Background: Early palliative care can be beneficial for patients and the health system alike. The principle of palliative care is to improve quality of life through patient-centric treatment goals and comfort measures. However, many patients are identified and receive palliative care in their last days of life where hospice is more appropriate. Hospitalists are routinely asked to identify patients who would benefit from a care conversation using the “Surprise Question,” which involves a physician reflecting on: “Would I be surprised if this patient died in the next 12 months?” We aimed to determine if a simple palliative care screening tool could enable hospitalists to more easily identify these patients.
Methods: Charts from 110 patients, admitted to the oncology/general medicine unit at the Shady Grove Medical Center (Rockville, MD), were individually reviewed by a palliative care physician between December 26, 2016 and February 2, 2017. Chart review was performed within 72 hours of patient admission. The Palliative/Surprise Screen Test (PSST), a modified palliative care screening tool adapted for use in this patient group, was completed for these patients (Figure 1). The attending physician was notified of all patients who were positive on the PSST and asked if a palliative medicine consult was wanted. Existing hospice referrals were also noted.
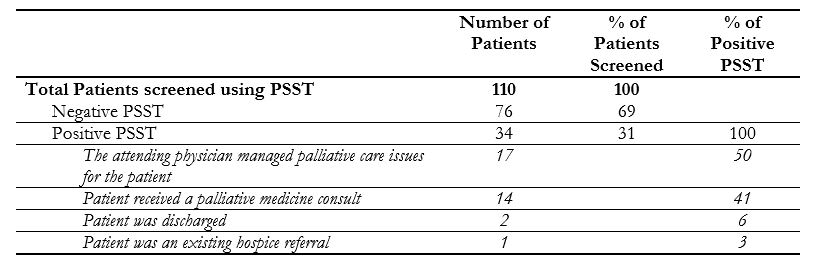
Results: Out of the 110 patients who underwent chart review and were screened using the PSST, 34 patients (31%) had a positive PSST (Table 1). Of the 34 patients with a positive PSST, the attending physician requested a palliative medicine consultation for 14 patients. The attending physician opted to address issues of symptom management or goals of care conversations themselves for 17 patients. Two patients were awaiting discharge when the attending physician was notified, and one patient was an existing hospice referral. Notably, we did not capture data on patients with advanced hematological malignancies, symptomatic but unconfirmed malignancies at admission, and patients initially admitted to other units and later transferred. Additionally, some charts were missing information about previous hospitalizations, functional status, or other parameters.
Conclusions: Timely assessment of patients that may be appropriate for palliative care should be considered for all critically ill patients to help improve their quality of life. Nearly one third of patients admitted to the oncology/medicine unit were identified using the simple PSST tool to potentially benefit from palliative care interventions performed by either a palliative care team or a hospitalist. We recommend including the PSST in education modules for hospitalists to more easily identify these patients when asked the “Surprise Question.”