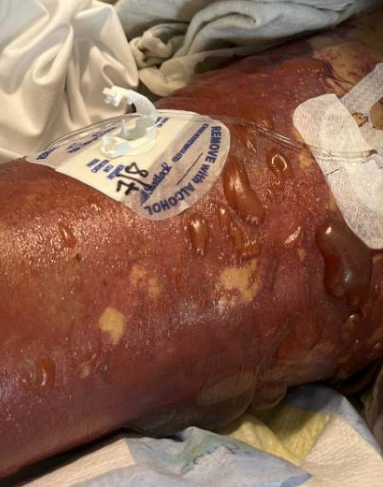
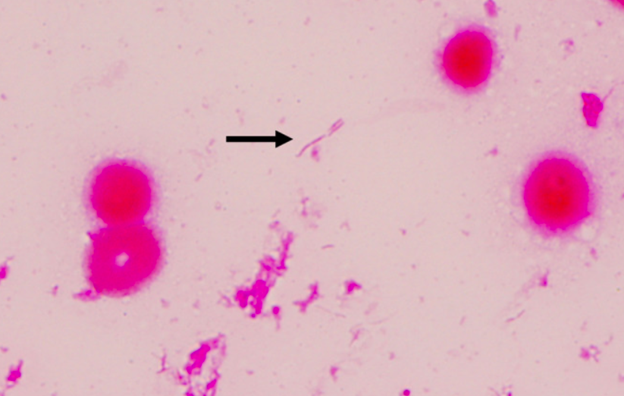
Case Presentation: A 54-year-old female with a past history significant for anxiety, tobacco, and alcohol use disorder presented to the emergency department with nausea, dizziness, weakness, and vomiting. Husband reports patient was bit by a dog on her right hand but denies any noticeable wound. He reports on the weekend she also had 2 episodes of nonbilious nonbloody vomiting. Last night at about 2:30 AM patient fell out of bed, which prompted husband to call 911. Patient drinks about 10-12 alcoholic drinks per day for the past 25 years, last drink was on Saturday per husband. Patient smokes about a pack and half per day for the past 40 years. On admission patient was found to be febrile to 104.4 F, with a BP as low as 79/36. Patient was also hypoxic with SpO2 of 48% and was placed on a nonrebreather 15 L but was subsequently intubated on admission for airway protection. On the physical exam diffuse mottling was noted throughout her entire body. Ecchymosis was found on her abdomen. A scratch wound was evident on her right hand without any local signs of infection, such as swelling or redness. Blood laboratory data indicated lactic acidosis with metabolic acidosis, elevated procalcitonin, pancytopenia, elevated troponin, hyponatremia, hypoglycemia, hypomagnesemia, and transaminitis. Enhanced computed tomography did not reveal the specific cause of the patient’s condition. An echo showed severely depressed left ventricular systolic function with an EF of 24%. Patient was started on appropriate inotropic, pressor support, and broad-spectrum antibiotics. It took greater than 48 hours for blood cultures to result and lab called stating an unusual organism was growing, later found to be Capnocytophaga canimorsus. Patient eventually developed multiorgan failure with disseminated intravascular coagulation (DIC). Despite empiric antibiotic therapy, aggressive fluid resuscitation (30–40 mL/kg crystalloids), transfusion (platelets, fresh‐frozen plasma, and red blood cells), vasopressors, steroid application, and continuous renal replacement therapy, the purpura spread throughout her body. Repeat imaging revealed amorphous fluid collection seen medial to the spleen. This fluid was not present on admission. At that point family decided to withdraw care, patient was compassionately extubated and expired at medical facility.
Discussion: We have described a case of C. canimorsus infection that resulted in mixed shock, septic/cardiogenic, and eventual death. It is important to note that this patient was immunocompromised as she did have alcohol-associated cirrhosis. Life-threatening infection with this gram-negative bacillus/rod typically occurs after a dog (or cat) bite/scratch or exposure to dog saliva in patients with asplenia, functional hyposplenism, history of excessive alcohol use, or cirrhosis. The increased risk for C. canimorsus infection in patients with asplenia/splenic hypofunction results from an impaired ability to clear intravascular bacteria and deficient antibody production. Management includes supportive care, empiric antibiotics with a carbapenem or a β-lactam/β-lactamase inhibitor combination, and possible surgical debridement.
Conclusions: It is important for physicians to recognize life-threatening infection with Capnocytophaga canimorsus in immunocompromised individuals typically occurs after a dog (or cat) bite/scratch or exposure to dog saliva for early diagnosis, management, and treatment. Two cases were found in our ICU during the summer months.