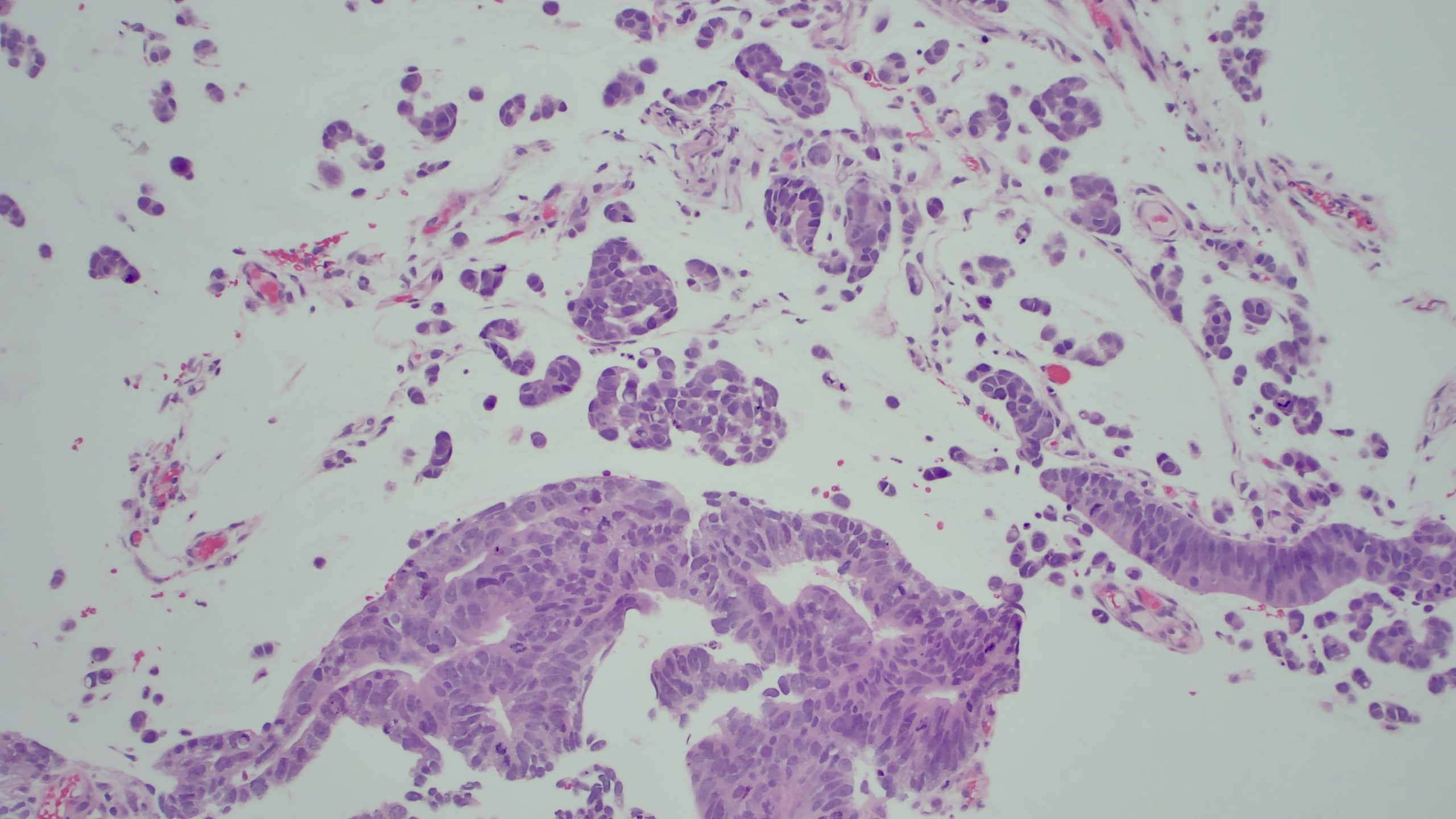
Case Presentation: A 49-year-old female with no known past medical history presents with worsening symptoms of abdominal discomfort, bloating, and shortness of breath for one month. Upon presentation, vitals were significant for tachycardia. A CT scan of the abdomen and pelvis showed hepatic steatosis with a large volume of ascites. A paracentesis was performed and six liters of fluid were removed and sent for microbiological and cytologic analysis. Patient received albumin and was discharged. Three days later, the pathology results returned and were consistent with adenocarcinoma with mucinous features. The patient was called back by the hospitalist to return for further workup. CDX2 and CK20 staining were suggestive of malignancy of colorectal origin. A pelvic ultrasound was ordered to rule out ovarian tumors and showed soft tissue nodules within the right adnexa, suggestive of metastatic peritoneal implants. A CT scan of the abdomen and pelvis with contrast showed soft tissue fullness involving the sigmoid colon and an underlying colonic neoplasm, as well as a moderate to large amount of ascites with probable omental caking. A colonoscopy was performed and revealed 30 cm mass in the sigmoid colon. Biopsy reports revealed poorly differentiated colorectal adenocarcinoma with signet ring cell morphologic features with negative microsatellite instability. Tumor markers were positive for PMS2, MLH1, MSH2, and MSH6. The patient was determined to be a candidate for the FOLFOX6 chemotherapy regimen.
Discussion: Ascites is associated with portal hypertension and liver cirrhosis in approximately 85% of cases in the United States. However, patients with undiagnosed malignancies including those of the ovary, breast, colon, lung, pancreas, and liver may present with a similar clinical picture and may account for approximately 7% of cases. Ascitic fluid analysis via paracentesis is essential for the diagnosis of malignant ascites. In patients with prior findings of liver pathology, ascites may be wrongly attributed to liver cirrhosis as opposed to underlying malignancy. Cytology should be sent on all ascitic fluid samples for patients suspected of having malignancy-related ascites. This case highlights the importance of diagnostic paracentesis in patients with ascites, especially those at risk of developing cancer, to ensure early detection and prompt treatment.
Conclusions: This study highlights the importance of considering malignancy as a differential diagnosis when patients present with ascites. As the incidence of colorectal malignancies increases, it is vital that we have the need for early diagnosis and diagnostic paracentesis in patients with comorbidities placing them at higher risk of malignancy.