Background: Newly graduated advanced practice providers (APP) face numerous hurdles in hospital medicine which may hinder the independent practice of APPs. APPs are tasked with assessing, diagnosing, beginning treatments, and discussing recommendations from various specialists with patients and their families. Despite overlapping responsibilities with physicians, there is wide variation in how APPs are prepared, both in terms of APP curricula as well as opportunities to apply skills prior to entering independent practice. For example, APPs complete 500-2,000 hours of clinical training depending on the program (NP versus PA) and institutional requirements. In contrast, physicians complete 12,000 hours of clinical training during residency. The expectation is that APPs can independently perform their duties immediately upon graduation, however the disparity in training reveals a need for programs that support transition to independent practice.
Purpose: One strategy to help new APPs transition to independent practice is through simulations (sims). Sims provide a safe learning environment for learners to participate in clinical scenarios and receive performance-based feedback. They are carefully designed scenarios that require active participation and decision-making. Learners are provided a framework for management of these patients, thus empowering novice APPs in independent practice.
Description: Over a 6-month period, each newly hired APP participates in our dedicated sim lab, led by experienced APPs. This lab has 7 clinical experiences focused on addressing goals of care, chest pain, respiratory failure, diabetes, sepsis, stroke, and pancreatitis with either a mannequin or paid patient actor. During the sim, APPs complete a history and physical and develop a treatment plan based on symptoms and clinical data. Scenarios can take unexpected turns, such as complications or patient decompensation. Following each sim, APPs have opportunities for self-assessment and a group debrief. APP leaders provide feedback to participants highlighting their strengths and identifying opportunities for development, then conclude with a satisfaction survey. Surveys use a 5-point Likert scale and capture pre- and post-sim satisfaction on content (i.e., clinical knowledge, topic relevance, facilitator effectiveness, and learning environment), overall level of confidence and readiness for clinical management, and suggestions for improvement.
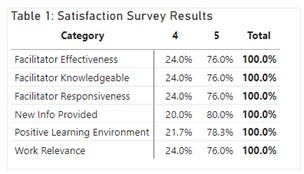
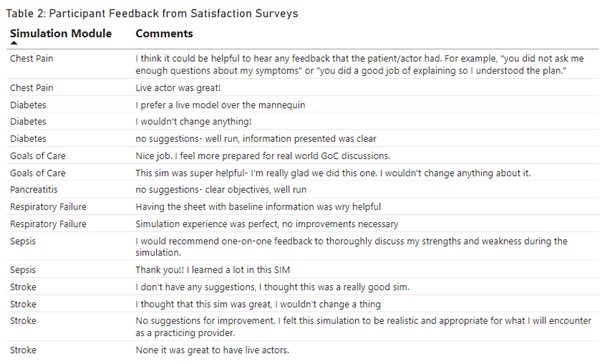
Conclusions: To date, 6 APPs completed 25 sims. In 76% (19/25) of surveys, APPs reported strong agreement that sims were relevant to their work and that facilitators were knowledgeable, effective, and responsive (Table 1). Most sims, 80% (20/25) provided APPs with new information suggesting that gaps in education are being addressed with 68% (17/25) reporting intent to utilize the information in practice. APPs’ comments (Table 2) suggest they felt more prepared for clinical practice and found value in these real-world simulations. Additional follow-up is ongoing to evaluate how education translates to practice over time and gain added insight on the lower scores to utilize the information. Additional sim topics of interest (e.g., antibiotic therapy, CHF w/ AKI), ideal learning modalities, and longer-term satisfaction are being collected which will inform our continuous improvement efforts for new APP orientation.