is very rare, with only 211 cases reported in a systematic literature review in 2017. Only 61 of these cases were from the United States [1]. Infection by prototheca – protothecosis – has four recognized entities: cutaneous, olecranon bursitis, systemic, and disseminated. All presentations of infection are more common in the immunocompromised, with nearly 69% occurring in patients with immunosuppression, on corticosteroids, or both [1]. This case demonstrates a presentation of cutaneous protothecosis after three weeks of steroid exposure with no other history of immunosuppression. Bacterial cellulitis is a common clinical entity, with over 14 million cases in the U.S. annually. Most cases resolve with empiric antibiotics. Individual patient risk factors should be considered with heightened suspicion for atypical infection without improvement on standard therapy. Early utilization of skin biopsy for pathology and culture can aid in timely diagnosis. Due to the rarity of protothecosis, there is no agreed upon management. Here, infection failed to respond to itraconazole and posaconazole. A fair response was seen to amphotericin B, but use was limited due to renal toxicity. Finally, response was seen with isavuconazole, a relatively new 2nd-generation –azole antifungal.
Conclusions: While cellulitis remains a common clinical entity, atypical causes should be considered in high-risk patients and when infection fails to respond to otherwise appropriate empiric therapy. Protothecosis is a rare algal cause of cutaneous infection, but its timely diagnosis can be made with high clinical suspicion of atypical infection and early utilization of skin biopsy for pathology and culture. This case provides novel support for the 2nd-generation –azole, isavuconazole, in the management of cutaneous protothecosis.