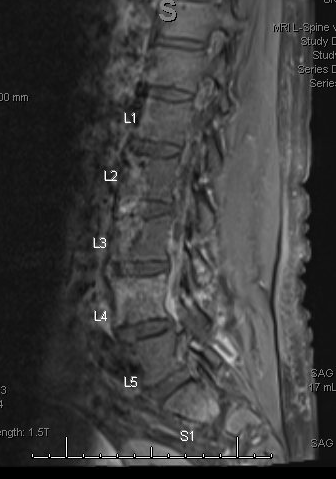
Case Presentation: Bacterial osteomyelitis is very challenging to treat. This is partly due to the widespread antimicrobial resistance to gram positive bacterium Staphylococcus Aureus. We present a severe case of disseminated staphylococcus aureus osteomyelitis, that includes bacteriemia, psoas abscess, infective endocarditis, osteomyelitis, septic arthritis of knee and shoulder joints. A 63-year-old woman with poorly controlled type II diabetes mellitus, ASD occluder device presented to the emergency department (ED) with complains of several days of low back pain. Patient had significantly elevated CRP of 23.4 mg/dL and a mildly elevated lactate of 2.3 mmol/L on presentation. An extensive work up including MRI of the lumbar and thoracic spine were negative for infection. As MRI was reassuring and patient clinically improved, she was discharged home. Patient was called back the next day as her blood cultures were positive for Methicillin-Susceptible Staphylococcus Aureus (MSSA) bacteremia. Patient was started on IV cefazolin. A TTE on admission was negative for intracardiac vegetations. Patient continued to have severe back pain in the setting of persistent MSSA bacteremia. MRI L spine repeated four days later showed extensive infection with osteomyelitis and discitis of L4 as well as bilateral psoas abscesses. Patient had seeding to her right shoulder requiring incision and drainage, and left knee washout twice for septic arthritis. Due to blood cultures showing persistent bacteremia with multiple sites of infection, IV ertapenem was added to provide salvage therapy for persistent bacteriemia. TEE a week later showed a new vegetation on ASD device. As this was a new seeding, patient’s antibiotic was changed to IV nafcillin with continued synergy with IV ertapenem. Cardiothoracic surgery was consulted but declined to intervene due to high risk and no compromise of cardiac function. Patient underwent drainage of psoas abscess with interventional radiology. Orthopedic Spine recommended continued medical management. Patient’s blood cultures remained persistently positive for two weeks after which they were finally negative. Patient was discharged with six weeks of outpatient parenteral antibiotic therapy (OPAT). Patient has had three OPAT appointments so far and has improved dramatically while on IV antibiotics.
Discussion: This case illustrates the severe pathogenicity and rapid course of MSSA bacteremia in the setting of an early negative imaging. This case also highlights the critical importance to keep a close vigilance on other sites of infection. This report is unique how MSSA was successfully treated.
Conclusions: Although published data is limited, synergy for the antibiotic combination cefazolin and ertapenem has been demonstrated with rapid bacteremia clearance in refractory cases. This case is an important contribution to the developing knowledge of MSSA bacteremia and will assist clinicians in performing thorough and timely septic investigations.