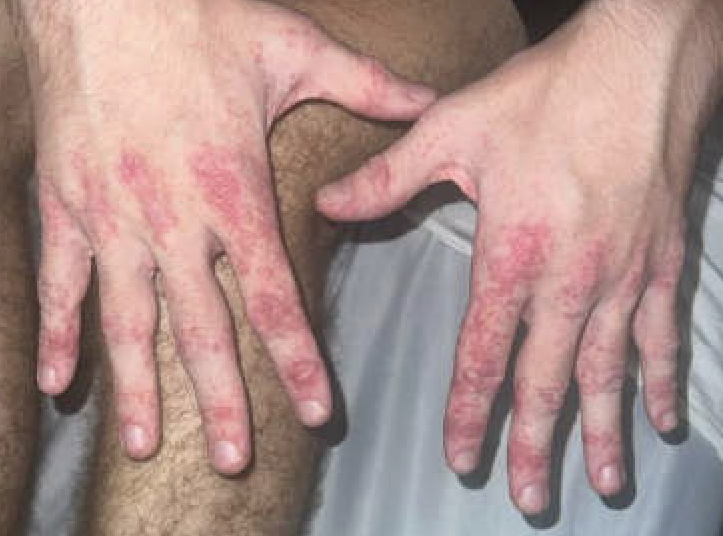
Case Presentation: A 17-year-old male with no significant past medical history presented for a diffuse rash and shoulder girdle weakness. One month prior to presentation he presented to an urgent care clinic with generalized fatigue, ear pain, cervical lymphadenopathy, and sore throat. He was initially prescribed a course of amoxicillin-clavulanic acid. He completed two days of this; however, he had worsening symptoms and was prescribed a seven-day course of cefdinir and seven-day prednisone taper. He subsequently had a positive result on rapid mononucleosis screening; cefdinir was stopped at that time. After 2-3 days of his prednisone taper, he developed a diffuse, erythematous rash. For the three weeks following his prednisone taper, he also noted shoulder girdle weakness which was only present in the morning. The day prior to and of presentation, the weakness did not improve throughout the day. The physical exam revealed 3/5 proximal shoulder muscle weakness, and a rash consisting of papules coalescing into erythematous plaques with scale on the bilateral dorsum and palms of the hands, bilateral elbows and knees, and bilateral medial ankles and dorsum of the bilateral feet. Additionally, Gottron papules were present on the bilateral hands. Labs revealed normal serum aldolase, negative ANA, and normal ESR. Imaging did not identify inflammation of the hip girdle muscles. A punch biopsy was performed and showed interface dermatitis with subjacent superficial and periadnexal lymphocytic infiltrate which was consistent with the diagnosis of dermatomyositis in this clinical context. He also had a positive IgG and IgM for Epstein Barr virus, positive IgG for parvovirus B-19, and an elevated CRP of 1.19. NSAIDs were started with some mild symptomatic improvement. After evaluation by dermatology and rheumatology, he started treatment for suspected juvenile dermatomyositis with a prednisone taper. He initially had marked, rapid improvement in his rash and muscle weakness, however after weaning his steroids from 30 mg daily to 20 mg daily, he had a flare of his rash.
Discussion: Juvenile dermatomyositis is a reasonably well-described condition in the literature1,2. Additionally, Epstein Bar Virus (EBV) has a variety of clinical manifestations and may serve as a trigger for a variety of inflammatory and rheumatologic conditions, including systemic lupus erythematosus and dermatomyositis, and may have implications in multiple sclerosis3,4. In this clinical vignette we presented a case of dermatomyositis probably triggered by EBV in which a careful history and thorough physical exam were key factors in clinching the diagnosis. This case presented several confounding factors, including the patient’s recent EBV diagnosis and prior steroid taper, that muddied the clinical picture. Upon presentation, his physical exam was consistent with myositis as he had significant (3/5) weakness of the bilateral upper extremities, and shoulder MRI- though low quality- showed edema in the left deltoid, indicative of inflammation at that time.
Conclusions: This case demonstrates the critical nature of the hospitalist’s careful history and thorough physical exam in a complex presentation, even in the presence of negative test results. The prior steroid taper may have reduced some inflammation, potentially affecting the lab results. Despite this initial treatment, it was the provider’s keen clinical insight and careful evaluation that led to the accurate diagnosis and appropriate management for this patient.